I can’t believe it’s taken me a few weeks to catch up on my notes from a conference call with David Snow and Dr. Rob Epstein from Medco Health Solutions about their 2010 Drug Trend Report. I captured some of Dr. Epstein’s comments in a quick blog post, but I have a lot of respect for David Snow and wanted to capture a few of his comments here and pull out some of the interesting data from the Drug Trend Report.
David Snow mentioned a few things:
- Reform has to address all three legs of the stool – Access, Quality, and Cost. Right now, it’s focused on access.
- Of the $2.4T we spend in the US on healthcare, $1T of it was unproductive.
- One of the big issues in the system is poorly designed systems for the people that deliver care.
- Pharmacy is ahead of the curve since it’s already wired and uses evidence-based care.
- We have to focus on the chronic conditions. 96% of the pharmacy spend and 75% of the medical spend is here.
- Prescriptions are used as first line solutions 90% of the time. (See my comments on why trend shouldn’t matter.)
- $350B of the waste is due to poor management of chronic solutions.
- We still have to address medical liability and defensive medicine.
He also answered questions. A few of my notes from the Q&A:
- Patent expiration doesn’t fully explain the increase in brand pharmaceutical costs. (Traditionally these drug costs go up once the patent expires.) You can correlate the tax on pharma (in reform) to the increase in prices. (Not dis-similar to the increases around Part D if memory serves me.)
- Adherence is a key issue. The Therapeutic Resource Centers (TRCs) are their answer to this. They drive adherence in the classes that matter and we report to clients on this. (While I think a lot of people viewed the TRCs as marketing strategies when they first came out, I believe they have demonstrated a clinical focus with some case studies and clinical leads over the past 18 months.)
- The pathway to biosimilars is very fair to the innovator.
- Class competition in specialty is increasing.
His most interesting comment which I’ll repeat from my earlier post was that if the FDA really understood true adherence they might make different decisions on approving drugs whose effect is tied to a person staying on a medication over time.
I won’t repeat some of the core data elements from my prior post, but here are some new ones from reading the document:
- Mail order penetration was 34.2% (which I believe is industry leading for the PBM sector with only Walgreens showing a 90-day utilization number that’s higher).
-
Interestingly, they show trend for clients with over 50% mail use (and clients with less than 50% mail use). [Most PBMs would love to have any clients with over 50% mail use.]
- 0.1% for those with over 50% versus 5.3% of those under 50%
Reported trends are based on 2 years’ data on pharmaceutical spending. Drug trend percent includes 201 clients representing approximately 65% of consolidated drug spending. The sample comprises clients who offer integrated (mail-order and retail) pharmacy benefit options for members. Clients with membership enrollment changes > 50% were excluded from the analysis. Plan spending is reported on a per-eligible per-month (PEPM) basis, unless otherwise specified. An “eligible” is a household, which may include multiple members who are covered under the same plan. Plan spending comprises the net cost to plan sponsors less discounts, rebates, subsidies, and member cost share. Generic dispensing rates and mail-order penetration rates represent the total consolidated Medco client base.
- Diabetes is obviously a critical category for everyone. I found it interesting that they saw fewer patients filing claims for diabetes but more drugs per patient in 2009.
- Respiratory therapies (driven by those <19 years old) jumped in contribution to trend from 8th to 2nd.
- In patients aged 35 to 49, antiviral drugs are the greatest contributors to cost – 8.3% of plan pharmacy costs. [Some of this driven by flu although this is not the at risk age group.]
Antiviral drugs (Formulary Guide Chapter 1.8) include oral treatments for HIV/AIDS, influenza, herpes, hepatitis C, hepatitis B, and injectable treatments for respiratory syncytial virus (RSV), and cytomegalovirus.
- Utilization growth for ADHD drugs for those age 20-34 grew 21.2%. [Is this for people not diagnosed as kids, people who have adult-onset ADD (if that exists), or just an over-diagnosis of the condition?]
- Specialty drugs…I’m always surprised that all the PBMs still have to caveat the fact that they only adjudicate some of the claims since some specialty drugs are filled and billed under the medical benefit. That seems like something that should / could be fixed, but I know it’s been tried and is hard since people are making money off them being billed elsewhere.
-
Cancer is already a huge driver of specialty costs AND:
- Much of the spending is still under medical;
- Most drugs approved in the past 4 years costs over $20,000 for a 12-week course; and
- There are over 800 drugs in the pipeline.
Spending growth has outpaced spending for nonspecialty, or traditional medications because:
- A high proportion of newly approved drugs are designated as specialty.
- Unique manufacturing processes make specialty drugs expensive to develop.
- Fewer drugs within a therapeutic category limit competition.
- There may be only one specialty treatment for an orphan condition.
- Few drugs are therapeutically equivalent to others in the category, reducing interchange and related cost savings opportunities.
- It is more difficult to transition existing patients from one specialty drug to another preferred specialty drug because often these drugs are large, unique proteins that are not considered interchangeable.
- Most small-molecule specialty drugs are relatively new with few generic alternatives.
- No defined approval pathway exists for follow-on biologics (also known as biosimilars).
- Drugs used to treat cancer represent a large portion of new drugs in both the pipeline and marketplace; most are specialty drugs and some can cost more than $20,000 for a 12-week therapy course.
- It was the first time I noticed anyone caveating the specialty trend. They proactively addressed different calculation methods to point out that their method yielded a 14.7% specialty trend, but if you did things differently (as I assume others must), then their trend would have been 12.1%.
- Trend in children exceeded trend in other age groups for the second year in a row. (I think this is an interesting perspective and a scary indicator for the future health of our country.)
-
They provided some examples of drugs that had new indications for younger patients approved:
- WelChol, Crestor—for low-density lipoprotein cholesterol (LDL-C) reduction in children aged 10 to 17 with heterozygous familial hypercholesterolemia.
- Atacand—for hypertension in children aged 1 to 17.
- Axert—for acute treatment of pediatric migraine.
- Protonix—for erosive esophagitis in patients aged 5+.
- Abilify—for irritability associated with autistic disorder in children aged 6 to 17.
- Seroquel—for schizophrenia in children aged 13 to 17, and for acute manic episodes in children aged 10 to 17 with bipolar I disorder.
- Zyprexa—for schizophrenia and for acute mania (bipolar I) in children aged 13 to 17.
- WelChol, Crestor—for low-density lipoprotein cholesterol (LDL-C) reduction in children aged 10 to 17 with heterozygous familial hypercholesterolemia.
- An interesting perspective that I’ve talked about many times (without the research capabilities to analyze) is the correlation between sleep and chronic disease. They looked at this across states based on drug utilization and found a correlation (not necessarily causation).
So what do they say to watch:
- Continued inflation in brand drug prices.
- Majority of trend will come from specialty – oncology, orphan conditions.
- Personalized medicine.
- Biosimilars.
- Generic pipeline.
- Obesity epidemic.
- They bring up an interesting issue relative to OTC (over-the-counter) product which is DUR (drug utilization review) which looks for drug-drug type interactions. They talk about the Medco Health Store integrating that data to monitor patients. [Do plans care? Do patients care? Should retail OTC purchases be integrated? How great are the interactions?]
-
They talk a little about obesity although I would love to understand more about how a plan sponsor should manage this.
- 68% of adults are overweight; 34% obese
- 32% of children are overweight; 17% obese
- Medical spending on obesity related conditions is $147B
- 19.5M adults (24-85) have diagnosed diabetes and other 4.25M are undiagnosed
- Diabetic medical claims are forecasted to grow from $113B to $336B over the next 25 years.
- I’m not going to spend a lot of time on personalized medicine here. (A recent post of mine on this topic.) They’ve been very active in this space for years talking about it. I think one of their interesting points in the Drug Trend Report is how Comparative Effectiveness will dovetail with Personalized Medicine.
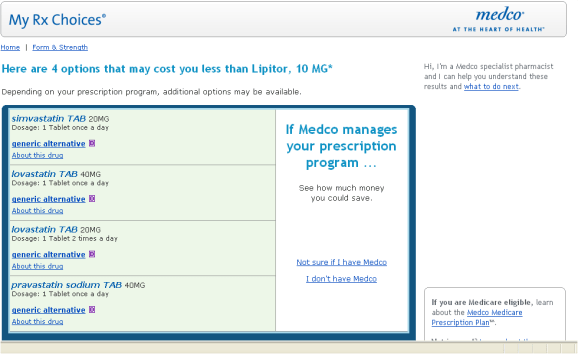
- Almost 2/3rds of people at risk for CHD in the next 10 years and eligible for lipid lowering drugs (e.g., Lipitor) were still not using them. (A common gap-in-care program run by many companies is to target these people (e.g., diabetics).)
- Only 29% of patients treated for high cholesterol reach their cholesterol goal.
- They have a section on wiring healthcare which David Snow has talked about for a while. It’s a critical area to address and has lots of opportunity.
- They also talk about the concept of collaborative care (aka medical home…aka accountable care organizations).
- I’m a big believer that poly-pharmacy creates issues (as does poly-physician). I don’t hear much talk about it. I was glad to see them talk about a study they did which identified poly-pharmacy issues, talked to MDs, and ended up with 24% of cases where medications were changed.
A Medco survey reported that 81% of participants with a new diagnosis, who received services at a traditional retail pharmacy, either did not receive counseling or were dissatisfied with the prescription drug counseling they received. When given the opportunity to speak with a Medco Specialist Pharmacist, 75% of these patients accepted the offer of immediate telephone support.
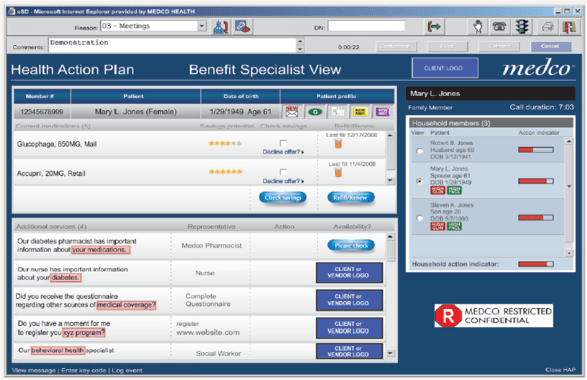
- I thought it was really interesting to see a screen shot of their application used by the TRCs to create their Health Action Plans for consumers.
- I was also interested in their focus on women’s health and some data on caregivers and the gender differences in healthcare. One of their TRCs is dedicated to addressing these differences.

 June 9, 2010
June 9, 2010