This is a nice infographic on some of the ACO activity around the country.
Using Gilligan To Drive Colonoscopies
While I do applaud the creative concept here, I wasn’t overly impressed with the creative itself. At the end of the day, the question for me is results. Did it pay for itself? Did it get more people to get colonoscopies (in the target audience) than otherwise would have? I’m unsure of that.
Here’s what I did find in a HealthLeaders article…At the end of the day, I’d want to compare that to a program we did at my last company for UHG in this area.
The campaign also netted 44 colonoscopy appointments. Of those 44 appointments, 13 were current Good Samaritan patients and 31 were new to the hospital. Forty-three of the 44 scheduled an appointment through the call center and one booked online. Of those who called, 27 cited the radio spot as how they found out about the service. More than half of the patients were in the target group of 50–59 year olds, with 24 female and 20 male.
When Is It Good To Pay 300% Profit For A Medication?
Another interesting discussion at this Oncology event was about physician reimbursement for drugs. In Oncology, one historical source of revenue (~50%) for physicians has been the medications they dispense and administer in their offices. And, depending on who you believe, this has some degree of influence on what drugs they dispense.
The problem that was discussed is that today’s reimbursement model is ASP (Average Selling Price) plus 6% mark-up. This assumes that everyone buys at some price near that average which by definition means that not everyone does. One of the presenters suggested that physicians lose money on about 20-25% of the drugs they dispense and that it would need to be ASP + 12% for them to be positive on every drug. (I don’t know the math here and am simply sharing the dialogue as I found it very intriguing.)
The examples that they kept talking about in several presentations were that for a generic drug that costs $40 then their margin is theoretically $2.40 (6%) versus for a brand drug that’s $4,000 where their margin is $240 (or 6%). The suggestion was that if generics were reimbursed at 200-400% of ASP then it would take this economic factor out of the oncologists influence (when conscious or subconscious).
It’s an interesting debate. (Here’s some comments from another conference on this topic.)
On the flipside, some of this may go away with oral oncolytics being more common in the future (and therefore being more likely to be controlled by the PBM) although companies will look to enable in-office dispensing of these drugs also to help the physician from losing this income.
The other strategy being pushed has been called “brown bagging” where the patient is directed to obtain their medications from a specific specialty pharmacy and then bring those to the oncology practice for them to use. This eliminates the “buy-and-bill” approach but is not something that the physicians like (from what I know).
At the end of the day, I don’t really care. I think there are several key principles that if met would make me neutral to any solution:
- Are decisions made in the patient’s best interest or do financial implications impact clinical decisions?
- Is the safety of the patient impacted in any way?
- Is the patient experience impacted negatively in any way?
Some ACO Facts From Modern Healthcare and CMS
In a Modern Healthcare article about ACOs, there was the following graphic which is a quick snapshot. The key here is that companies are rapidly moving forward with ACOs (commercial and Medicare). The initial data is positive, and it seems like everyone is jumping on board.

Healthcare Transparency, Out-Of-Network Claims, and Technology Solutions
Another big focus area these days is around the creation of transparency solutions to enable consumers to make better cost decisions about their healthcare. While several companies have sprung up to work directly with consumers, the large payers have begun to rollout their own solutions. And, as you can see from the Towers Watson and National Business Group on Health 2012 Survey, this issue of transparency was the 3rd biggest focus area for 2013.
If you havent’ heard much about the topic, here’s several articles about the challenge of price discrepancies and surprise bills to consumers:
- Navigating out of network claims
- Healthcare price differences
- Healthcare bargain hunters
- Employers need transparency tools
- Shopping for surgery
Here’s what UHG and Aetna are doing:
A few of the companies to look at are:
Companies like GoodRx are creating solutions in this area.
You also might enjoy this infographic from Change Healthcare.
If you don’t believe this is a big issue in terms of price differentials, take a look at this data from the Healthcare Blue Book. This shows a huge swing in prices which depending on your plan design can directly impact your out-of-pocket spend.
| Test or treatment | Low | Fair | High |
| Brain MRI | $ 504 | $ 560 | $ 2,520 |
| Chest X-ray | 40 | 44 | 255 |
| Colonoscopy | 800 | 1,110 | 3,160 |
| Complete blood count | 15 | 23 | 105 |
| Hip replacement | 19,500 | 21,148 | 43,875 |
| Hysterectomy | 8,000 | 8,546 | 16,480 |
| Knee replacement | 17,800 | 19,791 | 42,750 |
| Knee arthroscopy | 3,000 | 3,675 | 7,350 |
| Laminectomy (spine surgery) | 8,150 | 11,744 | 25,760 |
| Laparoscopic gallbladder removal | 5,000 | 6,459 | 12,480 |
| Tubal ligation | 2,865 | 3,183 | 5,729 |
| Transurethral prostate removal | 4,000 | 4,409 | 8,875 |
| Ultrasound, fetal | 120 | 169 | 480 |
| Vasectomy | 700 | 1,003 | 2,100 |
Pediatric Cancer Article in EBN
“In the 1950s and 1960s, 4% of children survived with that diagnosis [leukemia]. In 2010, 80% to 85% of children in all risk categories survived and are cured.” Dr. Beverly Bell, Medical Director of the oncology program at inVentiv Medical Management
This is a quote from the June 1, 2012 article titled Trial and Error in Employee Benefit News. It’s an important fact as we watch cancer go from a terminal diagnosis and medical event to a chronic disease. Working with the survivors is something that Dr. Bell and I have discussed several times.
Here are some other facts from the article:
- 1/3 of childhood cancers are leukemias.
- 10,400 kids under 15 in the US were diagnosed with leukemia in 2007.
- About 1,545 of them will die fro the disease.
- Approximately 75-80% of pediatric cancer patients are put on a clinical trial.
The article goes on to talk about several things to consider:
- Plan language modifications.
- Access to pediatric oncology nurses.
- Access to a oncology network of centers of excellence.
- General support for the entire family perhaps through an EAP program.
- Hospice care.
- Medical travel / tourism.
Creating a holistic strategy to address oncology is a big effort and one that is critical to helping these patients.
A Few Basics On Health Risk Assessments
Like many of you, I’ve heard a lot about HRAs (Health Risk Assessments) for years. A few times I’ve even taken them. And, depending on your employer, you may even get paid to complete one. But, what are the basics about HRAs that you should know?
- What is a HRA? An HRA is a series of questions that can be administered over the Internet or by the phone or by a nurse to help collect patient reported data to help screen patients for chronic conditions or risk of developing a chronic condition based on their behaviors or other data. Additionally, they often lead to either immediate feedback on behaviors to address or lead to the patient being engaged into a program with a wellness, disease management, or case management.
- Should employees be incented to take an HRA? Incentives are basically used to increase response rates to the HRA. Not surprisingly, several studies show that incentives work, but education about the need to take the HRA is also important. In some cases, employers are even linking participation to premiums. Additionally, here’s a list of the top incentives used based on a 2010 study.
- How should an HRA be used? An HRA is a key component of an overall care management strategy. Like claims analysis, the objective of the HRA is a screening mechanism to identify patients who should be included in wellness, disease management, or care management program.
- Are HRAs valuable? There have been studies over the years that have shown a 2:1 or 3:1 ROI for wellness programs and a ROI for case management. HRAs are valuable in identifying more patients who should be enrolled in these programs.
- Should you combine biometrics with HRAs? Here’s a good study that shows that blending lab work with HRA data significantly increases the likelihood of identifying patients with diseases especially kidney disease.
Of course, no HRA is valuable if:
- You can’t get enough members to actually take the HRA.
- You don’t have an engagement strategy to get the members to participate in the program.
- You don’t continue to follow-up and help the member manage their condition.
- The member doesn’t get engaged in their healthcare.
Costs Of Presenteeism and Absenteeism
At the World Health Care Congress (WHCC), one of the presenters was making a great case for why employers want to continue to be involved in healthcare. Their point was that the costs of presenteeism and absenteeism are significant and make health a bigger issue than simply the obvious medical and pharmacy claims costs. (In one study, presenteeism costs alone were more than medical costs.)
While absenteeism costs are obvious as in sick days paid out, presenteeism is harder to estimate but can have significant costs. Presenteeism occurs when people come to work sick and are not productive.
I’m sure there are numerous methodologies out there, but I found this one that seemed simple and gave me some data by condition on both factors.
Why Blending Rx and Dx Data Matters
Yesterday at the PBMI conference, I was listening to a presentation on the blending of pharmacy and medical data. This has been the Holy Grail for a while although companies have struggled to do it well and successfully use it to affect change. That being said, I think it’s one of the biggest focus area for differentiation in the market today. From a large PBM perspective, you can look at the Guided Health efforts at Prime Therapeutics. From a payer software perspective, you can look at Active Health.
Some of the examples from yesterday were interesting data points that you’d never see without digging into both sets of data. For example:
Of course, the challenge is not only to identify them but to engage the patient and the provider in the best course of treatment looking at cost, outcomes, and patient experience.
NYT Article On ACOs Replacing Health Insurers
I think it’s a bold (maybe foolish) prediction that is made in the NY Times article saying that ACOs (Accountable Care Organizations) will be the end of health insurers. We don’t even know that ACOs will work yet. You can even see some debate on this topic in this blog post on Why ACOs Won’t Work.
But, I’m not an ACO expert so let me focus on what I found interesting in the NYT article. It points out a few things:
- The focus on preventative care
- The fact that some managed care organizations are changing (and others will too)
- The fact that “ACOs” (in whatever form they take) will need a platform
This is what I find interesting.
I think the concept of an ACO (or Patient Centered Medical Home) where care becomes localized and there is greater focus on prevention and wellness not just sick-care is great. We should all want that to happen in some form.
But, in all cases, this changes the data needs and role of the physician. They need to be empowered with new information and tools. How do they manage their panel of diabetics? Will some database track them and monitor their screenings and blood sugar?
When the field of medicine is constantly changing with new drugs and new studies, how will physicians have the best practices pulled into their practice? They won’t want to wait the 16 years it takes for things to work their way through the system. They’ll actually want to embrace the best solutions and see more comparative effectiveness information.
I see a huge opportunity here for someone to create an ACO “platform” that embeds business rules, tele-monitoring, consumer engagement, and reporting into a way to create the “i-physician” (informed physician) of the future.
Medicare Enrollment Up 1.2M (9.5%) in 2012
Based on new data from CMS as shared by CSFB in a report, the enrollment in Medicare Advantage through January 12th is up 1.2M to 13.3M. This is 27% penetration into the Medicare market. PDP enrollment was up to 19.69M a similar gain of 1.2M.
A quick summary of the big winners are:
- For Medicare Advantage (by percentage)
- Humana +13.5%
- Amerigroup +13.3%
- Coventry +12.2%
- For Medicare Advantage (by membership)
- Humana +262K
- United +132K
- Aetna +35K
- For PDP (by percentage)
- Coventry +25.3%
- Cigna +14.8%
- Humana +12.3%
- For PDP (by membership)
- Humana +312K
- Coventry +291K
- Cigna +80K
This is also interesting in light of Kermit Crawford (CEO of Walgreens) comment yesterday:
“Based on our preliminary analysis of the Centers for Medicare and Medicaid Services (CMS) data, Medicare Part D plans with Walgreens in their network gained market share in the aggregate, while those without Walgreens lost market share. Importantly, we were very pleased to see that those plans that included Walgreens grew nearly twice as fast as those Medicare Part D plans without Walgreens. In fact, several health plans that partnered with Walgreens grew significantly faster. For example, Coventry, who partnered with Walgreens and introduced a low cost Medicare Part D option, grew five times faster than the overall market.”
The one obvious account that he’s talking about is Wellpoint which lost 2,000 (0.3%) members in MA and 73,000 (11.6%) members in PDP.
Uping The RxAnte: An Adherence Predictive Model
Those of you that have heard me speak know that I look at this topic of predicting adherence both from an area of fascination along with the eye of a skeptic. While I love the concept of predicting someone’s adherence and therefore determining how to best support them from an intervention approach, I also believe that the general predictors are pretty straightforward:
- Number of medications
- Plan design (i.e., cost)
- Gender
- Health literacy and engagement (see PAM score research)
And, this is a hot topic (see post on FICO adherence score). You can see my prior posts on some different studies, on the Merck Estimator, and some notes from the NEHI event on this topic. It generated a good dialogue on Kevin MD’s blog when I talked about paying MD for adherence.
I had a chance to talk with Josh Benner the CEO of RxAnte the other day. It sounds very interesting, and they have an impressive team assembled. In general, they’re focused on:
- Predictive modeling
- Decision rules
- Monitoring and managing claims to track adherence
- Evaluating effectiveness of interventions
- And creating a learning system
There are definitely some correlations to the work we do at Silverlink Communications around adherence. We’re helping clients determine a communication strategy that might include call center agents, direct mail, automated calls, e-mail, SMS, mobile, or web solutions. We’re looking at segmentation and prioritization. We’re looking at past behavior and messaging. The goal is how to best spend resources to drive health outcomes from primary adherence to sustaining adherence. This is a challenge, and we all need to build upon the work that each other is doing to improve in this area. We have a huge problem globally with adherence.
Wellpoint Quote On Drug Copay Cards
This topic seems to be heating back up based on several posts on Adam Fein’s blog (Lipitor, adherence) and an article in Drug Benefit News where this quote appeared along with an AIS blog post questioning the PBM’s dislike of copay cards (from the same article that Adam mentioned).
“Copay offset programs [offered by brand-name drugmakers to compete with generics] mitigate the effectiveness of our tiered benefit design programs and [are] going against what we’re trying to accomplish for our members’ health and for employers.”
— Peter Clagett, vice president of pharmaceutical strategies and PBM oversight for WellPoint, Inc.
United HealthGroup At CES – Two Videos
This is Dr. Crounse from Microsoft talking about worldwide healthcare and using technology.
This is Dr. Reed Tuckson from United Healthcare talking about creating cost effective healthcare leveraging technology.
Who’s the 1% in healthcare?
As we all have known, healthcare costs are driven by the minority. According to the Agency for Healthcare Research and Quality, the top 1% account for 22% of healthcare spending in the US or about $90,000 per year. (USA Today article)
So, what are the characteristics of these people:
– White, non-Hispanic
– Female
– In poor health
– Elderly
– Users of publicly funded healthcare
Only about 20% of the high cost consumers stay in that bucket for two straight years…which I think is good. But, I guess you have to look at what percentage die during that period since a lot of costs are concentrated at the end-of-life.
Obviously it’s critical to develop solutions to engage and manage these patients earlier in the process. As data gets better, our predictive algorithms around conditions will improve and we’ll be able to intervene and prevent or delay cost in the system. The key of course is doing that in a way that fully engages the healthcare team and the caregivers.
Opportunists vs. Solidarity
With the Walgreens and Express Scripts dispute unresolved, you are certainly seeing more of an opportunistic attitude in pharmacies than one of solidarity. Maybe this shouldn’t be a surprise, but early on, I thought that the pharmacy groups would see Walgreens as their “leader” standing up to the large PBM. If the largest retailer can’t get negotiating leverage over the PBM, can anyone?
Now, if you go into my local grocery store (Dierbergs), you see signs about moving your prescriptions to them from Walgreens before it’s too late. You see and hear videos playing throughout the store talking about how to move your prescriptions and how easy it is.
CVS Caremark is predicting that it could see as many as 23M prescriptions move from Walgreens to CVS stores.
I’m certainly a fan of preferred or limited networks although I’m not sure I ever imagined a scenario where one PBM would totally exclude one of the big two retailers. I always imagined a scenario where you were playing them off each other and letting the client choose which one(s) to exclude.
You can see in the new whitepaper by Walgreens that they point out several things:
- The savings being offered / created is likely not enough for clients to want to exclude Walgreens and create the disruption.
- Clients who can include Walgreens are doing so and others would like to or believe they can.
- If Walgreens is excluded long-term, self-funded clients will be more likely to consider other PBMs.
- Many people still think this will get resolved in 2011 or by early 2012.
This brings up two other discussion topics:
- Will they come back? If the disruption happens (or has already happened), will consumers come back to Walgreens once they are back in the network? This will be a true test of satisfaction, branding, and many other efforts. On the flipside, the other retailers should be spending real effort welcoming and trying to retain the new consumers so they don’t boomerang back.
- Has the pressure shifted from Walgreens to Express Scripts? Depending on the timing, Walgreens will have felt most of their pain by mid-January. At that point, the pressure (IMHO) shifts to Express Scripts. Will they want to go through their 2012 selling season without Walgreens in their network, a major acquisition in the works, and any other potential distractions? I wouldn’t.
Smoking is an easy target for lowering healthcare costs
These statistics from the CDC really paint the picture…
– Smoking is estimated to cost businesses over $170 billion a year.
– Every smoker on the payroll is costing the company more than $3,500 annually in increased health insurance premiums, increased absenteeism and lost productivity.
– Smokers take, on average, 6.5 more sick leave days a year than non-smokers.
– Smokers cost 35-50% more to insure, a figure which is increasing rapidly as healthcare costs spiral.
– On average, up to 40 minutes of the working day is spent on smoking breaks, which equates to 21 working days of lost productivity per smoker per year.
This is certainly why you see companies trying to avoid hiring smokers. For those that show pictures of them smoking on Facebook or in other social media channels, this might be a risk (although I’m not sure if it’s legal to use that).
Cost and Outcomes Drive Better Use of Data
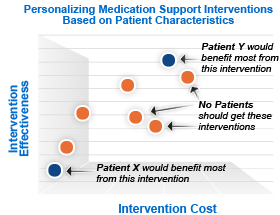
Overall, I would describe healthcare companies as trying to figure out how to drive the best outcomes at the lowest cost while maintaining a positive consumer experience. This isn’t easy. One area of opportunity that companies increasingly look at is how to use data to become smarter.
- Can I build a predictive model of response curves? Who’s likely to respond? Who’s likely to take action?
- Can I develop a segmentation model that works? How will I customize my communications after the segmentation?
- Can I rank and prioritize my outreaches? Should I do that based on risk or based on potential value?
Ultimately, I think this is driving companies to be a lot smarter and to look at how they use both medical and pharmacy data. For example, I’ll point to both CVS Caremark and Prime Therapeutics in press releases from earlier this year.
“The ActiveHealth CareEngine offers evidence-based information that can be used to improve the health care of our members and enables us to take our programs to the next level by seamlessly incorporating medical data,” stated Troyen Brennan, EVP and chief medical officer of CVS Caremark. “This agreement will enhance our existing programs to identify issues related to gaps in care, potential drug-to-drug interactions and duplicative care — information that is important to bring to the attention of the member’s physician.” (article that this is sourced from)
Smart use of medical and pharmacy data is one of the most powerful tools we have to improve outcomes and increase value for our members and clients,” said David Lassen, PharmD, Chief Clinical Officer at Prime. “Through ongoing partnership with health plan clients, Prime is uniquely positioned to view the entire spectrum of patient care, and we can leverage that information to help manage cost and to improve outcomes. We are very excited to collaborate with Corticon on the development of this clinical platform.” (press release)
The next step will be to integrate PRO (patient reported outcomes) from sources like connected devices and PHR (personal health records) that might show blood pressure, workouts, calories, or other data points that could help companies determine when to intervene and how to add value to drive an outcome.
Additionally, another key is continued work in the outcomes-based contracting world and bonus areas such as Star Ratings where the financial value is tied in the short-term to outcomes. This creates a burning platform for smarter use of data and use of a broader set of data to understand and impact care.
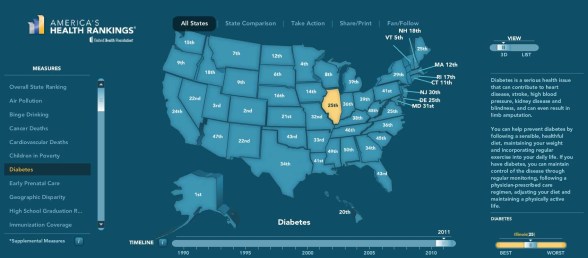
State By State Rankings – Key Healthcare Metrics
United Health Foundation published their Health Rankings today which offers some great statistics and interactive graphics to see how states compare on things like high cholesterol and diabetes. I pulled a few examples here, but it’s definitely worth checking out.
Medicare Patients Save $1.5B on Rxs!!
Now, here’s a great story. This may be one of the best government success that I’ve heard about in what I think of as a collaboration of the government with multiple businesses. (Although I think this is a lot more of what HHS is doing these days under Todd Park’s guidance.)
According to USA Today this morning, more than 2.65M Medicare recipients have saved an average of $569 per person this year based on addressing the donut hole with a 50% discount on the brand drugs filled during this time. And, the average premium for 2012 is actually LOWER than the premium in 2011 (by $0.76 per month).
The other part of the article is about the potential value of preventative care and leveraging this as part of the Medicare benefit. The key here is engagement of the participants to help them understand and take action on their healthcare. The power of the consumer in driving healthcare costs and outcomes is significant which is a topic that I know was discussed by several people today at the mHealth event in DC.
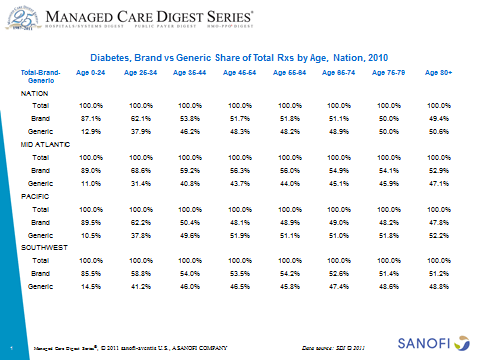
Managed Care Digest Sample Diabetes Reports
Sanofi sponsors the Managed Care Digest Series. I was looking at some of their data last night, and I thought I’d share two sample reports looking at diabetes retail pharmacy claims. A few things that this quick use of the tool shows you are:
Looking at the Brand and Generic mix of diabetes drugs based on payer, I notice 3 things:
- No significant geographic variance based on looking at a few regions
- People who pay cash are much more likely to choose generics while those with limited difference in copays (Medicaid) are more likely to choose brands
- Not a significant difference between Medicare and Commercial

In another view of the data, I looked at the brand and generic mix by age. Interestingly, it shows differences by geography especially in the younger ages. It also shows a clear correlation of age and generic utilization.
Utilizing The Same PBM For WC and Health Insurance?
While on the surface this seems like a natural opportunity for synergies, I’m not sure I really see this happening or simply wishful thinking by those in both businesses (see article about this). Since it’s not possible to track the same consumer as they move from one group to another within a PBM for historical data (i.e., when I change employers but stay with the same PBM), I can’t imagine aligning consumer profiles across divisions like Worker’s Compensation and Health Insurance.
And, while the market may be changing, there are real differences such as:
- Management objectives (get back to work and off the drug)
- Plan design (no copays, different formulary)
- Processing (different BIN at POS)
- Eligibility (there is no “eligibility” file until an incident happens to create a claimant)
In Worker’s Compensation, you also have an adjuster to deal with who is in the middle of the process and different legal frameworks to operate.
On the flipside, I agree that applying some of the processes that have worked in the traditional PBM business to WC has value it’s going to be very different. As the consumer, why do I want to use the generic when I don’t pay anything? There should also be some clinical value in coordinating the data, but the question exists of whether the consumer can be viewed with the same member ID in the adjudication platforms.
Slideshare: 2012 Digital Trends For Healthcare Marketing
Good deck that I found on Slideshare.net.
What’s A PAM Score?
PAMTM is the Patient Activation Measure which was developed by Dr. Hibbard, Dr. Bill Mahoney, and colleagues. It helps you gauge how much people feel in charge of their healthcare. To find out more, you can go to InsigniaHealth’s website.
Given the focus on health engagement across the industry these days, I think this is an important tool to consider. It’s been used broadly and has been validated in a lot of published studies. The questions lead people to be assigned to one of four different activation levels.

You can collect and use the PAM score for segmentation, developing customized messaging, measuring program success, and/or identifying at risk populations.
A few other interesting points from one of their FAQ documents were:
- Patients who are more activated are more likely to adopt positive behaviors regardless of plan design.
- People with higher activation levels are more likely to choose consumer directed plans.
- People with low activation often feel overwhelmed with the task of taking care of themselves.
- You increase the level of success in by breaking down change into smaller steps where the consumer has a greater likelihood of success.
The Dynamic Video Book: Aetna Example (Specialty Opportunity)

About a year ago, I picked up a “book” at an Aetna booth at a conference. I’d shown the technology to a few clients, but I’d never had a physical example. I thought I would share it here. When you open it up, it has a video embedded into the book. The video has several different options for messaging that you can view by pressing the buttons.

The cool aspect of the book is that it can be linked up to a computer so the videos can be updated over time. It’s produced by a company called Americhip who calls it “Video in Print”.
I’m sure it’s more expensive than a typical direct mail piece, but it can be used and updated over time. My thought is that this is a great tool for specialty pharmacy. These are high cost patients. Imagine a book with the following videos that came with their first script:
- Understanding your disease
- What to expect from your medicine
- How to access support
- Refilling your medication
- The importance of adherence
The content of these videos could change over time as their condition evolves, as they change medications, or even based on different lab values.
Reprint: Getting Aligned For Consumer Engagement
(This just appeared in the publication by Frost & Sullivan and McKesson called “Mastering the Art and Science of Patient Adherence“. It was written by me so I’m sharing it here also for those of you that don’t get that publication.)
According to the 15th Annual NBGH/Towers Watson Health Survey, employees’ poor health habits are the number one issue for maintaining affordable benefits. Since studies have shown that 50-to-70 percent of healthcare costs are attributed to consumer choices and adherence is one of those issues, the topic of how to engage consumers isn’t going away.
The challenge is getting the healthcare industry to use analytics and technology tools when engaging the consumer in a way that works for each individual and builds on their proven success in other industries. Healthcare has an enormous amount of consumer data ranging from demographics to claims and behavior data. Consequently, there is great opportunity to use this data to engage consumers in their health to improve clinical outcomes. While on the one hand, it’s like motivating consumers to buy a good, the reality is that healthcare is both personal and local which complicates the standard segmentation models.
This is a dynamic time where people are experimenting with different strategies for engagement. For instance, in medication adherence, people are trying everything from teaming those who have chronic conditions with community pharmacists to make sure they are taking their medications correctly to technology that monitors when the pill actually enters your body. But, there are still fundamental gaps in the process which can be addressed using interactive technology to complement the pharmacist interventions.
Consumer engagement in healthcare is increasingly moving to new channels with 59 percent of adults in the U.S. looking for health information online and 9 percent using mobile health applications according to Pew Research Center. Additionally, there is more and more participation in social media or peer-to-peer healthcare applications. Modes like SMS, which companies are starting to leverage in programs like Text4Baby or the diabetes reminder program recently launched by Aetna, are gaining popularity. Companies like Walgreens have also begun exploring the use of SMS and Quick Response (QR) codes for medication refills.
At the end of the day, consumers want preference-based marketing where they can elect how to best engage them, but that doesn’t mean that’s the most likely channel to get them to take action.They want you to learn from their past responses to improve your future outreach, but they are also skeptic about how their data is used. You have to put yourself in their shoes to create the optimal consumer experience. You have to deliver the right message to the right consumer at the right time using the right sequence and combination of channels.This is not easy.
So, if you’re going to optimize your resources and build the best consumer experience, you need an approach which is dynamic and personalizes each experience. For example, we found that creating the right sequence and timing around direct mail and automated calls improved results by as much as 100 percent in a pharmacy program. Or, in another case, at Silverlink Communications, we found that using a male voice in an automated call to Latinos got an 89 percent better engagement rate around colonoscopies. We also know that using a peer pressure message does not work in motivating seniors to take action in both a retail-to-mail program and a cancer screening program, but does work for those younger than 55-years-old?
You have to make simple messaging relevant to them—why should I get a vaccination, why is medication adherence important, how can you address my barriers? Only an ongoing test and learn approach to consumer insights will suffice, and those that figure this out will become critical in the ongoing fight for mindshare and trust. But, this isn’t a stand-alone opportunity. We have to partner with providers to improve engagement, adherence, and ultimately outcomes in different forms. We have to offer them a platform for engagement that is built upon consumer insights and provides a unique consumer experience to them based on their disease, their demographic attributes, and their plan design. All of these factor into their behavior and are important in “nudging” them towards healthcare engagement and ultimately, better health.
“Code Lavender” – Focusing On The Patient Experience
If you don’t know it yet, the consumer “experience” is rapidly becoming the hot topic. I’ve talked about it a lot beginning with companies like Cigna that have hired and staffed a consumer experience team and Chief Experience Officer. But, as the WSJ pointed out earlier this week in their article “A Financial Incentive For A Better Bedside Manner“, this is getting quantified in the provider world. One might argue that experience has always mattered more in the provider world since it’s easier to switch hospitals or physicians than insurance companies, but that is likely to continue to change as the individual insurance world and Medicare continue to create competition for the individual.
For payers, you can already see this individual market playing out with the growth of retail stores which is where the experience begins. In other cases, the PBMs and payers have to rely on many cases on their call centers as the front-end of the consumer experience. Additionally, with pharmacy being the most used benefit, this is another critical area. And, we know that pharmacy satisfaction is highly correlated with overall payer satisfaction.
But, let me pull a few things that caught my attention in the WSJ article:
Cleveland Clinic Chief Executive Delos “Toby” Cosgrove, a heart surgeon by training, says he had an epiphany several years ago at a Harvard Business School seminar, where a young woman raised her hand and told him that despite the clinic’s stellar medical reputation, her grandfather had chosen to go elsewhere for surgery because “we heard you don’t have empathy.”
-
The Cleveland Clinic calls their program HEART—for hear the concern, empathize, apologize, respond and thank. They also use the term “Code Lavender” for patients or family members who need immediate comfort.
I look forward to watching how this transforms over time. I know I’ve seen this play out in the dentist’s offices for my kids. The waiting rooms have video games and other things to keep them and their siblings busy, but I do agree with the article that this may unfairly bias the wealthier hospitals.
Sustained Patient Engagement Around Hypertension: Silverlink and Aetna
At Silverlink, we had a great opportunity to work with one of our clients and publicize it. This morning, Aetna released a joint press release with us about our hypertension program.
As companies continue to look at new ways to use technology to engage patients around chronic diseases, solutions like this offer companies a unique way to blend multiple channels into an overall consumer experience that improves engagement and outcomes.
From the press release:
The program also achieved high levels of engagement, with nearly 60 percent of participants continuing to actively monitor their blood pressure by using a free blood pressure monitor and submitting readings on a monthly basis. The frequency of participants’ cholesterol (low-density lipoprotein (LDL) cholesterol) screening also improved 5 percent.
“By helping our Medicare members manage their high blood pressure, we are hoping to help prevent heart disease, strokes and even deaths,” says Randall Krakauer, MD, FACP, FACR, Aetna’s national Medicare medical director. “Our nurse case managers work closely with our members and do a tremendous job providing them with the information, tools and support they need to help them control and improve various chronic conditions, including hypertension. The results of our program with Silverlink demonstrate that an automated program can further support and engage members in managing their own health conditions.”
One Challenge Of Medicare OEP – Satisfaction
We’re in the Medicare open enrollment period right now. This is a highly competitive time for MA and PDP plans to compete for new members and to get members to switch to their plans. I’ve talked about the Star Ratings process before. I’ve talked a little about the limited network offerings before.
This time, I wanted to focus on a recent study by Medicare Today that was put out on satisfaction. It shows:
- 95% say their current Part D plan works well, with 94% saying it is easy to use.
- 82% say their Part D plan offers good value.
- 67% say they have lowered their prescription drug spending.
- 34% say they used to skip or reduce their prescription medicine doses to save money, but now no longer have to do so.
- Two of every three seniors said they are unlikely to shop around.
Diabetes Facts From the ADA – Total Costs in US = $174B
I found this list of diabetes fact from the American Diabetes Association in an article I was reading:
- 25.8M children and adults in the US have diabetes (8.3% of the population). This includes 7.0M who haven’t yet been diagnosed.
- 1.9M new cases of diabetes were diagnosed in people 20+ in 2010.
- 215,000 or 0.26% of all people under 20 have diabetes.
- In 2007, diabetes was listed as the underlying cause of death on 71,382 death certificates and as a contributing factor on another 160.022 death certificates.
- Adults with diabetes have heart disease death rates 2-4x higher than adults without diabetes.
- The risk for stroke is 2-4x higher for people with diabetes.
- Diabetes is the leading cause of blindness among adults ages 20-74.
- Diabetes is the leading cause of failure accounting for 44% of new cases in 2008.
- Total cost of diagnosed diabetes in the US was $174B in 2007.
No wonder this is such a focus in the Medicare Star Ratings!

 December 31, 2012
December 31, 2012