It seems a logical evolution of the marketplace. Have we moved to a point where MCOs can really differentiate themselves based on their service? (The indicator for me on this would be whether consumers are willing to pay more out-of-pocket to have one plan versus another simply because of service.) It will certainly happen. Web tools. Pro-active communications. Personalized messaging. Educational programs. Friendly call center reps. Consumers care about these things.
Coverage, the AHIP magazine, had a recent article called “Creating a Culture of Service” which is about this topic. It talks about a health plan where the average call is picked up in 12 seconds, the call abandonment rate is 2%, and 88% of questions are resolved on the first call. I am not sure this is a sustainable model of differentiation since there is a floor to improvement. It is similar to the Kano Model which is used in Six Sigma. This model points out that there are different curves of expectations. Initially, you can delight a customer with something new, but it quickly becomes a standard expectation in the marketplace.
The article does point out a key point which is that patients expectations of service are not based on healthcare companies. They look at Starbucks, Nordstrom’s, Amazon, Dell, Disney, and other companies for what they expect in terms of online presence, response time, and service culture. In many companies, the call center agent is the first (and potentially only) point of contact for a patient (or member). They are not highly paid and often take the brunt of complaints all day long. Finding a way to make them happy and patient centric is essential.
Another challenge which exists in any human centric function like customer service is consistency. As benefits get more complex and companies have huge turnover issues at their call center, getting the same answer every time is difficult. Which is massively frustrating as a consumer. We used to have to do “secret shopper” calls constantly to determine what parts needed more training. This is of course one area where automated voice solutions are being used both inbound (reactively) and outbound (proactively) to address consistency and timeliness. In many cases, you can predict events that will drive a call and see a patient’s history to understand their probability of calling (versus using the web). Why not launch a call to them before the call which is less expensive?
One hiring model we saw work very well in specialty pharmacy was hiring people who had a family member with a chronic condition. They were empathetic. They understood the patient’s frustrations. And, they could project their family member’s experience. They were great.
BTW – The article has a great sub-story about what Connecticare has done in their call center to address recruiting and turnover.
Other things I have seen work are empowering the end agent to resolve an issue up to a certain level. If a person is complaining about a $5 copay change, it may be worth waiving it one time and sending them some information rather than taking 3 calls from them at $5 per call. Or, it may be worth providing a one-time override rather than spending 8 hours trying to resolve it.
Incentives along with metrics are also another obvious tactic. Definitely don’t incent them to get off the phone quickly. That always creates issues. Look at ways of turning them into “sales agents” for the company and reward them for getting patients to change behavior or based on satisfaction scores.
And, one thing to avoid that drives patients crazy is having different information on the web than at the call center. And, even worse is not letting the call center agents have Internet access so they can’t see what the patient sees.
There are a few words on technology such as CRM (customer relationship management) and voice recognition software (e.g., routing to a different agent based on an angry voice). This surprises me a little since I think using data to segment and address different patients differently. Are they a frequent caller that we should route to a live agent without IVR (interactive voice response)? Do we know why they might be calling and have an answer?
As I have talked about before, I believe MCOs and other healthcare companies will be differentiated based on communications. How do they use their data and a permission based marketing approach to understand the patient, push information to them at the right time using the right medium, and support their needs? That is what I am focused on building with clients.

 December 27, 2007
December 27, 2007 
 some family objectives, a financial planning objective, and a few personal objectives (e.g., run a 1:40 half-marathon).
some family objectives, a financial planning objective, and a few personal objectives (e.g., run a 1:40 half-marathon).

 Getting back to the article…He offers several good examples of sticky messages which are primarily what I would call rallying calls for organizations. In healthcare, the key is to find these simple messages that compel people to act. So, bottom lining it, he gives six basic traits:
Getting back to the article…He offers several good examples of sticky messages which are primarily what I would call rallying calls for organizations. In healthcare, the key is to find these simple messages that compel people to act. So, bottom lining it, he gives six basic traits:
 In
In 



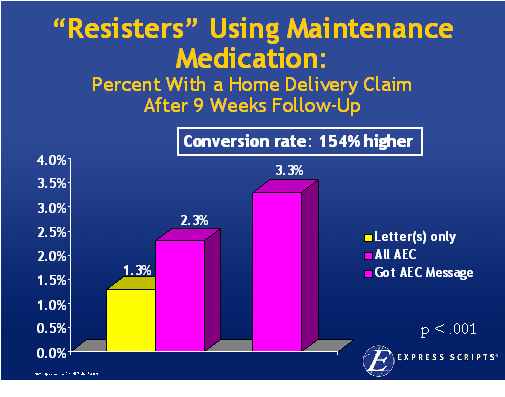
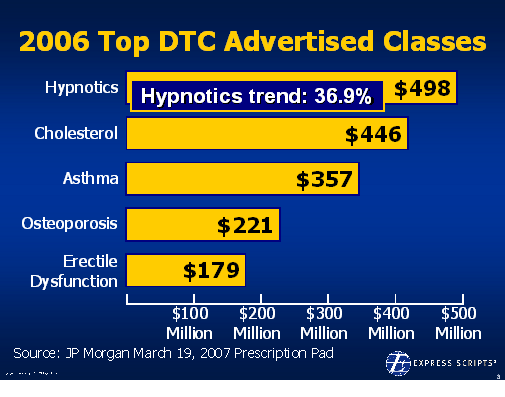
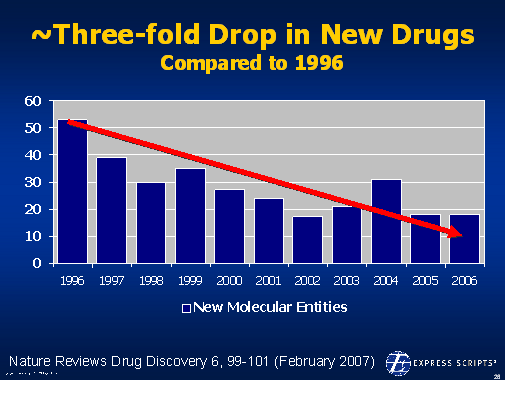
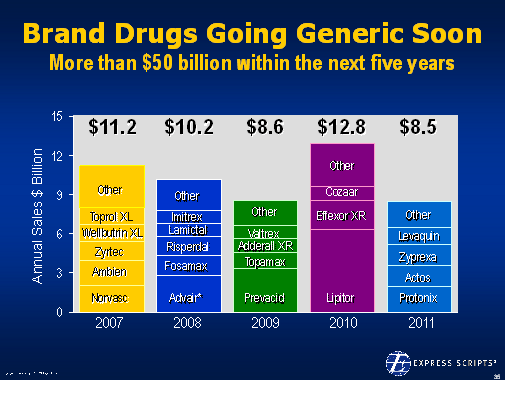

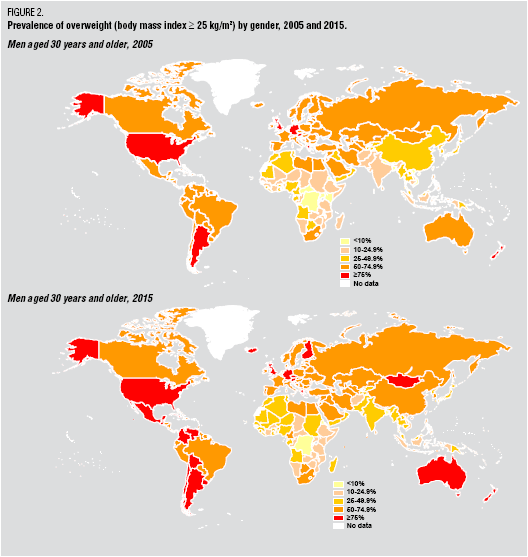
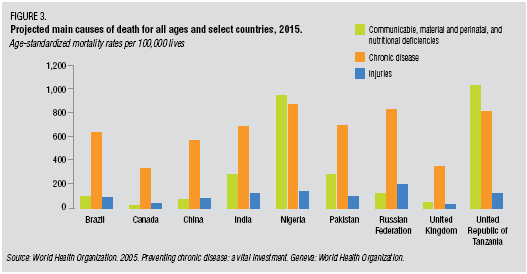


 There is lots of data out there validating this as a focus. In
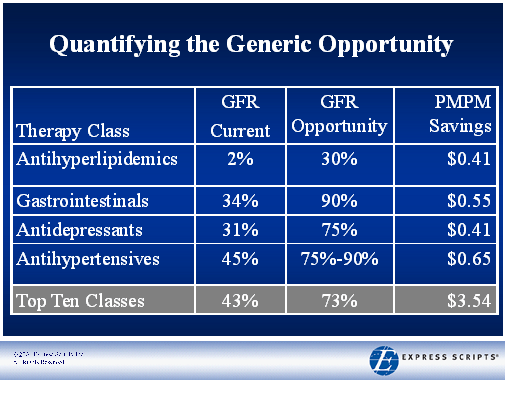
There is lots of data out there validating this as a focus. In  patients to try generic drugs. Earlier this year,
patients to try generic drugs. Earlier this year,