As someone who was trained as an architect, I understand the value of sketches in the design process and have always “doodled” as I try to conceptualize what people are describing with words. With that in mind, I really enjoyed this TED video and think it’s a good message for all of us in the communications field.
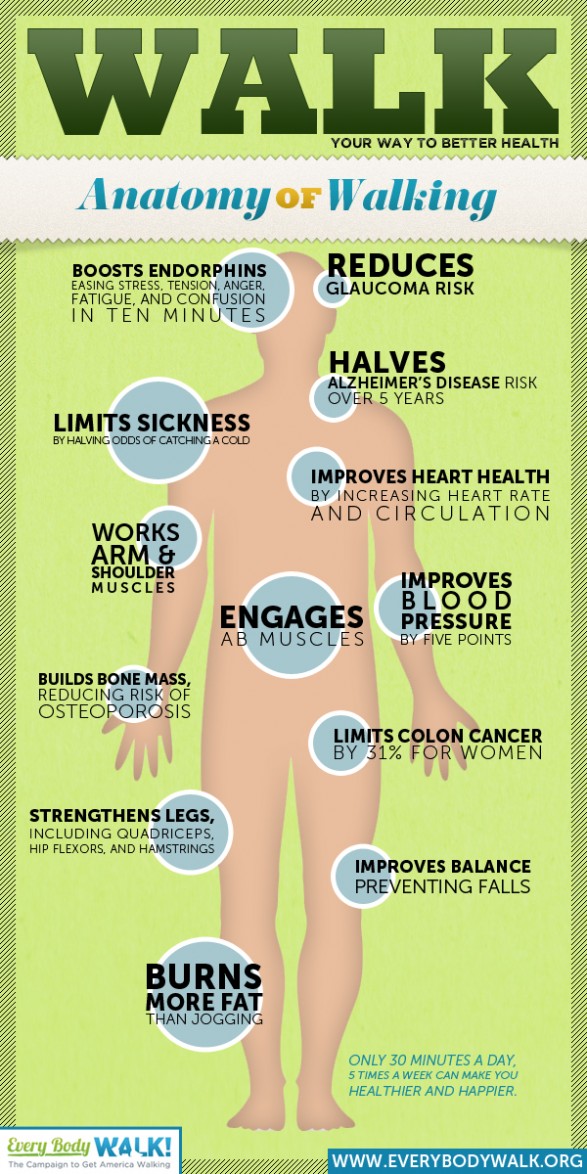
EveryBodyWalk.org Infographic
Some of you have probably seen some of the efforts by Kaiser to encourage walking. Here’s an infographic that they put out as part of their EverybodyWalk efforts.
Ambient Paper For Adherence
We’ve all heard of GlowCaps which is a great idea of using sound and color and communications to remind people to fill their medications.
One idea I’ve thought about for several years is the idea of “intelligent paper”. Imagine a refrigerator magnet or prescription label or some other piece of information printed on paper that changed color with time. As it got closer to time to refill your medication, it would turn yellow. When it was time to refill, it would turn red.
It should be easy. If you blend this with the QR code that Walgreens uses for refills, you have a captive reminder and reorder system that could be embedded within the label for less cost. I haven’t totally solved the issue, but it’s one that I think is feasible to accomplish and sell as a low-cost reminder vehicle.
Coordinated Versus Integrated PBM
I’ve long held what would appear to be conflicting positions:
A. I believe that a standalone PBM offers the unique ability to be laser focused on pharmacy and should therefore optimize your benefits from a carve-out perspective.
B. I also believe that ideally that focus could be achieved within an integrated benefit where you could leverage pharmacy strategically to drive down the bigger overall area of costs – medical.
So, my initial reaction when I heard about the study below Anthem was that this finally showed a clear savings from the integrated PBM model.
According to a separate analysis Anthem conducted of members in its affiliated health plans, enrollees with both medical and pharmacy benefits managed by Anthem have medical costs that are $8 to $16 lower per employee per month compared with those without Anthem’s pharmacy program. (from Drug Benefit News)
I haven’t seen the original study which I’d like to read in more depth, but on the surface, this is interesting. After further retrospect, I wonder if the issue isn’t necessarily integrated versus coordinated.
Can a standalone PBM act as an integrated PBM? What would need to happen for that to be true?
- They would need to coordinate benefit design across both areas (pharmacy and medical) which is easier when the managed care company is the buyer of PBM services not the individual employers.
- There would need to be integration of pharmacy and medical benefits into a predictive model and an outcomes model.
- The PBM would need to be tied to outcomes in some type of P4P model.
Pharmacy Adherence (Waste) And The Need for MD-RPh Collaboration
I spent the day today at the NEHI adherence event in DC. I pulled out a few of my takeaways below, but while I was riding on the plane to get here, a few things were running thru my head:
- The focus on budget and the estimates that adherence costs us $290B a year here in the US. (or as one person pointed out that’s $1.2T in a presidential term)
- The recent report estimating that chronic conditions could cost us $47T worldwide over the 20 years which is leading to the UN talking about healthcare for only the second time ever.
- The discussion by George Paz from Express Scripts the other day about how PBMs drive value by eliminating waste (see Drug Trend Report). A large piece of waste is adherence and certainly one of the forecasted benefits of the combined Express Scipts and Medco entity is the intersection of Consumerology with the Therapeutic Resource Centers (TRCs).
- The ongoing dialogue around motivational interviewing, commercial MTM, and blending face to face interventions with technology to “nudge” behaviors.
- The huge opportunity which I believe exists in leveraging technologies like Surescripts to create data exchanges with physicians around MPR and barriers.
- The exciting fact that the new STAR measures for Medicare include more adherence metrics that are weighed more heavily than some of the operational metrics.
Fortunately, these were a lot of the topics that were discussed. Here some of the discussion topics:
- The fact that there’s no “easy button” for adherence.
- How adherence is a foundational building block for quality.
- The role of HIT in sharing data bi-directionally across the care team.
- Upcoming evidence around VBID.
- The role of the pharmacist and need for them to collaborate more with the physician to discuss and manage adherence.
- The fact that the adherence solution has to be multi-factorial.
- The need to optimize the drug regiment and individualize care (aka patient-centered care).
- The role of the caregiver.
- Opportunities around PCMH, readmissions, MTM, and eRx.
- The need for patient engagement.
- The need for the patient to believe in the therapy and that it will make them better.
- Good discussion on the role of the PCMH (patient-centered medical home) versus the pharmacy as the foundation for adherence.
- Discussion on whether physicians could address adherence if time wasn’t an issue. Do they have the training and skills?
- Social media as an emerging factor.
- Reaching the consumer when they have time and are receptive to information.
- Helping prepare the consumer for the encounter (i.e., checklist or list of questions).
- What happens when the patient waits in line and then is rushed themselves in the encounter.
- The role of technology in complementing the physician and patient.
- How to share data across team members.
- The need for ROI data on interventions.
- The value of having a Dx on the Rx.
- The need to vary incentives and not keep doing the same thing.
- If prevention is long-term and adherence is short-term, should the physician focus more on adherence and less on screening and other preventative measures.
- The need for – sufficient accountability, information, and skills.
- Adherence as a solution that needs to be localized.
- Patient centered or disease centered solutions.
- The governments role in improving adherence via policy and funding demonstration projects through CMS.
- STAR ratings and the bonus payments as an incentive to motivate research and programs in this area.
Overall, it was a good discussion with a very engaged panel and audience. We didn’t come to any answers, but you certainly got to think about the topic, identify some projects that should be done, and identify some research questions.
I look forward to pulling out a few of the topics in more depth. They align well with the communications platform and intervention strategies that Silverlink provides for our clients around adherence.
Flu Shots: Stock It And They Will Come?
This is the hot topic. Everyone wants you to get a flu shot because it’s good for your health and a profit making opportunity.
- The CDC recommends flu shots for everyone over 6 months of age.
- Pharmacies have big expectations about volume but “unfortunately” (from the perspective of nudging people to act) the disease does not seem to be too prevalent yet.
According to the CDC (and thanks to Larry Marsh’s team at Barclays Capital for sending out in their Flu Clues report):
We highlight that 0.8% of patient visits to physicians were due to flu-like illness, which is down 20bps from last week’s data. We note that this is well below the peak of 8.0% in early 2010. The 0.8% rate is below the national baseline average of 2.5%. Next we note that 6.0% of all reported deaths were due to pneumonia and the flu, 10 bps below last week, and below the epidemic threshold of 6.4% for week 37.
Traditionally, only about 40% of US adults will get a flu shot meaning there’s lots of opportunity for growth in vaccinations. Tim Martin from the WSJ has talked about this in a few recent articles – Flu Shots Are A tough Sell This Year and People Have Big Plans For Flu Shots. In the second article, he quotes a recent survey showing almost 2/3rds of adults plan to get the shot this year. BUT WHY? (other than the fact that those who respond to survey’s around flu shots may be more likely to take action)
You can also look at the Google flu trends data (again thanks to Larry Marsh and team for pointing this out) which shows online searches down for flu topics:
Like last year, the number of locations for getting a flu shot has expanded exponentially driven predominantly by pharmacies (which BTW is a good thing for them in demonstrating additional value). You’re even seeing some creative programs building on last year’s programs. One new one I’ve seen is Walgreens use of Foursquare for donating flu shots.
Of course, if we can’t convince healthcare workers to get flu shots then it’s going to be really hard to convince the average consumer.
I would expect MA plans to work with their PDP provider or pharmacy partner to drive members to get flu shots. Since flu shots are a STAR measure, it’s important for plans to reach out and get consumers to get a flu shot.
But why should I get a flu shot if my likelihood of getting the flu is down? That is the question.
That’s why I’m skeptical about some of the “generic” marketing efforts. I think everyone knows that they “should” get a flu shot and now finding a location for one is easy. BUT, we need to make it relevant to them especially those of us in healthcare. Ideally, their pharmacist and physician are talking to them about it, but if not, how do “we” (as healthcare companies) engage them.
We have to make the “pitch” relevant to them. For families, make them understand the importance of keeping the family healthy and their kids in school. For pregnant moms, help them understand that it’s important and why. For people who work, stress the importance of not missing work. For people with chronic conditions, focus on their additional risk. For the elderly, explain the risks to them.
A recent Walgreens study quantified some of the costs of the flu:
A new Walgreens survey examining the effects of influenza on people’s everyday lives and the economy, suggests that last flu season resulted in 100 million lost works days, along with nearly $7 billion in lost wages and 32 million missed school days, among many other findings released today. These findings, the first of a two-part Walgreens Flu Impact Report series, underscore the ramifications the flu and ill-timed illness can have beyond people’s health – from missed work and lost income to parenting challenges.
According to the Centers for Disease Control and Prevention (CDC), on average 13 percent of the U.S. population gets the flu every year, with active flu seasons seeing closer to 20 percent, or more than 62 million Americans.
Judicial Committee On Proposed Express Scripts Acquisition Of Medco
While the judicial committee meeting today has no direct bearing on the FTC’s review of the proposed merger, it will definitely help form some public opinions and may help layout some areas of focus for the review. You can see the Bloomberg summary of some of the key quotes here.
You can also read the submitted testimony by each of the six witnesses online at the judicial site. I pulled a few comments from each below.
From Stephanie Kanwit:
The most important theme of the Guidelines is that “mergers should not be permitted to create, enhance, or entrench market power or to facilitate its exercise.” Reams have been written about what constitutes “market power,” but the definition in the Guidelines is relatively straightforward:
“A merger enhances market power if it is likely to encourage one or more firms to raise prices, reduce output, diminish innovation, or otherwise harm customers as a result of diminished competitive constraints or incentives.”
From Dan Gustafson:
the major PBMs continue to expand exclusive distribution arrangements with pharmaceutical manufacturers. Further analysis is required to determine whether these acquisitions and distribution alliances have led to decreased service and consumer choice in providers, as well as substantial increases in the prices of several specialty drugs. [Isn’t this becoming the norm with more and more REMS being required by the government for specialty drugs?]
From Dennis Wiesner:
The payment from a PBM to a pharmacy for dispensing a prescription drug differs from the amount a PBM charges a plan for the same prescription drug, to the benefit of the PBM. Plans sponsors are typically unaware of this difference, commonly referred to as “spread.” [Isn’t this common in business? Does a clothing retailer reveal what it pays its supplier for goods?]
From Joseph Lech:
Everyone knows the fastest way to reduce drug costs is to maximize the proper utilization less-expensive generic drugs. Yet, community pharmacies dispense generics at a much higher rate than the PBM-owned mail order outlets because we do not have incentives, such as kickbacks from manufacturers, to dispense brand name drugs. For example, the generic dispensing rate at the ESI mail facility is 60%. It is 62% at the Medco facility. By contrast, community pharmacies dispense generics on average 72% of the time. [How long will these inflated statistics stay around…it’s like the false perception about vaccines. You have to adjust out the acute drugs and acknowledge a different consumer mix leading to similar GFR.]
From George Paz:
According to our data, Express Scripts members utilizing our full complement of tools enjoy an additional annual average savings of over 11 percent per year. These savings are in addition to the discounts from negotiating with drug makers, which average 27 percent below the average cash price consumers would pay at a retail pharmacy for brand name drugs and 53 percent below the retail cash price for generic drugs.
From David Snow:
The business of pharmacy benefit managers (PBMs) is defined by robust competition, with more than 40 PBMs working hard to provide differentiated value propositions for public and private payors. These firms are a diverse group with very different business models and varying degrees of vertical integration, some integrated with pharmacies, others integrated with managed care organizations and others entirely independent. Nine Fortune 500 companies operate their own PBMs. Non-PBM participants like Wal-Mart and Target also contribute meaningfully to the competitive landscape by offering low-price generic prescriptions, as do other retail pharmacies that are providing steep discounts on 90-day prescriptions.
I didn’t get to listen to the prepared testimony, but I think I heard most of the Q&A which was interesting. But, I think I’m too close to it. I was really confused by some of questions and discussion.
- If the large payers only will choose one of the large PBMs that aren’t associated with another payer (i.e., OptumRx or Humana Rightsource), why would a merger of two of the top three affect the smaller PBMs in any way? [I don’t agree with the hypothesis by the way.]
- Since several PBMs leverage either SXC or Argus software, why would someone say that the smaller PBMs don’t have access to the same technology?
- Why would you view sales to managed care companies as a submarket for which to look specifically at marketshare? Or national employers for that matter? And, will any of that matter in the exchange market if consumers can purchase pharmacy coverage separately from medical benefits?
- Since consumers typically pay copayments, why is there a big focus on how consumers feel the savings of the merger? They may see a slight difference in percentage copayment plan designs, but the savings accrue to the payer which can choose whether or not to share those savings through lower copayments with the consumer.
- What services that a PBM provides are limited because of their geographic location? This seems to be one of the key points about the limitations of the smaller PBMs.
- Part of the pharmacy arguement was for creating a pharmacy home (which I agree with) and directing consumers to a single pharmacy. They also talked about having the pharmacist determine who should be allowed to fill 90-day prescriptions. This doesn’t sound very consumer friendly and sounds a lot like what they say the PBMs are doing that is bad.
- The idea that drugs are just shipped to patients without them wanting them was brought up several times. I’d really love to see some specific data about how that happens. Did their physician call it in? Did they sign up for auto-refill? There is a process to be followed which addresses consent and payment so while I believe consumers may say this happened I’d love to see the data on an individual basis.
I also thought it showed the difference culturally or philosophically when you listened to George Paz answer the question about the greatest opportunity to save money versus David Snow’s reponse.
- George said to focus on eliminating fraud, waste, and abuse
- David said to focus on managing chronic conditions
This difference is both the challenge and the opportunity that the combined entity will have to embrace.
The one part that really frustrated me was watching the member of the committee from Michigan try to pin everyone down on what they thought of healthcare reform and making the point that they were under oath. That seemed too political and not relevant to me.
Post ESRX/MHS Merger – How Many Big PBMs Are There?
This seems to be one of the critical questions in the evaluation of whether the merger should go through. We’ve always talked about the Big 3 PBMs – Express Scripts, Medco, and CVS Caremark. If that’s the market, then going from 3 to 2 seems like a huge deal.
But, I think the market has and is changing.
- What about OptumRx (formerly Prescription Solutions)? Once the lives formerly managed by Medco are insourced in 2013, this is going to be > $20B company (I believe) which is part of a huge company (United Healthcare).
- What about Prime Therapeutics? They manage over 14M members (I believe) and have been actively bringing in lots of new management from other PBMs as part of their growth strategy.
- What about SXC and CatalystRx? They both have shown their ability to win against the “Big 3” and grow.
- What about “captive PBMs” like Humana and CIGNA? I think they would both want a bigger crack at the lives outside their insured book of business.
- What about MedImpact? They manage 35M lives today.
Today’s session in DC will certainly be interesting.
[As noted before, I both own shares in some of the companies mentioned here and do business with others and/or seek to do business with the companies mentioned here.]
New Walgreens Pharmacy Layout

I was in a Walgreens last week in Chicago. Maybe it’s just a newer store than my local store in St. Louis, but I thought the pharmacy looked very different. I captured a few shots with my camera phone. As you can see below:
1. There is an automated check-in option for refills. 
2. There is a pharmacist in front of the counter not just behind. (And people were actively coming in and talking with him.) The clinic also seemed to have a person on the floor roaving around interacting rather than sitting behind a podium. 
4. There was a sitting space with what appeared to be a meeting room.
5. Overall, there was a lot more signage and videos which made it a very lively and bright place to be. 
This seems like a different engagement strategy. I’m surprised no one is talking about it. The only thing I could find was a mention of a “training store” and 40 locations and the following mention in an article about Express Scripts and Walgreens:
As part of its plan to expand its healthcare offerings and reduce costs, Walgreen is working on pilot stores with new technology and a health guide on staff to help patrons more easily fill prescriptions, speak to pharmacists and see nurse practitioners at its in-store Take Care clinics. The first such store, in the village of Oak Park, Illinois, opened in November. Walgreen plans to have 20 stores in Chicago and other nearby towns by October. (source)
It sounds like there are just a few stores so I must have got lucky to stumble into this one. I had heard rumors of some re-design, but I hadn’t seen anything out there on the Internet. Interesting. I’d love to see a study to understand satisfaction, engagement rates, retention, etc. associated with this footprint versus the older store pharmacy layout.
Is Your Adherence Program Leveraging Segmentation?
I was just finalizing a new marketing piece with our marketing team on Silverlink’s adherence services. I love this picture because it drives home the point of understanding the consumer.
If you don’t understand the factors that drive behavior and leverage those attributes in segmentation and personalization of your adherence program, you may be leaving opportunities on the table.
State By State Use of Rxs per Capita, Age, and Gender
(Note: This is retail only data so it’s not comprehensive, but it should be directionally accurate.)
The Kaiser Family Foundation puts out lots of data. One of their sites shows state by state analysis. Here is a map of utilization by state.
As you can see on the site, the top 5 states are (i.e., highest utilizers of prescription drugs):
- WV
- KY
- AL
- TN
- MS
The bottom 5 are:
- AK
- CO
- UT
- NM
- WA
For age breakdown, the data showed:
- 0-18 = 3.8 average Rxs
- 19-64 = 11.3
- 65+ = 31.1
For gender, the averages were 9.5 Rxs for males and 14.4 Rxs for females.
Note: All this data is available online at http://www.statehealthfacts.org/.
Videos from Kim Feil, Walgreens CMO
I was looking for something else and stumbled upon a few videos in YouTube by Kim Feil who is the Chief Marketing Officer of Walgreens.
CxO Roles In Pharmacy: A Quick Scan
I always find it interesting to see the senior roles created within organizations. While pharmacy doesn’t have many radical titles like Chief Executive Bear (aka Maxine Clark at Build-A-Bear), I did find the following looking at company websites, LinkedIn, and some quick Google searches:
- Chief Innovation Officer – Walgreens
- Chief Experience Officer – Walgreens
- Chief Supply Chain Officer – Express Scripts
- Chief Pharmacy Officer – Aetna, PartnersRx, Cigna, US Oncology, Tricare, United, Wellpoint, Excellus, CatalystRx
- Chief Sales Officer – PTRx
- Chief Strategy & Innovation Officer – OptumRx
- SVP Imagineering & Innovation – Medco
- Chief Trade Relations Officer – Express Scripts
- Chief Clinical Research & Development Officer – Medco
- Chief Healthcare Strategy & Marketing Officer – CVS Caremark
- Chief Scientist – Express Scripts
- Chief Strategy Officer – American Healthcare, Walgreens
- Chief Actuary – OptumRx
- Chief Branding Officer – Medco
Of course, there are always the obvious – CEO, COO, CFO, CIO, CTO, CMO (Marketing), CCO (Clinical), CMO (Medical), CCO (Compliance), and CAO (Accounting).
My takeaways from this list (which is likely incomplete) are:
- I would expect to see more Chief Innovation and Chief Experience Officers in the years to come.
- I continue to be surprised that there aren’t more Chief Pharmacy Officers.
Do you have others you’ve seen or companies that have these roles that my quick scan missed? Thanks.
Primary Adherence – Technology, Kaiser Study, and EHRs
I think we all know that primary adherence is a real issue. Depending on what you read, you see that anywhere from 20-30% (or more) of patients don’t start therapy. They are prescribed a drug, but they never fill it. This is due to lots of reasons:
- They get a sample.
- The drug costs too much leading to abandonment.
- They don’t feel like they need the prescription.
- They feel better.
- The doctor tells them only to fill it if something else doesn’t work.
These issues vary based on whether it’s an acute drug or a maintenance drug. It also varys by drug class.
I’ve always been surprised that pharmaceutical manufacturers focus so much on ongoing refills leading to improved MPR rather than focusing on primary adherence which would grow their market significantly. One of the big reasons for this has been visibility. Without electronic prescriptions and mapping those to claims data, it was hard to identify who had a prescription and didn’t fill it. You could do something with data out of the PPMS (Physician Practice Management System) or through more complicated processes to get data out of their notes, but it wasn’t easy.
So, this new study by Kaiser caught my attention.
If you are a diabetic, have high cholesterol, or high blood pressure and you receive medical care at an integrated healthcare system that has electronic health records (EHRs) linked to its own pharmacy, then you are more likely to collect your new prescriptions than people who receive care in a non-integrated system, a Kaiser Permanente study shows.
That’s a strong sell for an integrated model, but perhaps more realistically for the use of EHRs. You can also see some of the data from Surescripts around this topic of electronic prescriptions and adherence.
This creates a great opportunity for pharmacies, PBMs, payers, and pharmaceutical manufacturers to leverage technology to improve primary adherence. By identifying people who don’t fill a prescription they receive, companies can help determine which of those are intentional and which of those should be addressed. This should help address the overall costs attributed to non-adherence and be a business driver for all these entities.
[Note: If you’re interested in working on primary adherence, let me know. We have several approaches for this at Silverlink.]
Walgreens and Express Scripts: The Plot Thickens ($ESRX, $WAG)
Remember when this “conflict” was first announced a few months ago. If you’re like me, you probably assumed this would be over in 30-days like the Walgreens – CVS Caremark dispute last year. What’s different? I’m not sure. It seems like both sides are well dug in. (From my poll a few days ago of 22 of the readers of this blog, 65% felt this would get resolved by 1/1 and 25% felt that it would never get resolved.)
Now, it seems like both sides are continuing to take significant steps towards no resolution.
Express Scripts has apparently launched a pilot program to move share from Walgreens stores now using coupons. I believe the pilot was with Lowes and is about to expand to the Department of Defense. Additionally, I’ve heard that Express Scripts has sent out letters to their clients preparing them for a limited network starting 1/1/12 without Walgreens.
On the flipside, I’ve heard that Walgreens has begun putting signage out encouraging consumers to talk to their plans about excluding them from the network and for Medicare members to chose plans that aren’t run by Express Scripts. Walgreens also put out a whitepaper about what happens when you remove them from the network. This has some really interesting data in it.
Key Statement: Excluding Walgreens from a pharmacy network will result in little to no savings for most sponsors and patients, and in some cases will raise costs, while causing significant patient disruption and risking gaps in care, and increasing administrative costs on plan sponsors.
- As part of this document, they are encouraging payers to consider directly contracting with them and/or creating a custom network (if their PBM contracts allow for that).
- They state that their costs are comparable to other retailers or within 2% of their costs.
- They show some data from another PBM (not named) that modeled out network savings for them based on a limited network taking into account their drug costs, generic fill rate, and 90-day rates. It shows a jump in costs versus savings.
- They share data that their Generic Fill Rate (GFR) is 1.4% higher than the rest of the Express Scripts retail network which the paper says translates to $2 per Rx in cost.
- They say that 90-day retail generates a 6-8% savings compared to 30-day retail based on the pricing that they offered to Express Scripts.
Ultimately, I still believe resolution will occur before the end of the year. While both parties are dug in, I believe it’s a lose-lose situation for this to stay unresolved. That being said, there are lots of things that could occur here:
- This creates a wave of direct contracting between payers and pharmacies.
- This validates the integrated model of CVS and Caremark.
- This creates a large number of limited networks.
- This creates greater use of the Walgreens discount card and/or cash business at Walgreens especially for lower cost generics.
- Alienating Walgreens creates a disruptive force in the FTC review of the proposed Medco acquisition.
- Another PBM jumps in to do a creative deal with Walgreens which limits their long-term ability to work with Express Scripts.
- Express Scripts ends up in a shotgun relationship with CVS.
- The terms of PBM contracts get changed going forward based on new terms regarding retailers.
- Walgreens becomes a much more vocal voice in the retail world through NCPA and other organizations.
Between this and the proposed Express Scripts acquisition of Medco, the landscape in the PBM market could be radically different by early 2012.
[Note: As the stock market has dropped, I have continued to buy stock in the PBM industry including several of the specific companies mentioned in this post – MHS, ESRX, WAG and CVS.]
$47 Per Rx Guarantee From Prime Therapeutics
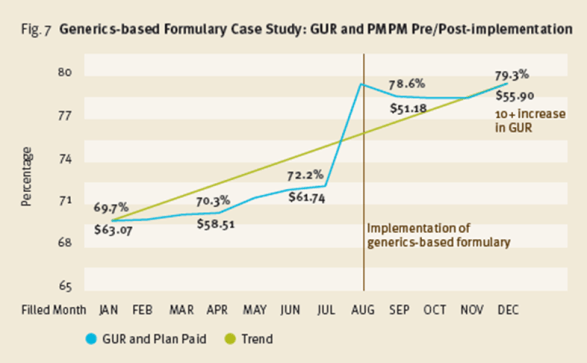
I think this is a good, bold move. Prime Therapeutics has launched four new programs. The most aggressive is called Reliance and guarantees your net spend per Rx at $47. The easy way to do this would be to exclude specialty drugs and basically offer a generics-only formulary. My quick read from their drug trend report and press release is that it includes specialty drugs. It also includes a lot of utilization management programs, suggestions on plan design, encouragement for mail order, and other features. I’ll be interested to see the adoption of the program or whether it’s just a great program to encourage clients to consider new, more aggressive plan designs.
“Our Reliance plan keeps costs predictable for plan sponsors,” said Michael Showalter, Prime Chief Marketing Officer. “The goal is to make pharmacy benefits easy, understandable and affordable. Through Reliance, there will be no surprises, allowing organizations to better plan for and manage their pharmacy costs and reduce overall health care costs, while providing excellent benefits. We provide a single number demonstrating the true cost of care – $47. We are the only PBM to back that up with a price guarantee and complete price transparency.”
Infographic: Hazards of Hospitals
Scary infographic from http://www.MedicalBillingandcodingCertification.net.
Highlights From the Prime Therapeutics 2010 Drug Trend Report
I just finished reading the Prime Therapeutics Drug Trend Report. As I highlighted the other day, their overall drug trend was 2.9%. Like in the past few years, they have jumped up to offer a report comparable with the other big PBMs. And, as we saw with last year’s report, the new management team is aggressive in using this to highlight research, their competitive differentiation, and point out why they are a competitive force in the market.
More interesting that just their success in drug trend was their “adjusted drug trend” for the other PBMs. You don’t often see this in your face marketing in this space, but they clearly want to show not only that their trend was better but that their methodology is better. (I don’t have the time to compare methodologies at this point.)
Fortunately, they don’t stake the argument on trend since as I’ve pointed out before – trend can be misleading. Sometimes higher trend is good as when it indicates better Medication Possession Ratio or better success at reducing gaps-in-care. They focus on five things in the document:
- Savings
- Safety
- Guidance
- Satisfaction
- Partnership
Their Generic Fill Rate (GFR) for 2010 was 69.2% which was lower than the 71% reported by Medco and the 71.5% reported by CVS Caremark. (I couldn’t find the Express Scripts numbers for whatever reason.)
The report focuses on some of the differences in the Prime model (client ownership, not public) and how that plays out in transparency and alignment.
They are now at 12 Rxs PMPY which to me still seems a little low. (I’ve mentioned this is prior reviews, but I don’t understand why their population usage is different.) To validate my hypothesis, I looked at the PBMI report from last year which shows PMPM utilization ranges by respondents (not industry averages).
I do think their example around implementing a generics-formulary along with their new benefit plan guaranteeing cost at $47 per Rx are very interesting. They remind me of the GenericsWork product I launched at Express Scripts and should offer some clients a great way to save money. They key, as I learned, was really understanding how to manage member disruption and gain buy-in to the offering. [Amazingly, a quick Google search led me to a cached image of the PDF from my product from 2004.]
They give some good MTM numbers:
- $1.29 in return for every $1 spent
- $86 in savings to the payer over a 10 year period per MTM encounter
They also announce a new offering for 2012 which they call the GuidedHealth care engine. There’s a little information in the document, but it sounds intriguing.
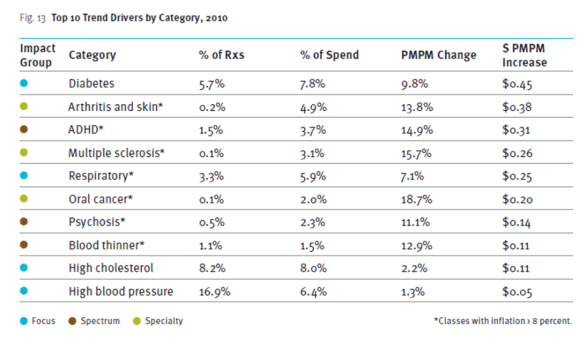
One of those typical charts that we all like to look at shows the drug classes that contributed most to driving trend.
I think their equation about overall cost…
Optimal cost = (medical cost + pharmacy cost) x health outcomes
One of my favorite charts is below which recognizes that there are two cost curves to focus on. The one for the relatively healthy which is often highly pharmacy focused cost versus the chronically ill that drive the majority of overall costs and is heavily medical and specialty medications.
Another study they share in here looks at the likelihood of hospitalization tied to adherence. Very interesting.
$7.60 PMPY savings for a limited network. Those are big numbers that they share from a case study around a client limiting their retail network by excluding one chain.
Their drug trend report looks at another hot topic – 90-day prescriptions. They share their results of a statin study looking at waste in 90-day retail and mail and 30-day retail and estimate the cost impact of the waste.
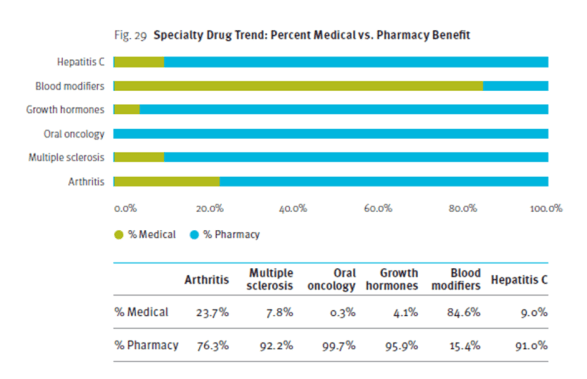
Another hot topic is the mix of specialty drug spend between medical and pharmacy. They share a chart looking at several of the large specialty drug classes.
At the end of the report, they give suggestions to clients on a spectrum of management (low to high). They also predict a few things in the next five years:
- A return to double digit trend increases after this generic wave;
- A generic fill rate in excess of 90%;
- Specialty drugs accounting for 40% of spend;
- Healthcare spending will increase 8-10% per year;
- The role of genetic testing will be validated; and
- Up to 25% of employers will drop benefit coverage.

 September 30, 2011
September 30, 2011