This is one of those terms that is thrown around a lot just like Medical Management or Disease Management.
I thought it would be helpful to define the 3.
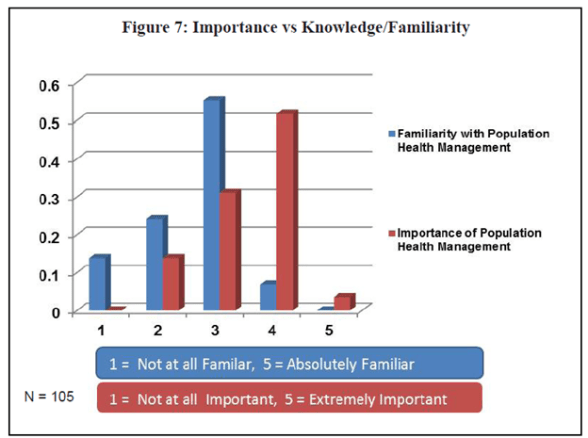
Population Health Management (PHM) is…
“Programs targeted to a defined population that use a variety of individual, organizational, and societal interventions to improve health outcomes” (Mathematica Policy Research Issue Brief, August 2011)
Medical Management (MM) is…
“The general term often applied to the practices of utilization management (UM), case management (CM), and disease management (DM), alone or in combination with each other.” (Trends and Practices in Medical Management: 2001 Industry Profile)
Disease Management (DM) is…
“An approach to healthcare that teaches patients how to manage a chronic disease.” (Disease Management on About.com)
Is that clear as mud?
In today’s world, everything is patient-centric so that doesn’t differ between the three. Obviously, DM is a part of MM, but I rarely hear people talk about MM as a part of PHM which it seems to be to me. But, I don’t think of most MM type programs taking on the macro level change that PHM implies to me. PHM implies things like public health or broad programs like BlueZones. It implies looking at things like plan design, incentives, social trends, workplace culture, and other aspects of change that are necessary to create change and sustain change.
Here’s the Care Continuum Alliance’s full description of PHM (or as they call it here – population health improvement):
Key components of the population health improvement model include:
- Population identification strategies and processes;
- Comprehensive needs assessments that assess physical, psychological, economic, and environmental needs;
- Proactive health promotion programs that increase awareness of the health risks associated with certain personal behaviors and lifestyles;
- Patient-centric health management goals and education which may include primary prevention, behavior modification programs, and support for concordance between the patient and the primary care provider;
- Self-management interventions aimed at influencing the targeted population to make behavioral changes;
- Routine reporting and feedback loops which may include communications with patient, physicians, health plan and ancillary providers;
- Evaluation of clinical, humanistic, and economic outcomes on an ongoing basis with the goal of improving overall population health.
The population health improvement model:
- Encourages patients to have a provider relationship where they receive ongoing primary care in addition to specialty care;
- Complements the physician/practitioner and patient relationship and plan of care across all stages, including wellness, prevention, chronic, acute and end-of-life care;
- Assists unpaid caregivers, such as family and friends, by providing relevant information and care coordination;
- Offers physicians additional resources to address gaps in patient health care literacy, knowledge of the health care system, and timeliness of treatment;
- Assists physicians in collecting, coordinating and analyzing patient specific information and data from multiple members of the health care team including the patients themselves;
- Assists physicians in analyzing data across entire patient populations;
- Addresses cultural sensitivities and preferences of individuals from disparate backgrounds;
- Promotes complementary care settings and techniques such as group visits, remote patient monitoring, telemedicine, telehealth, and behavior modification and motivation techniques for appropriate patient populations.
And, if you read articles about PHM, these macro issues don’t seem to be the focus. The focus seems to be mostly on the technology to accomplish PHM. There are obvious challenges and key success factors there. (Recent commentary on PHM.)

 October 29, 2012
October 29, 2012