Today was our first Think Different event in Boston. This is a road show we are doing around our new positioning and how health care companies need to get outside the box to improve the effectiveness of their communications. It has four external speakers plus our CEO.
[Spoiler Alert: If you are attending an upcoming session, I may reveal some of the content here.]
I missed ½ the session today due to a client call, but I will be at 3 of the other 5 events. In listening to the first two speakers, I jotted down a few thoughts.
From Kinney Zalesne:
- She spoke about moving to the Starbucks economy and how we have much more choice today in what we do, who we love, religion, and our gender. Everyone immediately thinks of gender meaning sex change operations, but the point here is that there is a group of people who don’t want to be forced to select a gender identity. Before you discount it, you should know that 100 corporations, 75 colleges, and 8 states now ban discrimination based on gender identity. This was a bit of a surprise to me, but when I was talking with a large health plan about this, they informed me that their new EMR (electronic medical record) allowed for 5 possible gender options.
- She talked about people basically starving themselves to focus on the theory that has been demonstrated in animals, but not yet in humans which says that by eating 30% less calories you can extend your life by 40%. (Not something I will be doing.)
- She talked about the Do-It-Yourself (DIY) Doctors which are the people who use the Internet to self-diagnose and treat the MD as an ATM for drugs (i.e., I need a prescription for simvastatin can you please write it for me). I have heard a lot of talk recently about the changing perception of physicians. I haven’t seen the statistics, but one person said that they have lost the most respect over the past 20 years than any other profession. I think Kinney’s point is more about them moving from being a supervisor role (i.e., you should do this) to an advisor role (i.e., thanks for your opinion…I will take it into consideration).
- Her statistics about 5M working retired (i.e., >65 years old) and 2M working teens (i.e., using the Internet to make money before they leave high school) says a lot about how benefit design will need to change. The implications on needs and flexibility (e.g., imagine two primary addresses for snowbirds) could be significant.
-
In her talk about micro-targeting, my mind drifted to a few thoughts:
- How has gas prices changed our opinion of other costs? A $15 copay used to be equal to 7 gallons of gas. When it only equals 3 gallons of gas, do we view the $15 differently? [Have you caught yourself saying gas is only $3.75 at this one station near my house?]
- Just like your segmentation can change in healthcare, it is important to consider the macro-economic and political environment when communicating. Have you listened to all the car advertisements lately…they all talk about gas mileage?
- If you need a simple example of why personalization matters, think about buying a car. I am not a mechanical person so if I came in and someone talked to me about horsepower and cylinders then I would be turned off. I care about comfort and low maintenance.
- Finally, getting back to health, I thought about how difficult it is to be successful. Let’s assume there were 10 primary reasons for non-adherence and 3 primary channels for delivering information (live, letter, automated call). In this case, you have 10% chance of hitting the right message and a 33% chance of using the right channel (i.e., a 3% chance to be successful).
From Liz Boehm:
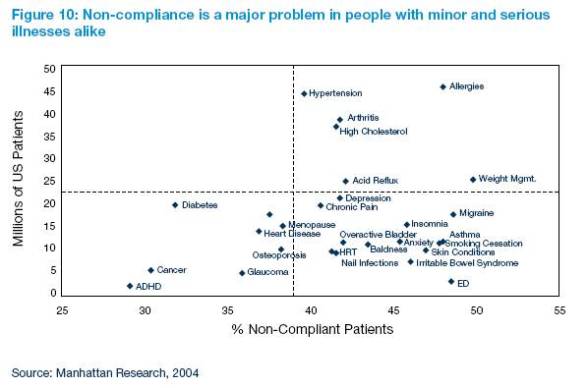
- She shared a lot of great facts about patient awareness of technology and how adherent they are.
- She points out a scary fact that while our health care needs are going up with the boomers we simultaneously have an issue with health care workers retiring which will only make things worse in the short term.
- She showed that 47% of people had visited their health plan’s website. [I will have to push her on this data since I believe they visited, but I think the percentage that log-in and use the site has to be very small. I would estimate 10-15%.]
- She talked about use of social media and gave an example of a MySpace group on diabetes.
- I found the discussion on wellness very interesting where she pointed out that things like chocolate, riding an elevator, or for some smoking gives you an immediate positive feeling while dropping your cholesterol by 10 points or even trying to lose 1 pound per week is pretty abstract.
- I have talked about loss aversion several times, and she talks a lot about it. Using it to make a link to why incentives matter in health care.
- Talking about motivation, I like her point that it isn’t a reasonable suggestion if you can’t achieve it. It may make good clinical sense to have a BMI of <25, but for someone with a BMI of 31, perhaps setting a goal of 28 is more reasonable and not as discouraging.
- In her talk about trust, it made me wonder how many people that work for managed care companies and pharmacy benefit management companies reveal that fact at cocktail parties. I am not talking about professional networking events, but your neighborhood events. Do you say who you work for and address their comments about service and/or coverage issues?
I finished my client meeting in time to hear Stan Nowak, our CEO and co-founder, speak and tie together the different points of view with some potential actions that people could take. As he often does, he talked a lot about the power of data and the fact that what’s new to health care is often old in other industries. We are an industry with the most data about people, but the least ability to use it effectively.
It’s also interesting to hear him talk about some of the “data exhaust” that is created by the analysis that the team does. These are facts that get revealed which may be surprising and may be things you never even thought to look for. For example:
- Patients with emphysema are 40% more likely to engage in a communications program related to additional coverage than patients with migraines.
- Patients with uncommon names are 18% more likely to complete a healthcare survey than those with common names.
- Males with depression are 83% less likely to do pill splitting than females with depression.

 May 29, 2008
May 29, 2008 
 I certainly think that more targeting is better although I might not always want you to tell me how much you know about me.
I certainly think that more targeting is better although I might not always want you to tell me how much you know about me.