This is one of my favorite times of year. After working on the Drug Trend Report at Express Scripts for several years, I love to get all the trend reports from the PBMs and read them. The first one that I have had a chance to review is the one from CVS Caremark. I found it an easy to read document with good case studies and a mix of strategy and tactics.
Here are some of my highlights and observations:
- 3 out of 4 clients cited “reducing health care costs” as their primary measure of PBM success…AND 2 out of 3 prioritized “plan participant behavior change” as the way to reach that goal. [Maybe the plan design bigot is finally dead.]
- With pharmacy spend approaching $1,000 PMPY, I found their chart on potential cost reduction a simple way of pointing people to things they should think about.

- A 10% improvement in diabetes adherence can save $2,000 in annual health care costs. [I assume this is based on improving MPR and would definitely like to learn more on how the health care costs are quantified.]
- They layout three objectives – improve use of lower cost drugs, improve adherence, and get people to take better care of their health. [Similar to the concept I laid out in my white paper of needing to be broader than just Rx benefit management.]
-
They talk about two of their solutions:
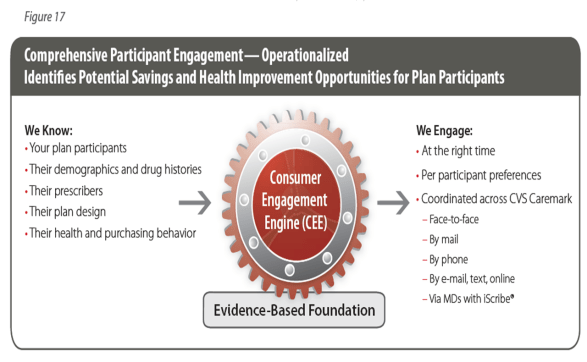
- Consumer Engagement Engine (CEE) which is very similar to what Silverlink does and provides business logic for targeting the right member at the right time with the right message.
- Proactive Pharmacy Care is their “medical neighborhood” concept to stitch together their entities – Mail Order, CVS retail, Specialty, MinuteClinic, and their disease management company.
- Consumer Engagement Engine (CEE) which is very similar to what Silverlink does and provides business logic for targeting the right member at the right time with the right message.
- Their trend was 3.9% PMPM in 2008 (or 2.8% excluding specialty drugs).
- Medicare Part D utilization was up 4.1% compared to 0.8% for the rest of their BOB (book of business).
-
Their GDR (generic dispensing rate) averaged 65.1% for 2008 and was 66.3% in December 2008.
- Best in class employers = 68.2%
- Best in class health plans = 73.4%
-
As they remind you, a 1% increase in GDR is roughly equal to a 1% reduction in pharmacy spend.
- [What I would like to see is improvements in GDR from new drugs coming to market in 2008 versus improvements that came from clients implementing plan design.]
- They say [which I preach all the time} – “proactive consumer engagement improves results and lowers the risk of disruption. For best results, provide personalized actionable information at a range of touchpoints.”
-
I saw a few interesting things in one of the case studies they share about their “Generous Generics” program. [Does that name get used with consumers? What’s their reaction to it?]
- $0 generic copay at mail [that should drive volume]
- 10% coinsurance penalty for not shifting to mail after the second fill [similar in concept (I believe) to the Medco “retail buy-up” concept]
-
Top Ten Therapeutic categories (53% of spend):
- Antihyperlipidemics
- Ulcer drugs
- Antidiabetics
- Antidepressants
- Antiasthmatics
- Antihypertensives
- Analgesics, Anti-inflamatory
- Anticonvulsants
- Analgesics, Opioid
- Endocrine and Metabolic Agents
-
They state that the population of diagnosed diabetics is growing by roughly 1M a year.
- Executive Summary, Economic Costs of Diabetes in US in 2007, American Diabetes Association, March 2008
- Executive Summary, Economic Costs of Diabetes in US in 2007, American Diabetes Association, March 2008
- They state that a generic for Lipitor is now expected in Q4 2011 [which I think is about a year later than originally expected]
-
They show some data from their Maintenance Choice program which I think has a lot of opportunity.
- This is where you can get a 90-day Rx from either mail or a CVS store for the same copay. [The key here is for them to understand member profitability and for CVS Caremark to understand how to drive consumers to the preferred channel.]
- [I would really need to understand their profitability by channel because if I read the chart in here right, it would appear that given the choice 45% of those at mail would choose 90-day at retail…a scary concept for mail order pharmacy.]

- They give a case on Maintenance Choice which leaves me looking for a key fact. They state that a recent implementation has a goal of 70% of the client’s day’s supply will go through the preferred network (CVS) or mail and that 20% of it goes through mail today. [What percentage goes through CVS today? If it’s a client in Boston, that one scenario. If it’s a client in Chicago, that would be another feat.]
- Specialty pharmacy trend was 13.5%.
- They say that pharmacogenomic testing is being used more frequently for specialty drugs. [I would love to know more…how often? For what drugs? Has it improved outcomes? Are their clients covering it? How are they playing in this space?]
- They talk about adherence which continues to be one of the hottest areas in the Rx arena today. They give stats showing 15-48% improvement across different metrics and up to $142 in cost avoidance in one case. [Are these again control groups? What was the cost / benefit analysis or ROI? Is this improvement in average MPR (Medication Possession Ratio) or improvement in the % of people with an MPR of >80%?]
- They talk about 88% of heart failure patients maintaining optimal prescription adherence compared to a norm of less than 50%. [My questions here (which isn’t apparent) is whether this was an opt-in program so the 88% is for engaged and active participants or whether it was across all targeted members.]
-
They provide a quick list of factors that will impact drug trend:
-
Driving costs:
- Aging
- Obesity
- Diabetes
- Specialty pipeline
- More aggressive treatment guidelines and earlier diagnosis [which hopefully would lower total healthcare costs]
- DTC advertising
-
Reducing costs:
- Economy – reduced utilization and improved GDR
- Increased availability of generics
- FDA safety reform
- Lackluster non-specialty drug pipeline
- Utilization and formulary management
- Consumer price transparency
-

 May 5, 2009
May 5, 2009 


This is an incredible study, BRAVO! I have pharmacists I’d like to share this post with – and reference the information. There’s components of the tools mentioned that could help empower the independents. Thank you!