Last week, I had a chance to sit down with Dr. Hawk right after his presentation at the World Health Care Congress (WHCC). Dr. Hawk is the Vice-President and Division Head for Cancer Prevention and Population Sciences at the University of Texas M. D. Anderson Cancer Center. He’s been there since late 2007 when he came from the National Cancer Institute.
My favorite point from talking to him was…
Cancer is a process not an event. Communication is critical.
In his presentation, he talked about several things:
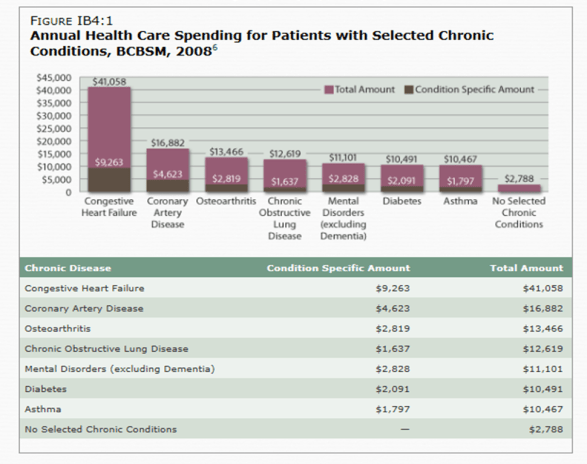
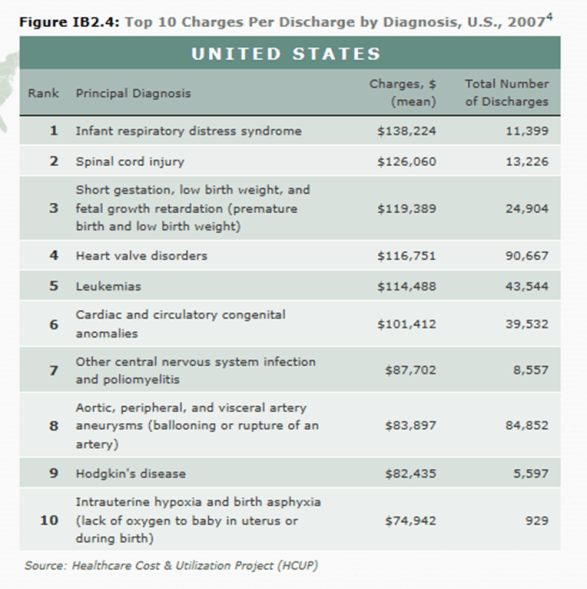
- The $227B total cancer cost in the US (2007).
- The personalization of risk assessments and interventions.
-
The services of MD Anderson.
- Mortality reductions
- Wellness education
- Vaccinations and chemoprevention
- The US Preventative Services Task Force.
- The work that they’re doing direct with an employer (Shell).
- The CEO Cancer Gold Standard.
- The impact of aspirin on all-cause mortality.
So, after his formal presentation, we talked about several things.
- One of the big focus areas for MD Anderson is prevention. As we know from research, many cancers are preventable. And, the promise of personalize medicine and genetic testing is beginning to help us understand these cancers and their treatments even more.
-
- Primary – this would include lifestyle changes such as diet and smoking which help prevent the disease
- Secondary – this would include screening and detection to help slow the progression of the disease
- Tertiary – this would include the focus on the patient (not the tumor) for treatment and helping them with quality of life
- He talked about how cancer is really 200 different diseases to be understood and managed.
- He gave a great analogy about how CVD (cardio-vascular disease) evolved and talked about how all the individual risk factors became asymptomatic diseases which have led to all the “know your number” campaigns around lipids and blood pressure.
- We talked about cancer as a process which led us into the discussion about palliative care and shared decision making. He made another good analogy here about driving a car. We need to understand the value of wearing our seat belt and having insurance, but we have to make the final decision about whether to do that or not.
- We talked about personalized medicine including genomics and epigenetics. We talked about how this impacts dosing and understanding of the tumor. (Interesting in a conversation with another person in this field this week they were telling me about how tumors and viruses change over time and those implications on genetic test results.) We also talked about SNPs and the complications in getting validation in studies due to sample sizes. We wrapped up this topic with discussions on coordinated registries and work that companies like 23andMe are doing.
- Our final topic of discussion was around clinical practice algorithms and how evidence-based medicine (EBM) gets implemented. We talked about the use of guidelines and how those allow for monitoring the use of EBM standards. We also talked about the need for integrated EMRs that would allow for benchmarking and linking outcomes to use of guidelines.
This is a fascinating area. Cancer affects most of us either directly or through some family member or friend.


 April 26, 2012
April 26, 2012