Without hesitation, that is the number one question I get from people in healthcare. Since seniors make up ~45% of the spend in healthcare, it would be difficult to promote a solution that didn’t work for that portion of the population. We have had some great success with the calls we have done around Medicare Part D and can provide a detailed set of data offline if you’re interested.
Here are a few of the key observations:
- If you use the Medicare Part D experience, you can see from the data that the CMS website was very busy during the week and much less so on the weekends. [Implying that the target population doesn’t use the Internet at home or had their caregivers or some public access facility helping them.]
- If you compare the 800# for Medicare Part D to the website volume, it is 4-5x as high. [Implying seniors use the phone primarily.]
-
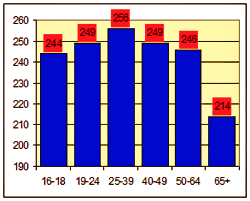
Comparing authentication by age for a refill program and a COB (coordination of benefits) program, the senior population (>64) responded best.
- Authentication means people that received an automated phone call and confirmed that they were the intended recipient (“are you bill jones?”).
- Once seniors started receiving the calls, they continued to be receptive over time to additional calls.
-
The likelihood of saying “repeat” during a call rose very slowly from 60 to 90 years of age.
- On an automated call, the patient has the opportunity to say “repeat” to hear the prior message again.
- We followed up on one call program and surveyed 70,000 seniors…95% said the messages were easy to understand and 91% said the calls were quick and helpful.
- Seniors answer calls all day, but more at night. [Gives you a good option for smoothing inbound call volume or transfers from outbound call programs.]

 December 10, 2007
December 10, 2007