My Favorite Posts From 2011
I shared with you what got the most traffic on my blog in my last post. Let me look back at 2011 and note some of my favorite posts:
- New Pharmacy Whitepaper: Innovate Or Be Commoditized
- PCMA Interview – The Core PBM Skill: Adaptability
- Trust As The Foundation For Healthcare Communications
- Specialty Rx Offerings Not Rxs Only
- Walmart: Good or Bad for the PBMs
- 15 Things You Should Know About Prescription Non-Adherence
- The Implication Of Personal Decisions On Health
- 5 Indicators Of Pharmacies Crossing The Chasm
- Copay Cards: Don’t Throw The Baby Out With The Bathwater
- Increasing Preferred Pharmacy Usage (3 of 3)
- Great Video! Placebo Effect Summarized In Video
- Walgreens and Express Scripts: The Plot Thickens ($ESRX, $WAG)
- Will The Stars Align To Drive Adherence?
- Will Pfizer Strategy On Lipitor Become The Norm?
Top 15 Posts From 2011
Based on individual visits, here are the top 15 posts from this past year:
Opportunists vs. Solidarity
With the Walgreens and Express Scripts dispute unresolved, you are certainly seeing more of an opportunistic attitude in pharmacies than one of solidarity. Maybe this shouldn’t be a surprise, but early on, I thought that the pharmacy groups would see Walgreens as their “leader” standing up to the large PBM. If the largest retailer can’t get negotiating leverage over the PBM, can anyone?
Now, if you go into my local grocery store (Dierbergs), you see signs about moving your prescriptions to them from Walgreens before it’s too late. You see and hear videos playing throughout the store talking about how to move your prescriptions and how easy it is.
CVS Caremark is predicting that it could see as many as 23M prescriptions move from Walgreens to CVS stores.
I’m certainly a fan of preferred or limited networks although I’m not sure I ever imagined a scenario where one PBM would totally exclude one of the big two retailers. I always imagined a scenario where you were playing them off each other and letting the client choose which one(s) to exclude.
You can see in the new whitepaper by Walgreens that they point out several things:
- The savings being offered / created is likely not enough for clients to want to exclude Walgreens and create the disruption.
- Clients who can include Walgreens are doing so and others would like to or believe they can.
- If Walgreens is excluded long-term, self-funded clients will be more likely to consider other PBMs.
- Many people still think this will get resolved in 2011 or by early 2012.
This brings up two other discussion topics:
- Will they come back? If the disruption happens (or has already happened), will consumers come back to Walgreens once they are back in the network? This will be a true test of satisfaction, branding, and many other efforts. On the flipside, the other retailers should be spending real effort welcoming and trying to retain the new consumers so they don’t boomerang back.
- Has the pressure shifted from Walgreens to Express Scripts? Depending on the timing, Walgreens will have felt most of their pain by mid-January. At that point, the pressure (IMHO) shifts to Express Scripts. Will they want to go through their 2012 selling season without Walgreens in their network, a major acquisition in the works, and any other potential distractions? I wouldn’t.
RWJF Guest Post: Interprofessional Collaborative Care Will Be Key to Meeting Tomorrow’s Health Care Needs
Guest Post by Maryjoan Ladden, Ph.D., R.N., F.A.A.N., Robert Wood Johnson Foundation Senior Program Officer
Maryjoan Ladden, PhD, RN, FAAN, is a senior program officer at the Robert Wood Johnson Foundation. A nurse practitioner whose work has focused on improving health care quality and safety through health professional collaboration, her work at the Foundation addresses: faculty recruitment and education to increase the capacity of nursing programs; developing collaborative partnerships to address local nursing issues; creating the next generation of academic nurse leaders; and building senior executive leaders in nursing. She also is senior editor for the Foundation’s quarterly publication, Charting Nursing’s Future. (full bio here)
A little over a year ago, the Institute of Medicine’s landmark Future of Nursing: Leading Change, Advancing Health report put forward a series of recommendations for transforming the nation’s health care system. Among them was a call for a system in which “interprofessional collaboration and coordination are the norm.” That’s no simple assignment in a system that often operates in silos, from schooling through practice. But a number of innovators around the nation are already making headway.
Their work is the subject of a new policy brief from the Robert Wood Johnson Foundation, part of its Charting Nursing’s Future (CNF) series. The brief delves into what the IOM recommendation means for health care systems, offers case studies of several collaborative care models already in place, and examines the implications of the recommendation for how we train nurses and other health care professionals.
According to the brief, Implementing the IOM Future of Nursing Report–Part II: The Potential of Interprofessional Collaborative Care to Improve Safety and Quality, the “silo” approach must soon give way if we are to meet coming health care challenges. For example, chronic conditions are increasingly common—not surprising given an aging population. But the health care system is poorly structured to provide the sort of coordinated care and preventive services needed to give these patients quality care while reducing costs.
Some health care institutions are gearing up for the challenge.
-
In Boston, where Harvard Vanguard Medical Associates developed its Complex Chronic Care (CCC) program, primary care has become interprofessional, collaborative and noticeably more efficient. Each CCC patient is assigned a nurse practitioner (NP), a registered nurse with advanced education and clinical training. The NP consults with all the patient’s subspecialists and incorporates their guidance in a single plan of care. The NP then manages and coordinates that care, connecting patients to nutritionists, social workers, and other professionals as needed. The model is dynamic, allowing patients to meet more or less frequently with the NPs and their primary care physicians, who remain responsible for the patients’ overall care.
-
In New Jersey, the Camden Coalition of Health Care Providers is “revolutionizing health care delivery for Camden’s costliest patients,” according to the brief. These individuals, sometimes called super utilizers, typically rely on hospital emergency rooms for care. Not surprisingly, such patients account for an outsized share of local hospital costs, often with diagnoses that would have been more properly handled in a primary care setting. The Coalition developed its Care Management Project to reduce these unnecessary emergency room visits by treating patients where they reside, even when that means treating them on the street. A social worker, NP and bilingual medical assistant work as a team to help patients apply for government assistance, find temporary shelter, enroll in medical day programs and coordinate their primary and specialty care.
Training the Next Generation to Collaborate
Of course, the silo effect usually begins in school. In May 2011, six national education associations representing various health care professions formed the Interprofessional Education Collaborative (IPEC) and released a set of core competencies to help professional schools in crafting curricula that will prepare future clinicians to provide more collaborative, team-based care.
Such efforts are already under way at a number of institutions.
-
Maine’s University of New England has developed a common undergraduate curriculum for its health professions programs in nursing, dental hygiene, athletic training, applied exercise and science, and health, wellness and occupational studies. The curriculum includes shared learning in basic science prerequisites and four new courses aimed specifically at teaching interprofessional competencies.
-
In Nashville, Vanderbilt University is also pursuing an interprofessional education initiative that unites students from the medical and nursing schools with graduate students pursuing degrees in pharmacy and social work at nearby institutions. Students are assigned to interprofessional working-learning teams at ambulatory care facilities in the area.
-
The Veterans Health Administration (VHA) is piloting an interprofessional initiative, as well, focused on preparing medical residents and nursing graduate students for collaborative practice. As part of the initiative, five VHA facilities have been designated Centers of Excellence and received five-year grants from the U.S. Department of Veterans Affairs. Each VHA Center of Excellence is developing its own approach to preparing health professionals for patient-centered, team-based primary care.
-
In Aurora, Colorado, the University of Colorado built its new Anschutz Medical Campus with the explicit objective of creating an environment that promotes collaboration among its medical, nursing, pharmacy, dentistry and public health students. It features shared auditoriums and simulation labs, as well as student lounges and other dedicated spaces in which students from different professions can pursue common interests such as geriatrics in a collaborative fashion.
Such initiatives are clearly the wave of the future, if only because the pressures of caring for a larger, older and sicker population of patients in the years to come will drive efforts to identify efficiencies. In the words of Mary Wakefield, PhD, RN, head of the Health Resources and Services Administration, “As the health care community is looking for new strategies and new ways of organizing to optimize our efforts—teamwork is fundamental to the conversation.”
Sign up to receive future Charting Nursing’s Future policy briefs by email at www.rwjf.org/goto/cnf.
Using Social Media For Underwriting
As healthcare moves towards an individual market where prior conditions can’t be excluded, will health plans be able to use social media data in underwriting? It seems logical. If I can understand your behaviors, I can asses your risk for life insurance, and I can predict some healthcare costs.
- Do you talk about going to the gym?
- Do you talk about drinking and smoking?
- Do you share pictures of food and is it healthy?
- Are you checking in at places like McDonalds or places like the park?
- Do you have an active social network?
- Are you going to the dentist and getting flu shots?
As companies like salesforce.com integrate social media through things like Radian6, can this type of tagging and data use be far behind?
The other question is whether is should get used?
Smoking is an easy target for lowering healthcare costs
These statistics from the CDC really paint the picture…
– Smoking is estimated to cost businesses over $170 billion a year.
– Every smoker on the payroll is costing the company more than $3,500 annually in increased health insurance premiums, increased absenteeism and lost productivity.
– Smokers take, on average, 6.5 more sick leave days a year than non-smokers.
– Smokers cost 35-50% more to insure, a figure which is increasing rapidly as healthcare costs spiral.
– On average, up to 40 minutes of the working day is spent on smoking breaks, which equates to 21 working days of lost productivity per smoker per year.
This is certainly why you see companies trying to avoid hiring smokers. For those that show pictures of them smoking on Facebook or in other social media channels, this might be a risk (although I’m not sure if it’s legal to use that).
What If The Medco Acquisition Doesn’t Happen?
First, I believe that the deal will happen without a doubt especially with the new specialty market share numbers from Adam Fein. While I understand the concerns of the independent pharmacies, I both disagree with them, and I don’t think that the FTC is focused on business protection but is looking at consumers.
That being said, the markets are still discounting the Medco stock which means they think there is some perceived risk. With the shareholder votes at both companies tomorrow, it got me thinking about what would happen if the deal didn’t happen.
If it didn’t happen, you’d have a much smaller Medco. They’ve lost United Healthcare, FEP, CALpers, BCBSNC, and I’m sure others. I’m sure you’d also have some change in the team with people’s resumes out in a tight healthcare executive labor market. You’d have a lot of clients wondering what they would do next. I’m also not sure if David would stay and his team has been together for a while so some of them would likely follow him. At the same time, I think Express Scripts would end up in good shape. They’ve paralyzed one of their big competitors for a year while they’ve continued several projects.
Medco would have to come out swinging in my mind. They would have to look at growth through acquisition putting several companies in play. They might also look at expanding beyond just the core PBM model which I think was always David’s perspective. Perhaps disease management or ACOs or exchanges or technology or maybe try to go vertical by looking at pharma or a wholesaler. I would think companies like IMS or inVentiv would also be interesting.
I’m not sure the FTC would disrupt the acquisition, but I did wonder if someone would try to be the spoiler like Express Scripts tried with the CVS acquisition of Caremark. I’m not sure who could do that but a United Healthcare could pull it off to support their services growth strategy with Optum. Or, Walgreens could take action to counteract their dispute with Express Scripts and follow the CVS Caremark success.
Interesting times.
[Note: I do own stock in many of the companies mentioned here.]
Live Longer By Being Optimistic!

While occasionally optimism can get you in trouble by being too trusting, I think it’s generally a better way to live. But, I still wonder why so many people can be overly optimistic about things like the lottery. Why do we all believe we can win when we’re more likely to get struck by lightning?
In healthcare, this means that we might overestimate our likelihood of getting better, not getting sick, or minimizing the risks of a surgery or medicine. “That will never happen to me.” According to an article about The Optimism Bias by Tali Sharot, people may get pessimistic about the broad economy but their private optimism stays very high.
For example, one study he mentions showed that cancer patients who were pessimistic were more likely to die within 8 months than optimistic patients. There was another article earlier this year about the impact of optimism on outcomes.
Another study talks about priming participants with key words such as smart and clever versus stupid and ignorant and comparing how they perform on a test. Guess what, the positive reinforcement led to better scores. (Why to pump your kids and co-workers up with positive self-esteem.) Perhaps, most importantly, the brains that expected to do poorly didn’t trigger responses to learn from their mistakes while the other participants did.
A few data points from the article:
- 10% of Americans expect to live to be 100…while only 0.02% do
- 0% of people getting married expect to divorce…but we know the numbers here
- 93% of people believed they were in the top 50th percentile for their driving ability
- www.bestautolenders.com
Why You Need Some Anxiety In Your Life
While 18% of the US adults have some type of anxiety disorder – generalized anxiety, OCD, phobias, panic disorder, social anxiety, or PSTD, Time magazine recently had an article on whether anxiety could be good for the rest of us. (12/5/11)
As most of us know, anxiety causes stress which constricts our blood vessels and causes our blood pressure to rise. But, it can also impact our metabolism and the way we burn calories. And, it can also impact digestion which can lead to heartburn, bloating, and diarrhea. (It doesn’t sound so good so far.)
But, the article goes on to point out that the hormones that drive anxiety can be powerful stimulants helping our senses to work at their best. It’s the difference between a “challenge stress” and a “threat stress”. Finding that right point on the curve where anxiety increases performance is critical. The article talks about a “metabolic jujitsu” of turning anxiety back on itself. That’s an interesting way of thinking about harnessing stress to better perform. I certainly need some stress in my life to feel the need to push harder in what I’m working on.

(Graphic from http://spinalstenosis.org/blog/back-pain-stress/)
Using the Local Pharmacist to Moderate the P2P Discussion

P2P or Peer-to-Peer healthcare is a common discussion topic these days. Patients want to go online and learn from others with their condition on sites like Inspire.com or PatientsLikeMe.com. The government has been one of the early adopters.
“The social media sites we have created show that the government can interact in a meaningful way with the public. We don’t just push information out; we strive to make the content relevant so people can act on it, share it with family or friends and ultimately change their behavior.” Amy Burnett, CDC (Tapping Into The Power By Getting Personal, Robin Robinson, PharmaVOICE, May 2011)
The question is how can traditional companies – pharmaceutical manufacturers, disease management companies, providers, managed care companies, pharmacies, and PBMs – interact in these discussions. On the one hand, they have a broad depth of experience and data to share. On the other hand, they can’t just jump in and drive their agenda. They have to add value to the conversation, demonstrate that they care, and add value.
Much like the idea that you can purchase things online and return them to the physical store, I think these virtual discussions need to eventually be tied to a physical experience for many patients. One group that I think could play significantly in this is local pharmacists. Imagine that a chain or an association created a social media team. That team could monitor and interact with patients especially in key conditions such as some of the specialty drug areas. As relevant, this could be linked back to a local store where a pharmacist could spend time consulting with the patient. I think this would be a great way to drive the retail specialty business and increase consumer brand awareness.
“The potential use of social media as a bellwether for identifying trends, informational gaps, support tools, even improved communications between providers, allied health professionals, and others could pave the way for a more collaborative approach to population mapping and patient care.” Michael Parks, Vox Media (Social Media: Paving The Way, Robin Robinson, PharmaVOICE, May 2011)
The CDC has even created a toolkit for people to use.
A Computer For The Baby?
I found an article in USA Today about computers for toddlers very interesting. (Image is The Vinci from this article.)
While I think anyone with kids has noticed their affinity to towards the Apple products (iTouch, iPhone, iPad), this article questions the wisdom of getting babies computers to play with. There are a few key questions here:
- Is it necessary?
- Does it accelerate their learning?
- Will it negatively impact them?
According to the article, 10% of kids below 1 and 39% of kids age 2-4 have used a mobile device. I guess the question I would have is whether this is simply for watching a video or for some actual educational purpose. The article quotes an expert saying that there is no evidence that educational toys are building brainier babies and the companies are simply preying on us parents that want to give our kids a headstart. Is it true?
I think technology has a role in our kid’s lives, but you have to think about it like TV and other things. Use it in moderation. Kids still need to learn by experiencing things. Kids still need to build with Legos. They need to get out and play. They need to read books. They need to draw and create things.
This is just a good reminder about the Kaiser study on the amount of screen time our kids have today.
The article also reminds you that the American Academy of Pediatrics recommends no screen time for kids under 2 and no more than 2 hours a day after that.
Will Doctor As Friend Impact Outcomes?
I was at my daughter’s DARE graduation today. [I didn’t realize there was such a thing until recently.] One of the comments that the officer made to the parents was to be a parent not a friend to your kids. I agree that this is important, but of course, my mind immediately drifted to how does that apply to healthcare.
As we think about measuring physician or provider satisfaction, does this factor in? If the provider attempts to become a “friend” with the patient, will that improve outcomes or will that detract from their ability to be the “authority”? It’s an interesting question for which I don’t know the answer.
On the one hand, I would imagine that a patient is more likely to ask questions and engage in a health dialogue with a “friend” but are they more likely to take action?
My impression is that this is where there is a blended approach needed where the provider has to be an authority and provide the patient with strict recommendations (e.g., you’re fat and going to die if you don’t do something different), but they have to be approachable so that the patient is comfortable. [If you’ve ever watched The Biggest Loser, you can see that their physician seems to play this role by being engaged with the patients over time.]
But, this could impact physician reviews which simply makes it more important to take those with a grain of salt. Just like schools or companies, one that works for someone may not work for someone else. We are all individuals and different.
Infographic: The Billing Impact On Satisfaction and Health
I can definitely understand this. I remember using a physician who I knew for services. The billing experience was so bad that I wouldn’t go back to his office and wouldn’t recommend him to someone else.
Obviously, if people lose connections with their provider that will impact their health.
Barrett Toan To Speak At PBMI Spring Conference
Barrett Toan who was the motivating force behind building Express Scripts has been gone for since 2006 when he stepped down as Chairman of the board. He is now the chairman of Sigma Aldrich here in St. Louis and active in other pursuits. I was excited yesterday when I heard from Brenda Motheral, the Executive Director at PBMI, that Barrett had agreed to speak at their conference (register here).
While I never got to work with Barrett as closely as I would have liked to, I was on several projects with him. I was always amazed by both his passion for the industry and the patient along with his ability to move from both the macro-vision to digging down into the details. It should be fascinating to hear his view on where the industry is today and all the changes that have happened.
And, that should add to the agenda they already have which includes Gilbert Welch, the author of Overdiagnosed, Kjel Johnson from Magellan, Stacy Dow from Whirlpool, and Dr. Troy Brennan from CVS Caremark.
The focus of the agenda this year is on specialty which is obviously front and center for all of us. The one concern that I have had in the past was around attendee mix. It always seemed like the PBMs talking to each other, but Brenda told me that so far ~75% of the registrants are plan sponsors and that the actual number of plan sponsors registered already exceeds last year. This would be a big and very positive change.
Brenda also mentioned several other key topics – 340B, MTM, eRx, generics, consumerism, OTC, and Rx and Dx integration. Of course, I’m sure there will be discussion from their survey which I reviewed earlier, and they will be releasing their new specialty survey at the event. I’m planning to attend, and I hope to see you there.
Cost and Outcomes Drive Better Use of Data
Overall, I would describe healthcare companies as trying to figure out how to drive the best outcomes at the lowest cost while maintaining a positive consumer experience. This isn’t easy. One area of opportunity that companies increasingly look at is how to use data to become smarter.
- Can I build a predictive model of response curves? Who’s likely to respond? Who’s likely to take action?
- Can I develop a segmentation model that works? How will I customize my communications after the segmentation?
- Can I rank and prioritize my outreaches? Should I do that based on risk or based on potential value?
Ultimately, I think this is driving companies to be a lot smarter and to look at how they use both medical and pharmacy data. For example, I’ll point to both CVS Caremark and Prime Therapeutics in press releases from earlier this year.
“The ActiveHealth CareEngine offers evidence-based information that can be used to improve the health care of our members and enables us to take our programs to the next level by seamlessly incorporating medical data,” stated Troyen Brennan, EVP and chief medical officer of CVS Caremark. “This agreement will enhance our existing programs to identify issues related to gaps in care, potential drug-to-drug interactions and duplicative care — information that is important to bring to the attention of the member’s physician.” (article that this is sourced from)
Smart use of medical and pharmacy data is one of the most powerful tools we have to improve outcomes and increase value for our members and clients,” said David Lassen, PharmD, Chief Clinical Officer at Prime. “Through ongoing partnership with health plan clients, Prime is uniquely positioned to view the entire spectrum of patient care, and we can leverage that information to help manage cost and to improve outcomes. We are very excited to collaborate with Corticon on the development of this clinical platform.” (press release)
The next step will be to integrate PRO (patient reported outcomes) from sources like connected devices and PHR (personal health records) that might show blood pressure, workouts, calories, or other data points that could help companies determine when to intervene and how to add value to drive an outcome.
Additionally, another key is continued work in the outcomes-based contracting world and bonus areas such as Star Ratings where the financial value is tied in the short-term to outcomes. This creates a burning platform for smarter use of data and use of a broader set of data to understand and impact care.
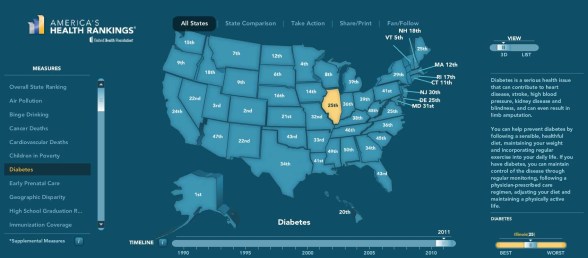
State By State Rankings – Key Healthcare Metrics
United Health Foundation published their Health Rankings today which offers some great statistics and interactive graphics to see how states compare on things like high cholesterol and diabetes. I pulled a few examples here, but it’s definitely worth checking out.
Medicare Patients Save $1.5B on Rxs!!
Now, here’s a great story. This may be one of the best government success that I’ve heard about in what I think of as a collaboration of the government with multiple businesses. (Although I think this is a lot more of what HHS is doing these days under Todd Park’s guidance.)
According to USA Today this morning, more than 2.65M Medicare recipients have saved an average of $569 per person this year based on addressing the donut hole with a 50% discount on the brand drugs filled during this time. And, the average premium for 2012 is actually LOWER than the premium in 2011 (by $0.76 per month).
The other part of the article is about the potential value of preventative care and leveraging this as part of the Medicare benefit. The key here is engagement of the participants to help them understand and take action on their healthcare. The power of the consumer in driving healthcare costs and outcomes is significant which is a topic that I know was discussed by several people today at the mHealth event in DC.
What’s Your Digital Strategy?
Do you have a digital strategy? Even if you don’t call it out that way, you certainly have digital as part of your overall member and physician strategy these days.
Hopefully, you start with a few basics like:
- What do I want to accomplish?
- How do I measure success?
- Who am I targeting?
- What does my target group do online and what tools do they use (and for what)?
- What is my competition doing? (and what do companies outside my vertical that I want to emulate do)
Once you know those things, you can start looking at different areas of focus. The key ones that jump to mind for me are:
- Search engine optimization
- Brand monitoring (e.g., Radian6)
- Content creation (blogging, Twitter, Facebook, Google+, LinkedIn)
- Moderation and involvement with social networking (e.g., PatientsLikeMe, DiabetesMine)
- Tele-monitoring / telemedicine
- Electronic prescribing / EMR / PHR
- Digital couponing / incentives
- Gamification
- Mobile applications
- SMS
- QR codes
- Augmented reality
But, I’m sure there are others…suggestions on what I’m missing?
Is “Gluten Free” A Diet?

We’ve all seen it over the past few years. More and more foods have the label “gluten free” on them. For the 1% of the population with celiac disease and others with some gluten sensitivity, this is great. But, since only 8-12% of the purchases of these products are made by people with gluten intolerance, what’s the reason for the purchase?
46% of people bought them because they thought they were healthier and 30% bought them to help them manage their weight. And, with this being a $2.6B market, everyone is jumping on the bandwagon.
The key question is whether this lives up to expectations. It seems the short answer is no.
“If you avoid only gluten, you will likely be getting more calories with few nutrients.” Dr. Stefano Guandalini, founder and director of the Celiac Disease Center (Time Magazine article)
You can see more about the FDA’s proposed labeling on gluten free here.

 December 23, 2011
December 23, 2011 




![Hospital Billing Survey [Infographic]](https://i0.wp.com/connance.com/sites/default/files/images/hospital-billing-survey.png)