If you’re like me the answer is “of course”, but I realize that it isn’t always true for people. Look at the people who get sucked into things like SecondLife or people who play games for hours on Facebook. That certainly isn’t efficient time.
An article “The Internet Ruined My Life” by Pat Regnier in Money Magazine (Jan/Feb 2010) makes some good suggestions.
“When work got stressful – pretty often in this economy – it was all to easy to click over to Facebook.”
He points out that for Americans working over 50 hours per week:
- 56% say technology has increased their job stress (27% by a lot).
- 47% say technology has made it harder to focus at work (14% by a lot).
- 66% say technology has made it harder to forget about work at home and on the weekends (37% by a lot).
I’d say what about the fact that it’s easier to multi-task and watch your kids soccer game during the week and stay in touch.
He makes a few suggestions (all relevant for getting into the new year):
- Check out the 43folders.com blog.
- Break the circuit – stop checking Facebook for a week and see if it’s still that important.
- Be smarter about e-mail. The more you send; the more you get. Create better subject lines. He suggests the book “The Tyranny of E-mail”.
- Focus on your job (which isn’t to check e-mail…by the way). He suggests checking e-mail just a few times a day [which is very hard but very efficient].
- Stay offline in front of the kids [which is hard to do when you work from home].

 January 3, 2010
January 3, 2010 

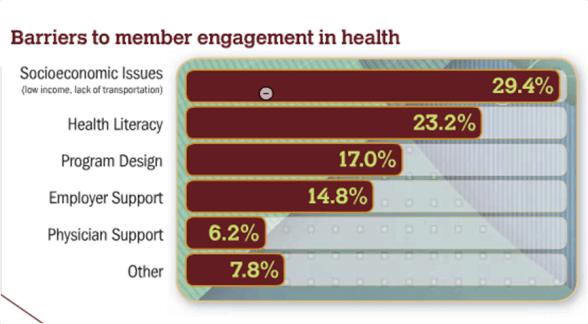
 Another part of the survey had 7.8% of people saying that patients (consumers) are less interested in health and that the primary reasons for lack of engagement were:
Another part of the survey had 7.8% of people saying that patients (consumers) are less interested in health and that the primary reasons for lack of engagement were: