This is a little bit of a rant set off by the current market / political situation. First, I know we all think of this as a bailout…apparently the messaging is 20:1 in DC from their constituents. I wonder how many of those people are the same people that wanted loose credit standards so that more people could afford houses and people could get bigger houses.
Blaming the banks is like blaming the auto companies for making SUVs. They are giving the consumers what they want. If consumers are willing to buy it, someone is going to make it.
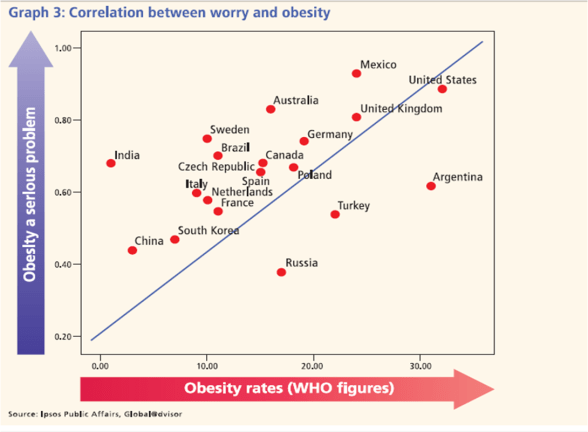
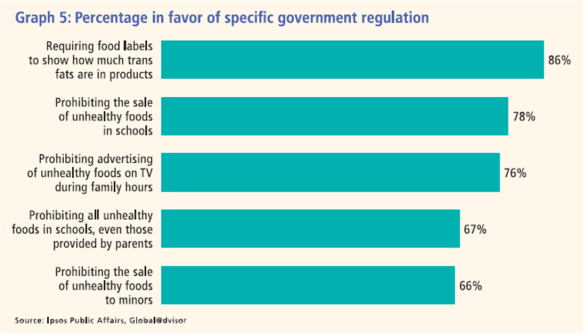
But, this has lots of application in healthcare. We are critical of the fast food companies for contributing to our obesity epidemic, but we don’t want government regulation and we don’t self-regulate. We want to stay compliant with our medications, but we forget and don’t want to be told what to do. We want to have unlimited access to care, but we don’t take preventative steps…we wait until it’s an emergency. We don’t want prices to go up, but we want to have every possible test done using the latest technology.
So…why do we shift blame around? We need to understand the long-term implications of our decisions from wanting the bigger house to driving the SUV to eating whatever we want.

 September 30, 2008
September 30, 2008