I always enjoyed being part of the team that put the Drug Trend Report out when I was at Express Scripts from 2001-2006. With that in mind, I do await anxiously to see what new information they will share each year. I will say that the core fundamentals (as always) were very strong in the 2009 report, but I missed not having any client case studies in the document.
They reported drug trend of 1.5% (without specialty) and 3% with specialty.
Specialty drug trend was 15.4%.
Patients paid an average of $12.82 per Rx.
They say that more patients converted to Home Delivery (aka mail order). [I have to check this. My recollection is that mail volume was relatively flat and this would be hard to achieve unless they had more people filling less drugs on average at mail.]
They reported PMPY utilization of 14.32 Rxs.
Their members paid 29% of the generic drug costs; 19.6% of the brand costs; and 22.3% overall for traditional drugs. For specialty drugs, they paid 2.3% (or 20.2% for all drugs including specialty).
They have a section on compliance (which is rapidly becoming a key discussion point in the PBM world). I was a little surprised they didn’t call it adherence which is more common these days. But, they revealed some surprisingly high MPR (medication possession ratio) numbers for antidiabetics, antihypertensives, and lipid-lowering drugs. Considering adherence is where a member has an MPR of greater than 80%, they showed 77%, 83%, and 83% respectively. Since we know that 50% of people (on average) drop therapy within 12-months, this seems improbable on a book-of-business basis. (Maybe I’m just becoming a cynic in my old age.) The only reason I could find to explain this example was that this was not based on new starts (i.e., NRxs) unless they came in the first quarter. Therefore, there might be some selection bias in that they are taking MPR on people that started the year on the medication and may therefore have been people who were more likely to be adherent. I would rather see this done on a rolling 12-month basis.
As I often use, they define waste in the system and give you a potential GFR (generic fill rate) goal for the top therapy classes.
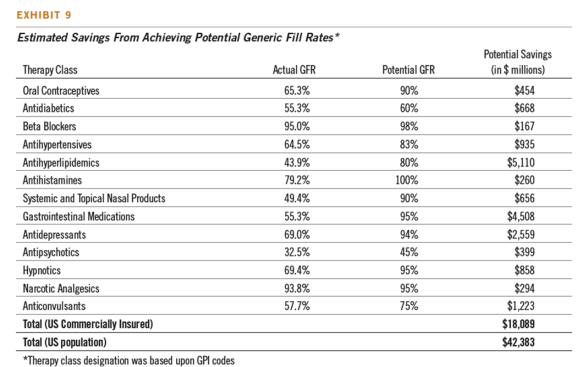
Their analysis shows that 55% of the costs for specialty drugs were billed through the medical benefit rather than the pharmacy benefit.
55% of their members are in plans with at least one step therapy module.
They talk about a few studies they have published showing that targeted and framed messages are more effective than general messages. And, that those messages are more effective with mail order users than people at retail.
Again, there might be some selection bias here as people at Home Delivery may simply be more active in managing their healthcare. The other question I have had for a few of my friends there has been whether we are comparing apples-to-apples. Since I ran a few of the programs before I left, I know we did a lot more interventions (web, inbound IVR, outbound calls, messaging on the invoice, letters, POS rejects) than we did for retail (letters and outbound IVR). If they’ve adjusted for that, than this is clear. If not, I would want to see that adjustment made.
As anyone who reads the blog knows, I am a big supporter of the theory behind their Consumerology story. I think Larry Zarin and Bob Nease have done a great job putting together their advisory board, creating case studies, and using behavioral economics. I always talk with our clients about these theories, and our analytics team is constantly helping clients define test plans that use these.
- Social comparison
- Hyperbolic discounting
- Loss aversion
In comparing adherence at retail and mail, one thing that came into my mind was whether a driver of better adherence was a longer time window to refill. Typically, you have a refill-too-soon (RTS) edit in place until 2/3rds of the medication has been used (based on days supply dispensed from dispense date). At retail, that means you have about 10 days. At mail, that means you have about 30 days (less the 7 days for shipping). Does that make a difference?
I was also surprised under the methodology section that they now include rebates in calculating costs. It’s a quick one-line comment but how did that effect trend or other metrics here…and if so, how significantly?
As always, I love the therapy class reviews in the back that give you great numbers like:
- Cost PMPY
- # Rxs PMPY
- Prevalence of Use
- Average Cost / Rx
- # Rxs / User / Year


 May 25, 2009
May 25, 2009