I have been a big fan of Myers Briggs for years. Every since I took the test and realized that it described me to a tee. I even took an elective in graduate school to drill down on the testing and look at ways to use it in team development and other activities.
The purpose of the Myers-Briggs Type Indicator® (MBTI) personality inventory is to make the theory of psychological types described by C. G. Jung understandable and useful in people’s lives. The essence of the theory is that much seemingly random variation in the behavior is actually quite orderly and consistent, being due to basic differences in the ways individuals prefer to use their perception and judgment. (source)
If you haven’t taken the test, here is a site where you can answer a page of questions. I took it and it matched my end result from numerous testings. So why bring it up here? And, why is this entry 1 of X?
First, I am a big believer in trying to categorize individuals to make some assumptions about how to deliver healthcare information to them. This is one theoretical attempt to do this. Second, I am certainly not going to solve this tonight so I will layout a few thoughts and likely pick the topic up again.
The first category is Introvert (I) or Extravert (E). For me a healthcare introvert is someone who doesn’t talk about their family history or their individual ailments. If they feel sick, they will research it before making an appointment. Additionally, they may read online discussion groups but won’t participate. The extravert will ask everyone’s opinion about their condition. They want to tell you their cholesterol. If they feel bad, they go right to the ER or Urgent Care. And, if they have a chronic condition, they are active in online or physical groups.
The second variable is Sensing (S) or Intuitive (N). For me, the sensing healthcare person has a deep memory of their condition. They can tell you (and may even record) all the facts about their experience with a provider, drug, or disease. The intuitive healthcare person remembers the general patterns (e.g., every time I eat after taking my pill) and speculates on what this might mean. They aren’t focused on the specifics but more on the possibilities.
The third variable is Thinking (T) versus Feeling (F). The thinking healthcare person is consumed by the facts. They want to read the medical research and debate with their providers the treatment plan based on an article in the New England Journal of Medicine. The feeling person is much more driven by experience. If the placebo is helping them, they are willing to stick with it. Or, if their neighbor says that generics are not good, then they won’t buy generics.
The final category is Judging (J) or Perceiving (P). The judging patient is planning their care path or wellness. They participate in disease management. They go to preventive clinics. They get the flu shot even if they never get the flu. The perceiving person reacts to the events. They don’t have regular check-ups unless they are in pain. They don’t participate in any programs unless they are sick.
These are some initial thoughts, but we all know that figuring out a healthcare segmentation model that would predict behavior is significant. I don’t have the answer, but I think there is something here.
If you know your type and want to learn more, here is a good site I found. (http://typelogic.com/)

 November 12, 2007
November 12, 2007 


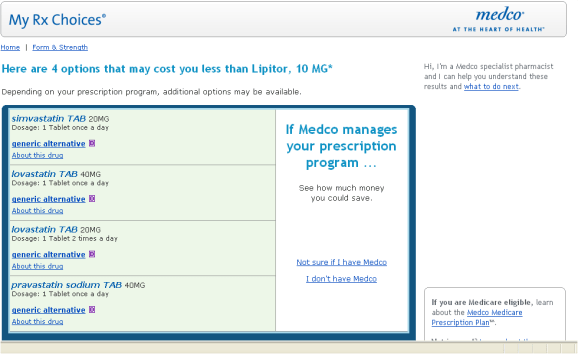
 Wouldn’t that be nice? Most of us don’t even know what the options are. We just get bombarded with information from our employer, managed care company, pharmacy, PBM, disease management company, wellness programs, HSA / HRA account manager, etc. Different messages. Different information.
Wouldn’t that be nice? Most of us don’t even know what the options are. We just get bombarded with information from our employer, managed care company, pharmacy, PBM, disease management company, wellness programs, HSA / HRA account manager, etc. Different messages. Different information.