I am now up in Minneapolis at our 4th Think Different event on how to engage the healthcare consumer. I talked about the first few speakers the other day, and I finally had a chance to hear the other speakers present. This week, I had the chance to listen to James Taylor (of Smart (enough) Systems fame not music) and Fred Jubitz (American Express). Here are a couple of my takeaways.
[Again, if you are coming to the upcoming events, this might be a little bit of a spoiler.]
A few notes from James’ presentation:
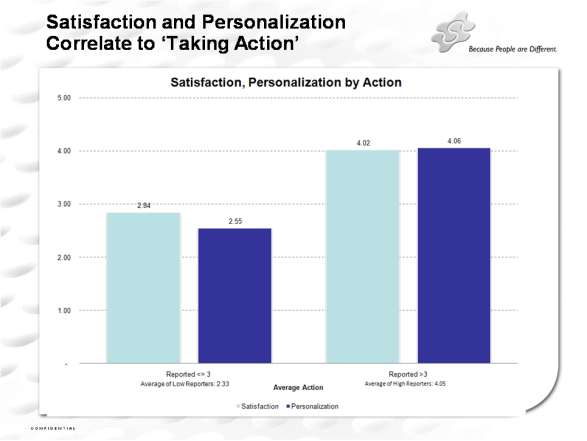
- He gave a great example of a program they did at Fair Isaac where they compared the standard, baseline program with one that was highly personalized. What was the improvement – 2,000%!!
- He gave a good real-life example of the need for channel coordination talking about buying tickets for the Chunnel and how he got different prices on the web and phone which were also different from the prices his father in England got using the same channels.
- The Chunnel example reminded me of something that someone told me the other day. They were using the Dell self-service example and pointed out that Dell now uses real-time chat right before you buy. They have found that this increases the average sale by 15%.
- The Chunnel example also made me think about how web technology allows us to do a lot of customization by visit, but most companies don’t do this. At the simplest level, I remember a competitor of Firepond (previous employer) where if I visited their website from work it looked one way and from home looked different.
- James talked about ATM customization as an easy example. How much money do you normally take out. Only showing you services that you have access to. Some of this is starting to happen, but not much.
- He also talked about rules creation and how that varies. I think it is always interesting to trace the evolution of rules and policies within a company. Are they there because of regulatory issues? Is it because someone coded the legacy systems that way? Is it based on a personal interpretation? Or are they dynamic and regularly reviewed? One of the worse examples that I have ever seen was a large healthcare company that believed that HIPAA required them to re-code everything as it moved from development to production. (A very costly error in interpretation.)
- He also talked about the evolution of interactions:
- Automate decisions
- Apply rules
- Segment customers
- Predict risk and value
- Optimize
- James hammered home the point of never stopping to try to optimize since as the environment and your customer base change the optimal solution might change.
Fred who ran the gold and green cards at AMEX talked about:
- American Express really wanted to be a lifestyle enabler not a payments company.
- He talked about the Centurian Card (black AMEX card) which apparently is able to charge $5,000 initiation fee plus a $2,500 annual fee. (Surprising that people still pay it, but I have heard examples of people buying a plane with their black card so I guess that level of service requires something.)
- He gave examples of how companies think about cards and showed a lot of affinity cards which made me think about groups and how people like to affiliate with others (e.g., by diseases).
- He talked about the importance of several things:
- Know your audience
- Key metrics
- Segmentation
- Personalize
- Continuous improvement
- He showed the standard framework for segmentation looking at size of wallet (i.e., how much you charge / spend per year) versus their share of wallet (i.e., how much of that is with AMEX). Each box on the grid then had a strategy – invest, retain, focus, divest, etc.
- He showed a lot about how the financial services companies can personalize the web experience, but he pointed out that this took months to develop as they built up your profile.
- I think a key point he made relative to healthcare is that a lot of a new member’s behavior was determined in the initial months which led to how they used their card. He gave an example of his blackberry. The first couple features he learned are all he uses.
- What are you doing in the initial months to “train” your members or be trained by your healthplan to use the website and leverage other ancillary services (e.g., gym membership) that they might offer?
- He stressed evolving your segments but not starting over each year or you will lose some of the lessons you have developed.
- Finally, as you always want to stress, he said to keep it simple.
Additionally, you can see some of Matthew Holt’s comments about the event at The Health Care Blog (here and here) and Les Masterson’s comments in The Health Plan Insider.

 June 5, 2008
June 5, 2008 

 I get a lot of solicitations to talk about products on the blog. I also get a lot of general e-mails. The ones I generally respond to are people giving me a heads up about an article, press release, technology, or something else that I just wouldn’t have known about. That doesn’t mean I will do anything about it, but if I have time and find it interesting, I will usually click through the link. And, if it still catches my attention then I will write about it.
I get a lot of solicitations to talk about products on the blog. I also get a lot of general e-mails. The ones I generally respond to are people giving me a heads up about an article, press release, technology, or something else that I just wouldn’t have known about. That doesn’t mean I will do anything about it, but if I have time and find it interesting, I will usually click through the link. And, if it still catches my attention then I will write about it. I certainly think that more targeting is better although I might not always want you to tell me how much you know about me.
I certainly think that more targeting is better although I might not always want you to tell me how much you know about me.