The concept of the tipping point made famous by Malcolm Gladwell’s book is (in my words) the inflection point at which the market begins to adopt something and everyone jumps on the bandwagon.
So, with CMS saying that eRx (electronic prescribing) could eliminate as many as 2M prescribing errors per year, and Congress considering a bill to link Medicare payments to use of technology, will it make a difference. (I am pulling a few of these facts from Medco’s recent announcement about launching a Medicare Part D eRx initiative.) Only 3% of physicians use the technology today, and from my experience working with the vendors and physicians, there are still several big issues. Maybe this will address some of them.
- Standards – Will all the payors and PBMs share some standard such that a physician can move from system to system or from office to hospital without having to relearn a new application? Can they write prescriptions for the majority of their patients from one system or have to keep using different applications?
- Stability – Is there a vendor that they can trust? There have been several great concepts that were either before their time or had a flawed model. Time and money wasted on a system that isn’t supported leaves a bad taste in their mouth.
- Workflow – Does the system fit into their current office workflow? If not, why should they change behavior? Is it less expensive and disruptive for them to have the pharmacy or PBM contact their staff to address the issues after the fact? What percentage of the 2M errors wouldn’t be caught further upstream?
- Incentives – What’s in it for the physician? You are asking them to do more.
- Division of Labor – Who has what responsibility? For the PBMs, MCOs, and pharmacies, it is great to resolve issues at the point-of-care (POC) with the physician. Drug-drug interactions. Formulary issues. Brand to generic opportunities. Retail to mail opportunities. The physician could easily get overwhelmed with all the requests and go from a quick process to a difficult process.
- Support – What IT responsibilities come with the system? Who is supporting it? Does it impact the rest of their practice? Does it integrate with their practice management system? If they come to depend on the solution, what happens when it goes down?
- Cost – Who pays – physician, MCO, PBM, pharma (not likely these days)?
I know many of these are addressed in different ways today. I think we may be able to systemically force some of this into the office, but in general, until there is a generational transition in the physicians office (i.e., those in their 30s today are the high prescribers), I don’t think wide spread adoption will happen.
The value is clearly there. Even looking at the pilot statistics from the Medco pilot in Michigan, you see that there are issues and opportunities which can be addressed. These don’t even take into account the handwriting issues and other safety issues which occur.
- A severe or moderate drug-to-drug alert was sent to physicians for more than 1 million prescriptions (33 percent), resulting in nearly 423,000 (41 percent) of those prescriptions being changed or canceled by the prescribing doctor;
- More than 100,000 medication allergy alerts were presented, of which more than 41,000 (41 percent) were acted upon; and
- When a formulary alert was presented, 39 percent of the time the physician changed the prescription to comply with formulary requirements.
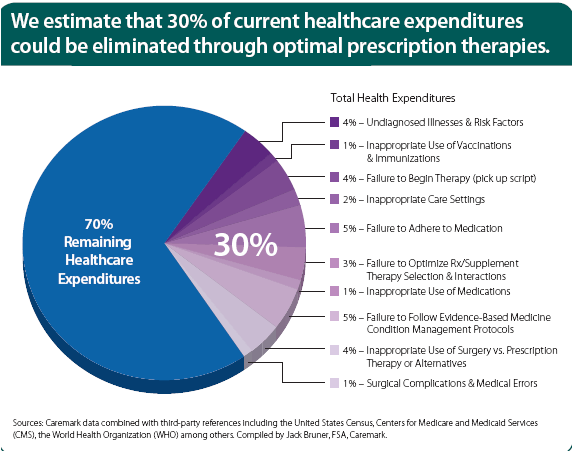
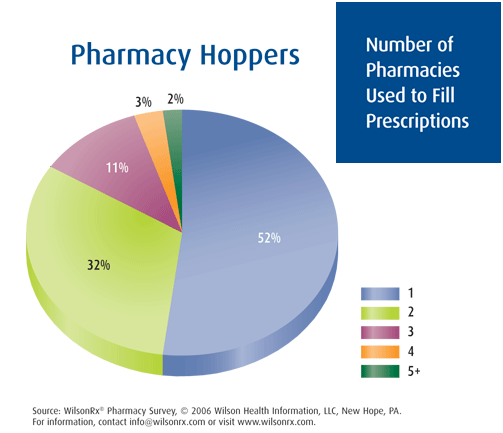
I personally think one of the most interesting opportunities will be to see who received a prescription and didn’t fill it and subsequently determining which of those estimated 30% of people should be filling the claim. The value of driving that initial compliance should be significant in avoiding more costly issues down the line.

 February 15, 2008
February 15, 2008