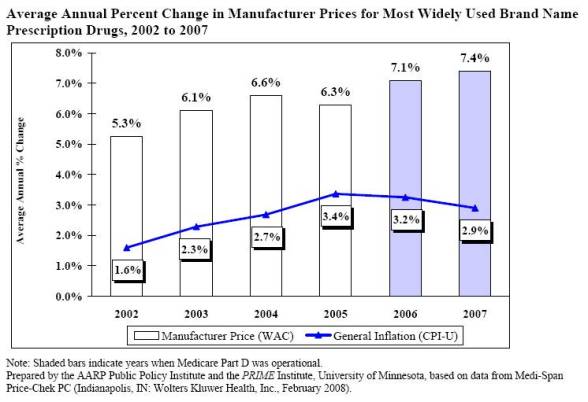
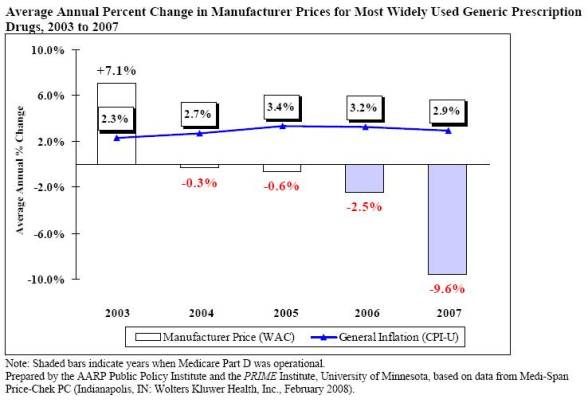
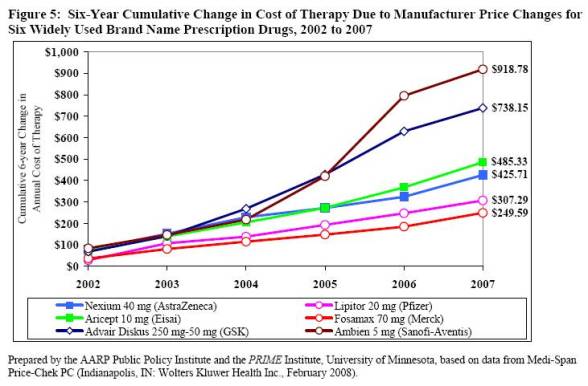
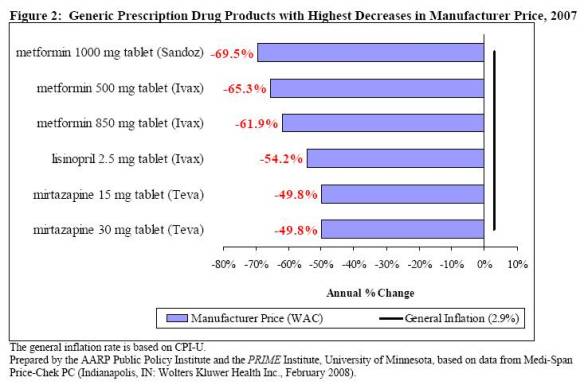
For those of you who are interested in this type of stuff, I think the AARP Watchdog reports (Brand Report, Generic Report) which track prescription drug prices over time are pretty interesting. (Note: This is for drugs most commonly used by Medicare recipients, but I think you’ll get the point.)
Why People Choose Mail Order Pharmacy?
I was looking for something else in the Express Scripts Drug Trend Report 2005 when I came across this study referenced on page 209. I should have remembered since I wrote this section (yes I was a contributor see page 332). This is a Morgan Stanley study which talks about why people choose mail order pharmacy.  Of course, the primary reason here is savings. The more savings the higher the likelihood of a person moving to mail order. This is a factor of savings per Rx multiplied by the number of maintenance drugs that an individual has that can be filled at mail order (or home delivery). This study shows the frequency of the response. If you focus on the weighted scores, you would see a dramatic cliff after savings. (I.e., 61% of people may choose mail for convenience, but they are much less likely to do it than someone with significant savings) So, why don’t all PBMs communicate exact patient savings to each individual? It’s hard. Given minimums and maximums; deductibles; percentage copays; and other benefit plan designs, the systems are stressed to produce this.
Of course, the primary reason here is savings. The more savings the higher the likelihood of a person moving to mail order. This is a factor of savings per Rx multiplied by the number of maintenance drugs that an individual has that can be filled at mail order (or home delivery). This study shows the frequency of the response. If you focus on the weighted scores, you would see a dramatic cliff after savings. (I.e., 61% of people may choose mail for convenience, but they are much less likely to do it than someone with significant savings) So, why don’t all PBMs communicate exact patient savings to each individual? It’s hard. Given minimums and maximums; deductibles; percentage copays; and other benefit plan designs, the systems are stressed to produce this.
Sprint Response
Just to continue on the Sprint story I posted the other day. The response time to get a live person was 5 days (but only 3 business days). I then received an e-mail and a voicemail message. Interestingly, when I call back the individual’s direct dial number (nice), her voicemail says “from the office of dan@sprint.com”. I am not sure if I will get the context to help relay my story to healthcare, but I look forward to the conversation.
Good afternoon Mr. Van Antwerp,
I am certainly happy to hear that you are enjoying the simply everything plan. I called and left you a message on your voice mail with my contact information. If you would like to call me that would be just fine. I am here Mon-Fri from 8 AM to 4 PM eastern time.
Thank you for your loyalty. We really do appreciate it. Have a great evening.
Sincerely,
Her Name
Sprint
Sell Your Captive PBM – Why?
I was a little surprised by the quote from Lisa Gill from JPMorgan Chase about why health plans should sell their in-house PBMs (Pharmacy Benefit Management):
“I think it makes a lot of sense for PBMs [pharmacy benefit managers] to be sold or spun off as a stand-alone business. The only time it will make sense for a managed care company to actually own a PBM is after they move to real-time [medical] claims processing. And that’s not going to happen near term.”
Maybe I am missing some context here, but I don’t understand. Why would you have a “captive” PBM (i.e., owned by a managed care company)?
- Able to align total healthcare interests (e.g., drive Rx usage up to manage ER visits)
- No conflicts of interest (real or perceived)
- Able to keep margins of the PBMs (look at the stocks of Medco, Express Scripts, and CVS Caremark)
- Manage the customer service experience
What does any of this have to do with real-time claims access?
Why would you use a standalone PBM? (Again an easy decision)
- Economies of scale on rebates
- Mail order pharmacy efficiencies
- Manage capital outlays
- Get a dedicated focus on pharmacy which as only 10% of the total healthcare spend will be a stepchild under a managed care plan no matter what
- Best practices being leveraged across companies
And, we all know from bidding on RFPs that managed care companies use this service to win business talking about the integrated solution and underwriting pharmacy with medical.
If you understand the rationale here, help me out.
Express Scripts Jumps Into Worker’s Compensation
Express Scripts has been in the Worker’s Compensation space for years now. As I suggested several months ago (see #2), buying a worker’s compensation PBM makes some sense. The margins are good, but it does require a different service model.
That being said, they jumped in last week with the announcement to buy the worker’s compensation PBM business from MSC down in Florida. It would have been intriguing to see them buy the other ancillary business that MSC has to get their footprint a little bigger. Now, this can go from being someone of a stepchild for Express Scripts to a major business unit. As Joe Paduda points out in his blog post, they have good teams at both organizations so they should be able to make some things happen in the market with a focused team, financial resources, and some efficiencies.
Given that fact that PMSI has been on the block, this may create a reason for a Coventry or a CypressCare to step in and buy them to gain more marketshare to take on Express Scripts.
A Few AIS Quotes Of The Day
I have a few more to post, but I often find their quotes interesting (www.aispub.com).
“Specialty medications require significant education for patients to feel confident self-injecting and achieve a successful outcome. For many patients, injecting a medication into the skin or muscle can be very intimidating. Because of the expense and the complexity of the medication, we cannot assume that the patient is just going to figure it out on their own.” Kari Amundson, director of specialty pharmacy services at Fairview Pharmacy Services, LLC.
“I think it makes a lot of sense for PBMs [pharmacy benefit managers] to be sold or spun off as a stand-alone business. The only time it will make sense for a managed care company to actually own a PBM is after they move to real-time [medical] claims processing. And that’s not going to happen near term.” Lisa Gill, a JPMorgan Chase analyst, speaking with AIS’s Health Plan Week about why health plans should jettison their in-house PBM units to shore up ailing profits.
“We went back and asked the 37,000 consumers we surveyed how long they had been with their last health plan, and found that the plans with the highest levels of involuntary turnover had the lowest levels of customer satisfaction.” Jim Dougherty, health care practice leader at J.D. Power Associates.
“The hepatitis C medications are pretty effective, but patients will feel much more sick from the treatment than from the disease, [so] companies that make those drugs are very willing to education patients” to improve their chances of remaining on the medication.” Mark Rubino, chief pharmacy officer at Aetna Inc.
George Paz (Express Scripts) on Adherence
Paul Levy who is the CEO of a hospital has a blog called Running A Hospital. He posted a summary the other day of a presentation by George Paz who is the CEO of Express Scripts. It has some good facts and there are several good comments on there about defining the terms in this area (see my old post) and whether these are reasonable rates of compliance. There is also a patient commenting about getting nurse calls and reminder e-mails which sounds great but puts them in the 1% of the population for which this happens.
The numbers do seem understated to me – 85% compliance with cholesterol lowering drugs. That might be the amount of people that get a paper prescription and then fill the drug or it might be the amount of people that get one refill, but I believe by month 6 or certainly by month 12 most compliance rates are closer to 50%.
There is clear value in adherence. Everyone should (in key therapeutic categories and using evidence-based standards) want to increase adherence to reduce total medical costs.
What surprised me most recently around this was what Kaiser had observed when looking at how doctors shared information with patients (Archives of Internal Medicine, Sept 2006):
- Only 74% of the time did the physician tell the patient the name of the prescription drug
- Only 35% of the time did the physician discuss adverse events with the patient
- Only 58% of the time did the physician explain the frequency and timing of dosing
A Few Blog Entries About The Think Different Event
We wrapped up the road show this week in Hartford and NY. I missed both events to be at client meetings on the west coast (and now down south). But, one of the presenters and someone who was in the audience posted entries on their blogs about the event:
- James Taylor on his blog Smart Enough Systems
- The Interactive Snack blog
The Automated Sprint Reply
As a reply to my e-mail (see my last posting), here is what I got. Now let’s see how long it takes to get a real reply.
Thank you for taking the time to write. To truly revolutionize wireless, we need your input. It’s people like you who are using our services everyday that can provide the best perspective. We’ll be looking through all the ideas and feedback we receive.
This will, of course, take some time. I appreciate your patience until we can get you a response. A representative from my office will be contacting you in about a week.
In the meantime, if you are interested in learning more about our new Simply Everything plan, you can find the details at www.sprint.com/everything.
Once again, from all of us at Sprint, thank you.
Dan Hesse
President and CEO – Sprint
Giving Out Your CEO’s E-mail
From the perspective of soliciting feedback, how many companies post their CEO’s or anybody’s real e-mail these days? Sometimes you can’t even find a number to call on the website. You simply get some generic form to fill out and get feedback. You sent it into the black hole and wonder if you’ll ever hear.
So, given Sprint’s challenges over the years, I think it was (is) a bold move to post the new CEO’s (Dan Hesse) e-mail (dan@sprint.com) at the end of some of their television commercials. I have been using Sprint as a great example of a company building loyalty because they reached out to me recently to move me to a better plan which reduced their revenue in ½. So, to test this e-mail address, I just sent the following. I will let you know what happens.
Dan (or whoever answers these for you):
I have been a loyal customer for 15 years now with Sprint PCS. I am not sure if that puts me in a minority, but I bet it does.
I was recently impressed when you guys called me to make sure I knew about the all inclusive plan (not sure of the actual name) which was something like $99 per month. Especially, since I was spending about $200 per month before. I work for a healthcare technology company and have been using that as an example about how to build loyalty.
I would be very interested (if you can share) how you guys made the decision to “down-sell” people and whether it has had the desired effect (which I assume is less churn).
The NY Times had an article about this on 6/9/08. Apparently, the initial response is an automated reply from Sprint, but most people then hear from someone on his staff (or likely a group of dedicated customer service agents) to address their questions.
“Yeah, we were worried,” said Mike Goff, vice president of advertising and marketing communications for Sprint. The company had a reputation for poor customer service, and soliciting critiques for the new chief to read was a risk. But, Mr. Goff said, Sprint wanted to “show we were serious about our intent to improve our customer service. We knew this was happening at a time when the perception of our customer service in the market was poor, so this is a chance for Dan to hear back from the market.”
The question is whether bold tactics like this can work to help change their image. If so, maybe health plans and PBMs should start posting their Chief Medical Officer, SVP of Customer Service, and CEO’s e-mails and see what happens. I can only image the look on some of their faces of doing something like this. Even though I am sure the reality is that he has a confidential e-mail address that gets used for internal purposes and personal purposes. As the Times article says, I am sure shareholders don’t want to think that the CEO sits in front of his PC all day answering questions.
Exercise Supercenter – Lifetime Fitness
Have you ever heard of Lifetime Fitness? I didn’t until they started building this huge facility near my house outside St. Louis. My first reaction was that somebody had the wrong business model. A million square foot gym in this economy. No way.
After an initial run in with an overly aggressive salesperson, my neighbors slowly signed up after their strong marketing push. Given that I primarily run, it seemed hard to justify, but everyone who I talked to that had been to one of their facilities raves about them. People compare them to country clubs (other than everyone in casual clothes) where there is great service and quality design and materials.
When you review their website, you get a much different view of the company. Not your typical gym. The facilities include a restaurant with healthy foods, a spa, and all of what you’d expect – classes, equipment, pools. But, they also provide corporate wellness programs.
It finally opened, and I had a chance to go there Sunday. Very nice. Lots of staff. Lots of equipment. Lots of people (but not too many). [I have no idea what the breakeven model is for a facility but it has to be 3,000+ members.] And, a great example of old world social networking was the fact that there were tons of people who we knew and who knew each other there. It was a destination to be at where hanging out at the pool was a social event by itself.
Since we know that peer pressure can influence wellness, it would be interesting to study the health dynamics in neighborhoods with a Lifetime Fitness versus other gyms and versus no facility. Could it be the catalyst or tipping point? It’s only a couple of days in, and I am on the west coast so we will see.
More On Silverlink’s Think Different Event
I am now up in Minneapolis at our 4th Think Different event on how to engage the healthcare consumer. I talked about the first few speakers the other day, and I finally had a chance to hear the other speakers present. This week, I had the chance to listen to James Taylor (of Smart (enough) Systems fame not music) and Fred Jubitz (American Express). Here are a couple of my takeaways.
[Again, if you are coming to the upcoming events, this might be a little bit of a spoiler.]
A few notes from James’ presentation:
- He gave a great example of a program they did at Fair Isaac where they compared the standard, baseline program with one that was highly personalized. What was the improvement – 2,000%!!
- He gave a good real-life example of the need for channel coordination talking about buying tickets for the Chunnel and how he got different prices on the web and phone which were also different from the prices his father in England got using the same channels.
- The Chunnel example reminded me of something that someone told me the other day. They were using the Dell self-service example and pointed out that Dell now uses real-time chat right before you buy. They have found that this increases the average sale by 15%.
- The Chunnel example also made me think about how web technology allows us to do a lot of customization by visit, but most companies don’t do this. At the simplest level, I remember a competitor of Firepond (previous employer) where if I visited their website from work it looked one way and from home looked different.
- James talked about ATM customization as an easy example. How much money do you normally take out. Only showing you services that you have access to. Some of this is starting to happen, but not much.
- He also talked about rules creation and how that varies. I think it is always interesting to trace the evolution of rules and policies within a company. Are they there because of regulatory issues? Is it because someone coded the legacy systems that way? Is it based on a personal interpretation? Or are they dynamic and regularly reviewed? One of the worse examples that I have ever seen was a large healthcare company that believed that HIPAA required them to re-code everything as it moved from development to production. (A very costly error in interpretation.)
- He also talked about the evolution of interactions:
- Automate decisions
- Apply rules
- Segment customers
- Predict risk and value
- Optimize
- James hammered home the point of never stopping to try to optimize since as the environment and your customer base change the optimal solution might change.
Fred who ran the gold and green cards at AMEX talked about:
- American Express really wanted to be a lifestyle enabler not a payments company.
- He talked about the Centurian Card (black AMEX card) which apparently is able to charge $5,000 initiation fee plus a $2,500 annual fee. (Surprising that people still pay it, but I have heard examples of people buying a plane with their black card so I guess that level of service requires something.)
- He gave examples of how companies think about cards and showed a lot of affinity cards which made me think about groups and how people like to affiliate with others (e.g., by diseases).
- He talked about the importance of several things:
- Know your audience
- Key metrics
- Segmentation
- Personalize
- Continuous improvement
- He showed the standard framework for segmentation looking at size of wallet (i.e., how much you charge / spend per year) versus their share of wallet (i.e., how much of that is with AMEX). Each box on the grid then had a strategy – invest, retain, focus, divest, etc.
- He showed a lot about how the financial services companies can personalize the web experience, but he pointed out that this took months to develop as they built up your profile.
- I think a key point he made relative to healthcare is that a lot of a new member’s behavior was determined in the initial months which led to how they used their card. He gave an example of his blackberry. The first couple features he learned are all he uses.
- What are you doing in the initial months to “train” your members or be trained by your healthplan to use the website and leverage other ancillary services (e.g., gym membership) that they might offer?
- He stressed evolving your segments but not starting over each year or you will lose some of the lessons you have developed.
- Finally, as you always want to stress, he said to keep it simple.
Additionally, you can see some of Matthew Holt’s comments about the event at The Health Care Blog (here and here) and Les Masterson’s comments in The Health Plan Insider.
GINA – A Good First Step For Personalized Medicine
Whether you are a patient or a health care company, I think you should be happy about this. GINA is the Genetic Information Nondiscrimination Act of 2008 which was signed into law on May 21st. It is a good step in encouraging individuals to participate in genetic testing without worrying about that information being used against them by an employer or health plan/insurer. It also bans companies from requiring genetic testing.
Based on an e-mail I got from Fulbright (a law firm where a friend practices), they offered the following definitions:
A. Genetic Information = includes the individual’s genetic tests, the genetic tests of family members of the individual, and the individual’s family medical history. Any information related to the individual’s or any family member’s participation in clinical research offering genetic services is included as is the genetic information of any fetus and embryo of an individual or family member of an individual who is pregnant. The sex or age of the individual is not considered genetic information, however.
B. Genetic Test = any analysis of DNA, RNA, chromosomes, proteins, or metabolites that detects genotypes, mutations, or chromosomal changes.
The use of genetic information (i.e., genomics) is a key step in creating personalized medicine. We know people are different and their bodies react differently to different drugs and different treatments. Some (much) of that can be attributed to their genetic make-up and likely to environmental factors.
The future holds a lot of promise once we can delivered personalized therapy that is specific to an individual. But, no one is going to get these tests if they distrust or worry about how the information is used. I have talked about this issue before when looking at companies like 23andme.
Wisdom Of The Crowd – Socializing Wellness
You probably caught the articles last year about how obesity seemed to spread throughout social networks. Now, in an article in the Washington Post (5/27/08), they talk about another example of research showing that smoking is similarly affected by social networks. Theoretically, this research could have significant implications for using social media (i.e., Facebook, MySpace, SecondLife). I can easily imagine blogs out there following people’s efforts to lose weight or quit smoking. I can see a Facebook “badge” or “sticker” congratulating someone for not smoking.
In a study published last week in the New England Journal of Medicine, the team [Nicholas A. Christakis, a medical sociologist at the Harvard Medical School, and James H. Fowler, a political scientist at the University of California at San Diego] found that a person’s decision to kick the habit is strongly affected by whether other people in their social network quit — even people they do not know. And, surprisingly, entire networks of smokers appear to quit virtually simultaneously.
Some of the observations that they found which seem interesting included the way non-smoking spread throughout a interrelated but not always directly related group. I don’t find that too surprising. If everyone quits and it is no longer “cool” or accepted you are marginalized and likely to feel pressure to quit. This was a concern that they noted which might lead to other negative health outcomes for the group that doesn’t change.
In a small group of my friends, I have seen one person’s efforts to lose weight (which included drinking less) impact the broader group. Others lost weight. Less beer is consumed when we get together. And, there is more discussion about the gym and running and other activities. For those who aren’t interested in those topics, they miss out on part of that dynamic.
- A person whose spouse quit was 67 percent more likely to kick the habit.
- If a friend gave it up, a person was 36 percent more likely to do so.
- If a sibling quit, the chances increased by 25 percent.
- A co-worker had an influence — 34 percent — only if the smoker worked at a small firm.
“It could be your co-worker’s spouse’s friend or your brother’s spouse’s co-worker or a friend of a friend of a friend. The point is, your behavior depends on people you don’t even know,” Christakis said. “Your actions are partially affected by the actions of people who are beyond your social horizon” — but in the broader network.
“People quit in droves — whole groups of people quit together at roughly the same time,” Christakis said. “You can see it ripple through a network. It’s sort of like an ant colony or a flock of birds. A single bird doesn’t decide to turn to the right or the left; the whole flock has mind of its own.”
From a employer, health plan, or even individual perspective, the question is how do we capitalize on this? How can we create wellness programs that leverage this “viral marketing” approach to drive behavior across the “colony or flock” to quickly and efficiently drive change. Certainly, this is where I see an opportunity for some of the Health 2.0 type of companies to play a role in creating communities and enhancing dialogues on key topics to enable this process faster and make the reach broader.
NCPA Survey on Adherence
I have been talking a lot about adherence lately (or lack of). A friend sent me the results of a survey of 1,000 adults by NCPA (National Community Pharmacy Association) from October 2006. This is now the 3rd study I have read this week with different results. Of course, they all used different channels – web, mail, and phone. And, I am sure that the questions asked were slightly different.
- While most consumers believe they are highly compliant when it comes to taking their prescription medications (64% said they follow their physician’s instructions “extremely closely”), the survey found they are not as compliant as they believe.
- Nearly three-fourths (74%) of respondents admitted to non-adherent behaviors in the past.
- Nearly half (49%) said they had forgotten to take a prescribed medication.
- Nearly one-third (31%) had not filled a prescription they were given.
- More than one in 10 (13%) had taken someone else’s prescription medicine.
- Nearly one-quarter (24%) had taken less than the recommended dosage.
- Nearly three out of 10 (29%) had stopped taking a medication before the supply ran out.
- More than one in 10 (11%) substituted an over-the-counter medication instead of filling the prescription they were given.
- Nearly four out of 10 (38%) had forgotten whether they had taken a medication.
- Less than half of respondents (48%) said they had consulted their doctor or pharmacist before making these changes.
- An overwhelming 90% of respondents saw non-adherence as a serious problem.
- More than eight out of 10 (83%) respondents agree that pharmacists can play a role in improving adherence by helping to make sure patients are taking their prescription medications correctly.
- More than two-thirds (68%) believe pharmacists are more knowledgeable than other health care professionals when it comes to information about prescription medications.
- Two-thirds (66%) go to one pharmacy for their prescription medications, which presents an opportunity for pharmacists to advise patients how to take their medications properly.
- Nearly nine out of 10 (86%) say they would be likely to talk to their pharmacist about their medications.
When Would I Pay More – Z-Lists and Green
The other day, someone was talking to me about the Z-List at Harvard. Basically, Harvard will allow a certain number of students to come in if their parents give $1M. Makes sense, and it allow them to provide lots of other students with aid.
At the grocery store, we pay a premium for organic foods.
We pay a premium for green buildings.
We pay a premium for energy derived from sustainable sources (e.g., wind).
Yet, in healthcare, we are always focused on how to lower premiums and/or ashamed of the constant increases.
- Is there a place for a premium product with a different service model? E.g., no inbound IVR…you always talk to a live agent
- Is there a place for more bundled services? E.g., vision, personal health concierge, OTCs
- Is there a place for a wide open formulary? E.g., every drug is covered for a flat copay of $10
- What about a preventative care plan that focused on getting you better?
The one that immediately jumped to my mind is pre-existing conditions. I am sure the underwriters could figure it out like Harvard, but why can’t I pay a one-time penalty or annually higher rates to be insured even with my pre-existing condition and maybe I can earn credits for being preventative.
It ultimately gets to the idea of personalized insurance that is specific to me where I weigh my need for simplicity, my financial assets, and my risk profile against the insurance companies underwriting model for risk management.
Variance In Children’s Healthcare
I think state-by-state variance in basic statistics is fascinating. It seems like we should have standardized around some fundamentals by now, but the variances continue to be significant.
In a recent report out by The Commonwealth Fund, it showed some wide variation:
- Only 46% of kids visit the doctor and dentist at least once a year in Idaho, but 75% of Massachusetts children do.
- Infant mortality rates are 2.5 times higher in the District of Columbia than in Maine.
- Kids in South Carolina are 5.7 times as likely to wind up in the hospital for asthma as those in Vermont.
- The percentage of children who received five recommended vaccinations from ages 19 months to 35 months ranges from 94% in Massachusetts to 67% in Nevada.
- Utah has the lowest spending per person at $3,972. The District of Columbia has the highest at $8,295.
| State |
Overall rank |
| Alabama |
14 |
| Alaska |
41 |
| Arizona |
47 |
| Arkansas |
44 |
| California |
34 |
| Colorado |
34 |
| Connecticut |
14 |
| Delaware |
37 |
| District of Columbia |
31 |
| Florida |
50 |
| Georgia |
38 |
| Hawaii |
7 |
| Idaho |
33 |
| Illinois |
38 |
| Indiana |
22 |
| Iowa |
1 |
| Kansas |
10 |
| Kentucky |
9 |
| Louisiana |
48 |
| Maine |
3 |
| Maryland |
27 |
| Massachusetts |
4 |
| Michigan |
12 |
| Minnesota |
23 |
| Mississippi |
49 |
| Missouri |
28 |
| Montana |
28 |
| Nebraska |
13 |
| Nevada |
45 |
| New Hampshire |
5 |
| New Jersey |
42 |
| New Mexico |
40 |
| New York |
25 |
| North Carolina |
31 |
| North Dakota |
21 |
| Ohio |
6 |
| Oklahoma |
51 |
| Oregon |
43 |
| Pennsylvania |
19 |
| Rhode Island |
8 |
| South Carolina |
36 |
| South Dakota |
16 |
| Tennessee |
30 |
| Texas |
46 |
| Utah |
26 |
| Vermont |
2 |
| Virginia |
23 |
| Washington |
18 |
| West Virginia |
20 |
| Wisconsin |
11 |
| Wyoming |
16 |
PBM Satisfaction Survey
It should be out soon, and it will be interesting to see the data. The WilsonRx PBM Satisfaction Survey is the only (I think) independent survey done of the industry. [Although I never remember paying attention to it at Express Scripts.] From what I know, they seem to get a good sample of more than 25,000 responses rating 18 PBMs (Pharmacy Benefit Managers).
Some of the new factors they are including:
- Overall Medicare costs and availability
- Annual increases in premiums or costs
- Overall delivery of pharmacy benefit services
- Courteousness and helpfulness of PBM plan representatives
- Ease and timeliness regarding conversations with a PBM representative
- Ease and ability to access prescription records and order refills
- Resolution of denied drug claims or appeals
- Overall quality of care
- Adequate coverage of treatment medication needs
- Personalized care for Rx needs
They seem like logical factors, but some of them aren’t controlled by the PBM but by either the self-insured employer or the managed care company (1, 2, 9). Depending on the service model, several others may be done by the managed care company (4, 5, 6, 7). And, I have no idea of how they are going to gauge things like overall delivery (3); quality of care (8); or personalized care (10). I hope they at least look at how responses vary by high utilizers versus low utilizers (of drugs) along with the type of coverage (which I doubt the individual knows whether their pharmacy coverage is through Aetna’s PBM or Medco (for example)).
Walgreens Health Initiatives (WHI) won the award last year and is certainly building a very competitive offering:
- A goal of 10,000 retail locations
- Mail pharmacy
- Specialty pharmacy
- 90-day at retail
- On-site (or worksite) pharmacy
- PBM
“While we already knew from our own surveys that members are highly satisfied with the wide selection of innovative products and services we offer, it was gratifying to have it confirmed by an independent third-party,” according to Richard Ashworth, Pharm.D., MBA, executive vice president for WHI, a wholly owned subsidiary of drugstore giant Walgreen Co.
He believes member satisfaction ultimately boils down to choice and convenience, noting how a 90-day medication option at the retail level serves as an important mail-order alternative for those who prefer face-to-face consultations with a pharmacy team they know and trust. Of WHI’s national retail network of more than 62,000 pharmacies, more than 39,000 offer this option and the number continues to grow.
Walgreens also offers worksite pharmacies on many corporate campuses across the U.S., which encourages employees to be more proactive about their health and, in turn, helps reduce absenteeism and the overall health care spend. Serving just one employer allows pharmacists to focus solely on that particular patient population, maximizing plan design and wellness strategies as part of a tailor-made approach to comprehensive care.
Pharmacists can help engage, educate and empower employees, as well as provide informed feedback on clinical prior authorizations, therapy-specific programs or the impact of formulary changes on medication options. There’s also room for leveraging a company’s core cost-containment strategies by promoting generic utilization, formulary efficiency and other key clinical programs whether or not WHI is the plan’s PBM. (Text from article by Employee Benefit News)
The Doctor Will See You…IF You Promised Not To Critique Them
It takes a lot for me to get offended, but I find this offensive. The WSJ Blog mentioned it this morning, and when I clicked through the links, it seems like a total disconnect with the technology world.
Medical Justice Inc. has put together a contract physicians can ask their patients to sign. In it, patients promise not to post anything about their experience, good or bad, without your prior approval. The organization calls it a “vaccine against libel.” (AMA article)
This seems ridiculous to me. Don’t we all have reputations that we work and go to school to create and protect. Doesn’t every business have a brand equity that they work to protect. This is nothing new. So trying to create a fascist environment where public comment about your services is not allowed is ridiculous.
What’s next? Hotels that won’t let you stay there unless you don’t rate them. eBay not allowing feedback on buyers and sellers. Architects not letting you visit their buildings unless you promise to like them and not comment about them.
This is a new economy which is driven by consumers. Healthcare is going to be part of that like it or not. Patients should have choice and should have transparent access to how physicians and other providers perform. I am not against establishing some standards in terms of how the experience is evaluated, but censoring speech seems like the WRONG way to accomplish this.
Why don’t they focus on helping the physician create a positive experience, be responsive to criticism, and get patients that like them to post their comments. We all realize that one or two people can be negative about a person or company, but that can be outweighed by a hundred positive reviews.
Pavlovian Response To Sound
We recently got a new dog (a Tibetan Terrier), and we decided to start training the dog using the clicker method. I kiddingly commented that it would be great to have something like this to train people. Apparently there already is such a method, and it can be used as a teaching method for autistic children (for example) along with sports training.
Basically, clicker training is an audio reinforcement for positive behavior…think whistle with dolphins. TAG Teach is a website where you can learn more.
What I found interesting is how to link this in with sonic branding and the Pavlovian response concept. Could I create an audio sound that drove behavior? For example, I have my dry cleaning dropped off and picked up at my house. They use an automated call to remind me to set it out. All I have to do is pick up the phone and hear the voice. Once that happens, I know what to do and hang up on the call.
TAG stands for Teaching with Acoustical Guidance and uses a sound marker to indicate correct performance.
The TAG refers to the distinctive sound made to mark or “TAG” a moment in time. This sound becomes an acoustical binary message, a sort of “snapshot” that is quickly processed by the brain.
A TAG means “yes.” Absence of a TAG means “try again.”
The student no longer has to perform a time-consuming language analysis while attempting complicated movements. The immediacy and clarity of the feedback allows the student to form a mental picture of the movement or position.
TAG points are the individual pieces of a desired response action or position. Students receive a TAG (the click sound) when the points are correctly performed.
The set up for a golf swing may have TAG points for grip, body position, foot placement, and club placement. The swing component may have TAG points for hand, arm, and club position at the top and end of the swing, TAG points for leg position, arm position, and weight transfer during the swing. With a beginning golfer a limited set of key TAG points are defined and executed individually. With an experienced golfer a diagnosis is performed and TAG points are identified based on technique errors requiring correction.
Kid’s Cancer Highest In Northeast
I think this is an interesting analysis, but I don’t think it shows any causality just correlation. The key questions (as reported) are whether there is an issue here (e.g., greater exposure to radiation) or just a difference in reporting or access.
The study was just released by the CDC. It showed that cancer effects 166 out of every million children or 0.017%. Rare, but very tragic.
- The highest rate was in the Northeast with 179 cases per million children.
- The lowest was among children in the South with 159 cases per million.
- The rates for the Midwest and West were nearly identical, at 166 cases per million and 165 per million, respectively.
- The cancer incidence in boys was 174 cases per million, compared with 157 cases per million in girls.
- In white children, the rate was 173 per million, versus 164 per million in Hispanics and 118 per million in blacks.
- Teenagers had higher rates than younger kids.
You Only Have To Be Compliant For 10-Days…What Happened?
On the topic of non-compliance, I found this a pretty pathetic statistic:
56% of children on a 10-day course of penicillin for streptococcal infections were no longer receiving the drug by day three. (The Merck Manual of Diagnosis and Therapy)
I guess I expect it with maintenance drugs, but this is for your sick kids where you have already purchased the medication.
Deloitte Survey Of Health Care Consumers II
I posted an entry about a month ago about the Deloitte study that was out about consumer segmentation. That was from reading their website.
After someone sent me the PDF on their study, I finally read it on my flight to San Francisco today. It is full of lots of interesting facts based on their web survey of just over 3,000 adults in September 2007. Here are a few additional things that I pulled out (click on the tables to expand their size).
78% of consumers express a preference for customizing their insurance product by selecting the benefits and features they value and, in doing so, increasing or decreasing the overall cost of their coverage (Figure 18). Only 22% prefer selecting from a few pre-packaged products with defined benefits and features.
Hall of Shame – Customer Service
On the positive side, there were no healthcare companies that “won” this “competition”. Winning being that you were rated as having poor customer service the highest percentage of times. (On the flipside, very few were included.) [full rankings here]
“We’ve seen a fall in customer service as we’ve gone into a recession,” said Richard D. Hanks, the president of Mindshare Technologies, a customer-service consulting company. “As the cost cutting occurs . . . they start to cut the wrong things.” (Article)
Not surprisingly, the people surveyed said that being knowledgeable, available, and friendly were very important. As we all know, the key attribute is knowledge and with the complexity of benefits, multiple systems that healthcare reps need to access, and turnover, this is a challenge.
It’s no wonder that everyone is trying to move people to self-service. In a related article, some of the benefits of self-service were clearly articulated:
“What better customer service is there than self-service?” ask the marketers. “It’s fast!” “It’s accurate!” “It’s convenient!” “It’s confidential!” (No more bystanders overhearing that triple-cheese, extra-mayo order.)
- People buy more. Customers spend 39% more per order at fast-food kiosks and are twice as likely to upsize than if a person takes their orders. (Machines are programmed to ask every time, and no one can overhear.) Customers also buy more at deli kiosks in supermarkets.
- More people buy. Good Web self-service allows for far more customers to be adequately served.
- People remain loyal. “You mean I’m going to have to upload all my data into a new bank? And learn a new system? No way.”
- People give the company high marks for customer service. Yes, funny but true. It’s hard to complain about a food order that you placed yourself, a transaction that you scripted or the way you pumped your own gas. When customer service is self-service, you have only yourself to blame.
Guest Post: Health Researchers Obtain Grants for Video Game Study
12 US research groups were awarded grants this week in order to conduct studies on how interactive video games affect players’ health. There has been a lot of press lately for Nintendo Wii and its many health benefits. It seems that the Wii isn’t the only gaming system to influence a person’s lifestyle choices where health is concerned. Of course, not all games are having a positive influence.
Grants totaling up to $200,000 were given to each research team, all of which are connected with a major US university. The generous donations come from Robert Wood Johnson Foundation (RWJF), a private foundation that is dedicated to improving the health of all Americans.
In regards to the grants, RWJF program officer Chinwe Onyekere stated:
We have been actively working in this area since 2004. Over this time, we have heard repeatedly that there is a need for stronger evidence that games can improve health and healthcare and support the growing realization that games can make a real difference in public healthcare in the United States.
Our vision is that in the coming years we will have a thriving marketplace of well designed, compelling interactive games that draw on this evidence base to become highly engaging and effective tools for improving the health and healthcare of Americans.
The 12 teams are currently working on projects that focus on different age groups and behaviors. Maine Medical Center, for example, was awarded a grant for its study, “Family-Based Exergaming with Dance Dance Revolution (DDR)”. The aforementioned game, DDR, is extremely popular with children and young adults. It involves moving on a small, portable dance floor while a video with instructions plays on the screen.
Research grants were dispersed by RWJF in order to study things like “the potential of physical activity video games to serve as innovative, cost-effective ways to help people recover motor skills after experiencing a stroke” or “health impacts of online mobile mini-games for people with type 2 diabetes.” Another group of 12 research grants will be awarded next year.
By-line: Heather Johnson is a regular commentator on the subject of CNA Classes Online. She welcomes your feedback and potential job inquiries at heatherjohnson2323 at gmail dot com.
American Cancer Society on YouTube
I think it’s interesting to see how the American Cancer Society is using YouTube to create a call to action both around the election, the uninsured, and other issues.
Our First Think Different Event
Today was our first Think Different event in Boston. This is a road show we are doing around our new positioning and how health care companies need to get outside the box to improve the effectiveness of their communications. It has four external speakers plus our CEO.
[Spoiler Alert: If you are attending an upcoming session, I may reveal some of the content here.]
I missed ½ the session today due to a client call, but I will be at 3 of the other 5 events. In listening to the first two speakers, I jotted down a few thoughts.
From Kinney Zalesne:
- She spoke about moving to the Starbucks economy and how we have much more choice today in what we do, who we love, religion, and our gender. Everyone immediately thinks of gender meaning sex change operations, but the point here is that there is a group of people who don’t want to be forced to select a gender identity. Before you discount it, you should know that 100 corporations, 75 colleges, and 8 states now ban discrimination based on gender identity. This was a bit of a surprise to me, but when I was talking with a large health plan about this, they informed me that their new EMR (electronic medical record) allowed for 5 possible gender options.
- She talked about people basically starving themselves to focus on the theory that has been demonstrated in animals, but not yet in humans which says that by eating 30% less calories you can extend your life by 40%. (Not something I will be doing.)
- She talked about the Do-It-Yourself (DIY) Doctors which are the people who use the Internet to self-diagnose and treat the MD as an ATM for drugs (i.e., I need a prescription for simvastatin can you please write it for me). I have heard a lot of talk recently about the changing perception of physicians. I haven’t seen the statistics, but one person said that they have lost the most respect over the past 20 years than any other profession. I think Kinney’s point is more about them moving from being a supervisor role (i.e., you should do this) to an advisor role (i.e., thanks for your opinion…I will take it into consideration).
- Her statistics about 5M working retired (i.e., >65 years old) and 2M working teens (i.e., using the Internet to make money before they leave high school) says a lot about how benefit design will need to change. The implications on needs and flexibility (e.g., imagine two primary addresses for snowbirds) could be significant.
-
In her talk about micro-targeting, my mind drifted to a few thoughts:
- How has gas prices changed our opinion of other costs? A $15 copay used to be equal to 7 gallons of gas. When it only equals 3 gallons of gas, do we view the $15 differently? [Have you caught yourself saying gas is only $3.75 at this one station near my house?]
- Just like your segmentation can change in healthcare, it is important to consider the macro-economic and political environment when communicating. Have you listened to all the car advertisements lately…they all talk about gas mileage?
- If you need a simple example of why personalization matters, think about buying a car. I am not a mechanical person so if I came in and someone talked to me about horsepower and cylinders then I would be turned off. I care about comfort and low maintenance.
- Finally, getting back to health, I thought about how difficult it is to be successful. Let’s assume there were 10 primary reasons for non-adherence and 3 primary channels for delivering information (live, letter, automated call). In this case, you have 10% chance of hitting the right message and a 33% chance of using the right channel (i.e., a 3% chance to be successful).
From Liz Boehm:
- She shared a lot of great facts about patient awareness of technology and how adherent they are.
- She points out a scary fact that while our health care needs are going up with the boomers we simultaneously have an issue with health care workers retiring which will only make things worse in the short term.
- She showed that 47% of people had visited their health plan’s website. [I will have to push her on this data since I believe they visited, but I think the percentage that log-in and use the site has to be very small. I would estimate 10-15%.]
- She talked about use of social media and gave an example of a MySpace group on diabetes.
- I found the discussion on wellness very interesting where she pointed out that things like chocolate, riding an elevator, or for some smoking gives you an immediate positive feeling while dropping your cholesterol by 10 points or even trying to lose 1 pound per week is pretty abstract.
- I have talked about loss aversion several times, and she talks a lot about it. Using it to make a link to why incentives matter in health care.
- Talking about motivation, I like her point that it isn’t a reasonable suggestion if you can’t achieve it. It may make good clinical sense to have a BMI of <25, but for someone with a BMI of 31, perhaps setting a goal of 28 is more reasonable and not as discouraging.
- In her talk about trust, it made me wonder how many people that work for managed care companies and pharmacy benefit management companies reveal that fact at cocktail parties. I am not talking about professional networking events, but your neighborhood events. Do you say who you work for and address their comments about service and/or coverage issues?
I finished my client meeting in time to hear Stan Nowak, our CEO and co-founder, speak and tie together the different points of view with some potential actions that people could take. As he often does, he talked a lot about the power of data and the fact that what’s new to health care is often old in other industries. We are an industry with the most data about people, but the least ability to use it effectively.
It’s also interesting to hear him talk about some of the “data exhaust” that is created by the analysis that the team does. These are facts that get revealed which may be surprising and may be things you never even thought to look for. For example:
- Patients with emphysema are 40% more likely to engage in a communications program related to additional coverage than patients with migraines.
- Patients with uncommon names are 18% more likely to complete a healthcare survey than those with common names.
- Males with depression are 83% less likely to do pill splitting than females with depression.
Skin Cancer Widget
 I get a lot of solicitations to talk about products on the blog. I also get a lot of general e-mails. The ones I generally respond to are people giving me a heads up about an article, press release, technology, or something else that I just wouldn’t have known about. That doesn’t mean I will do anything about it, but if I have time and find it interesting, I will usually click through the link. And, if it still catches my attention then I will write about it.
I get a lot of solicitations to talk about products on the blog. I also get a lot of general e-mails. The ones I generally respond to are people giving me a heads up about an article, press release, technology, or something else that I just wouldn’t have known about. That doesn’t mean I will do anything about it, but if I have time and find it interesting, I will usually click through the link. And, if it still catches my attention then I will write about it.
This one is fairly self-explanatory, but I found it interesting. VisualDxHealth has built a widget for you to self-diagnose your skin cancer. Which, according to the statistics they sent me, is valuable since 1 in 6 Americans will develop skin cancer and the survival rate is high when found and treated early.
The Recognizing Skin Cancer widget interactively provides information about the different types of skin cancer and includes a visual identification quiz that tests the user’s knowledge about recognizing the signs of these conditions.
Unfortunately, I can’t add widgets and other code to my blog or I would have lots of these types of cool things on the site.
Wii Fit: Using Technology To Teach Wellness
I talked about the Wii a few months ago when we first got one. At the time, I didn’t know that Wii Fit was coming.
This past weekend we happily bought it, and I enjoyed it. It tells you your BMI. You can do yoga. You can do aerobic exercise (running, hula hoop, step aerobics). You can do agility exercises (downhill skiing, tight rope walking). I was a little skeptical, but I have been fascinated by the Wii so far.
And, I loved the fact that my 6 year old could get into it. She loved that once you put in your height, and it calculates your weight that it changes your Mii (avatar) to reflect your likely dimensions. She spent lots of time on the yoga moves that I probably never could have gotten her to do in a traditional forum.
This creative use of technology gives me a lot of hope for how we can teach our youth, drive rehab programs, and impact people.
Now what I am looking for is when will we see a competition to lose the most weight only using the Wii for training.

Groups And Microsegments
When I was listening to Kinney Zalesne (Microtrends author) present this morning at our Think Different event, there were several things that crossed my mind:
- Which micro-trends am I part of?
- How much micro-targeting is too much?
- Will consumers self-identify into groups?
Without going back to the whole book, I can think of several micro-trends with which I associate:
- Marathoning
- Stay-at-home worker and extreme commuter
- 30-winker (don’t sleep a lot)
- DIY Doctor (research my own care)
- Pet Parent (pamper my dog)
- Video Game Grown-ups (enjoy playing Wii w/ and w/o my kids)
- Blogger
It has come up in the past two sessions where I have seen Kinney present. The question is how much is too much. Just because I know that you like cats, subscribe to Popular Mechanics and GQ, and have 3 siblings, should I use that information?
 I certainly think that more targeting is better although I might not always want you to tell me how much you know about me.
I certainly think that more targeting is better although I might not always want you to tell me how much you know about me.- You have to be flexible enough to allow for mistakes in interpretation and/or not too presumptuous. (For example, one of our co-founders is from Brazil but has been here for years. He recently started getting all of his communications from a few companies in Spanish. He didn’t opt-in, but they assumed his last name meant he spoke Spanish (which is not what they speak in Brazil BTW).)
- You have some issues of parity which must be either addressed or are legally required (i.e., you may have to treat everyone in a similar way). I am sure we might all like to drive high satisfaction for healthy members to increase their retention, but this deliberate adverse selection would be an issue and abuse of information.
Finally, there is a lot of discussion about capturing preferences (i.e., I prefer calls over letters) and how to segment populations. I think there is an interesting trend in social media for people to self-identify into groups. For example, I pulled up my LinkedIn profile to look for a second at all the groups to which I belong. The same thing is happening in Facebook. Until recently, this was not a huge driver of activity, but over the past 6 months, I have noticed people forming and joining groups. We want to be associated with certain things. I think if I knew how the information was being used that I would spend a few minutes during enrollment filling out information about how and when to communicate and interact with me. I think I would even reveal my Myers-Briggs category (INTJ) if it helped someone better deliver information to me that would make me healthier.
The younger generation is rapidly becoming used to revealing lots of information about themselves. I don’t think that things are considered as private as they once were.

 June 19, 2008
June 19, 2008