I realized yesterday that many consumers might not even know what a PBM is. PBM stands for pharmacy benefit manager. The market is dominated by 3 large players – Medco, Caremark, and Express Scripts. After that, you have several mid-sized players – Walgreens, Pharmacare (which is now being integrated into CVS/Caremark), Prime Therapeutics, MedImpact – and lots of captive (i.e., part of a managed care company) PBMs – Wellpoint, Aetna, Cigna. And, finally, you have PBMs like Argus that primarily process claims for companies like Humana. (Here is a directory of most of the PBMs.)
Typically, a PBM has the following functions:
- Process pharmacy claims (i.e., when you go to your retail pharmacy, the pharmacist enters your prescription and electronically submits it for adjudication. The claim is routed to the PBM where it is checked for eligibility and then to see if it pays and what copayment you owe)
- Set up pharmacy benefits (i.e., based on the plan selected by your employer or payor, the PBM codes what drugs are covered and the copayment structure)
- Administer rebates…since large pharma companies (e.g., Pfizer) pay rebates for having their drugs on formulary (aka preferred drug list), someone has to manage the negotiations and billing of this.
- Set up clinical programs (i.e., most PBMs have a clinical committee which evaluates new drugs and looks at market data to help employers choose coverage options)
- Establish a retail pharmacy network (i.e., work with retailers to get them to agree to discounts on drugs)
- Communicate with patients and physicians (i.e., look at pharmacy claims data and help find ways to save money or identify clinical issues to inform the patient or physician about)
- Provide cross pharmacy data for drug-drug interactions…this is a critical function since many people use more than one pharmacy for claims
- And, last but not least, most PBMs provide a mail order and often specialty pharmacy where they ship prescriptions to patients.
The PBM’s clients are employers who are self-insured, government entities (i.e., state employees, DoD), unions, TPAs (third party administrators), and managed care companies (i.e., BCBS of). Since healthcare has not traditionally been a consumer focused business especially in the PBM world, many of you might not know who your PBM is. In some cases, the managed care company may make it basically invisible to you.
The only people that likely have good awareness of their PBM are high utilizers who run into lots of claims questions and/or people who use the mail order service.
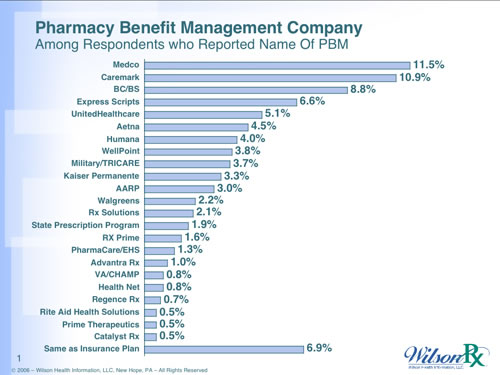
WilsonRx does surveys around PBMs Learn More. Here are two charts from their website about who people name as their PBM and satisfaction with their PBM.
If you like this post and are interested in the topics here, don’t forget to sign up for my e-mail updates or add the RSS feed from the blog to your reader.

 October 12, 2007
October 12, 2007 



Where would Costco fit into all this? I’ve heard good things about their presription drugs, as well as having good prices.
I was doing some research regarding Healthcare ISVs in the following segments: Pharmaceutical Benefits Management (PBM), Health Insurance, and Hospitals. Is there anyone who could tell me who the top three ISVs are in each segment?
http://en.wikipedia.org/wiki/Pharmacy_Benefit_Management
PBM’s are the much required focal points that bring together pharmacies, patients, plans and employers. Without PBMs, other entities would face increasing challenges in providing affordable drugs in the absence of PBM negotiated prices.
I can not agree with you in 100% regarding some thoughts, but you have got a good point of view. Thanks for your thoughts.