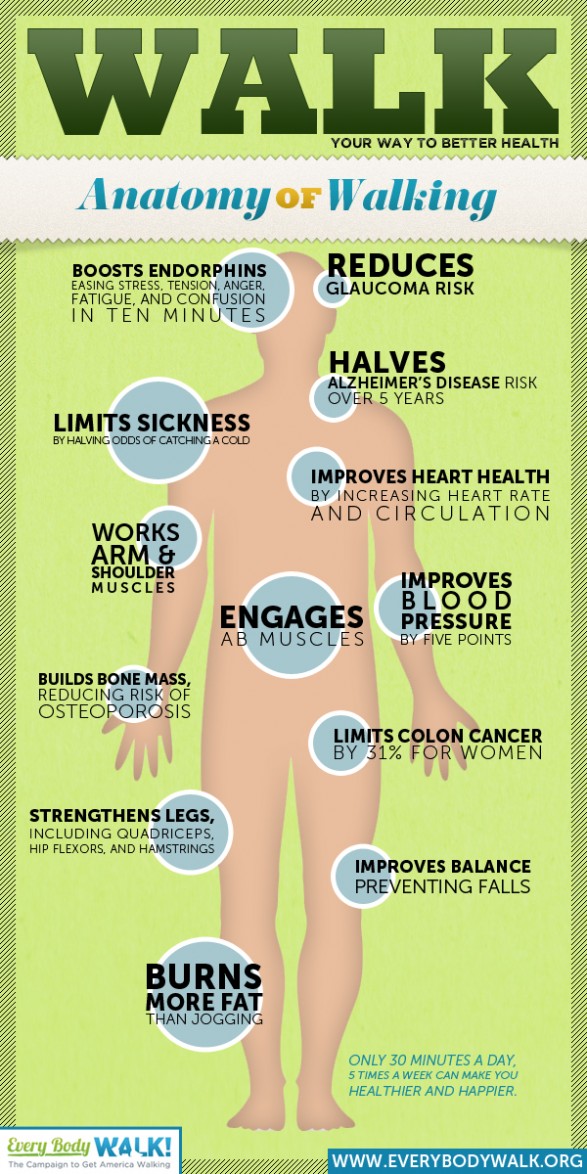
Some of you have probably seen some of the efforts by Kaiser to encourage walking. Here’s an infographic that they put out as part of their EverybodyWalk efforts.
Ambient Paper For Adherence
We’ve all heard of GlowCaps which is a great idea of using sound and color and communications to remind people to fill their medications.
One idea I’ve thought about for several years is the idea of “intelligent paper”. Imagine a refrigerator magnet or prescription label or some other piece of information printed on paper that changed color with time. As it got closer to time to refill your medication, it would turn yellow. When it was time to refill, it would turn red.
It should be easy. If you blend this with the QR code that Walgreens uses for refills, you have a captive reminder and reorder system that could be embedded within the label for less cost. I haven’t totally solved the issue, but it’s one that I think is feasible to accomplish and sell as a low-cost reminder vehicle.
Pharmacy Adherence (Waste) And The Need for MD-RPh Collaboration
I spent the day today at the NEHI adherence event in DC. I pulled out a few of my takeaways below, but while I was riding on the plane to get here, a few things were running thru my head:
- The focus on budget and the estimates that adherence costs us $290B a year here in the US. (or as one person pointed out that’s $1.2T in a presidential term)
- The recent report estimating that chronic conditions could cost us $47T worldwide over the 20 years which is leading to the UN talking about healthcare for only the second time ever.
- The discussion by George Paz from Express Scripts the other day about how PBMs drive value by eliminating waste (see Drug Trend Report). A large piece of waste is adherence and certainly one of the forecasted benefits of the combined Express Scipts and Medco entity is the intersection of Consumerology with the Therapeutic Resource Centers (TRCs).
- The ongoing dialogue around motivational interviewing, commercial MTM, and blending face to face interventions with technology to “nudge” behaviors.
- The huge opportunity which I believe exists in leveraging technologies like Surescripts to create data exchanges with physicians around MPR and barriers.
- The exciting fact that the new STAR measures for Medicare include more adherence metrics that are weighed more heavily than some of the operational metrics.
Fortunately, these were a lot of the topics that were discussed. Here some of the discussion topics:
- The fact that there’s no “easy button” for adherence.
- How adherence is a foundational building block for quality.
- The role of HIT in sharing data bi-directionally across the care team.
- Upcoming evidence around VBID.
- The role of the pharmacist and need for them to collaborate more with the physician to discuss and manage adherence.
- The fact that the adherence solution has to be multi-factorial.
- The need to optimize the drug regiment and individualize care (aka patient-centered care).
- The role of the caregiver.
- Opportunities around PCMH, readmissions, MTM, and eRx.
- The need for patient engagement.
- The need for the patient to believe in the therapy and that it will make them better.
- Good discussion on the role of the PCMH (patient-centered medical home) versus the pharmacy as the foundation for adherence.
- Discussion on whether physicians could address adherence if time wasn’t an issue. Do they have the training and skills?
- Social media as an emerging factor.
- Reaching the consumer when they have time and are receptive to information.
- Helping prepare the consumer for the encounter (i.e., checklist or list of questions).
- What happens when the patient waits in line and then is rushed themselves in the encounter.
- The role of technology in complementing the physician and patient.
- How to share data across team members.
- The need for ROI data on interventions.
- The value of having a Dx on the Rx.
- The need to vary incentives and not keep doing the same thing.
- If prevention is long-term and adherence is short-term, should the physician focus more on adherence and less on screening and other preventative measures.
- The need for – sufficient accountability, information, and skills.
- Adherence as a solution that needs to be localized.
- Patient centered or disease centered solutions.
- The governments role in improving adherence via policy and funding demonstration projects through CMS.
- STAR ratings and the bonus payments as an incentive to motivate research and programs in this area.
Overall, it was a good discussion with a very engaged panel and audience. We didn’t come to any answers, but you certainly got to think about the topic, identify some projects that should be done, and identify some research questions.
I look forward to pulling out a few of the topics in more depth. They align well with the communications platform and intervention strategies that Silverlink provides for our clients around adherence.
Flu Shots: Stock It And They Will Come?
This is the hot topic. Everyone wants you to get a flu shot because it’s good for your health and a profit making opportunity.
- The CDC recommends flu shots for everyone over 6 months of age.
- Pharmacies have big expectations about volume but “unfortunately” (from the perspective of nudging people to act) the disease does not seem to be too prevalent yet.
According to the CDC (and thanks to Larry Marsh’s team at Barclays Capital for sending out in their Flu Clues report):
We highlight that 0.8% of patient visits to physicians were due to flu-like illness, which is down 20bps from last week’s data. We note that this is well below the peak of 8.0% in early 2010. The 0.8% rate is below the national baseline average of 2.5%. Next we note that 6.0% of all reported deaths were due to pneumonia and the flu, 10 bps below last week, and below the epidemic threshold of 6.4% for week 37.
Traditionally, only about 40% of US adults will get a flu shot meaning there’s lots of opportunity for growth in vaccinations. Tim Martin from the WSJ has talked about this in a few recent articles – Flu Shots Are A tough Sell This Year and People Have Big Plans For Flu Shots. In the second article, he quotes a recent survey showing almost 2/3rds of adults plan to get the shot this year. BUT WHY? (other than the fact that those who respond to survey’s around flu shots may be more likely to take action)
You can also look at the Google flu trends data (again thanks to Larry Marsh and team for pointing this out) which shows online searches down for flu topics:
Like last year, the number of locations for getting a flu shot has expanded exponentially driven predominantly by pharmacies (which BTW is a good thing for them in demonstrating additional value). You’re even seeing some creative programs building on last year’s programs. One new one I’ve seen is Walgreens use of Foursquare for donating flu shots.
Of course, if we can’t convince healthcare workers to get flu shots then it’s going to be really hard to convince the average consumer.
I would expect MA plans to work with their PDP provider or pharmacy partner to drive members to get flu shots. Since flu shots are a STAR measure, it’s important for plans to reach out and get consumers to get a flu shot.
But why should I get a flu shot if my likelihood of getting the flu is down? That is the question.
That’s why I’m skeptical about some of the “generic” marketing efforts. I think everyone knows that they “should” get a flu shot and now finding a location for one is easy. BUT, we need to make it relevant to them especially those of us in healthcare. Ideally, their pharmacist and physician are talking to them about it, but if not, how do “we” (as healthcare companies) engage them.
We have to make the “pitch” relevant to them. For families, make them understand the importance of keeping the family healthy and their kids in school. For pregnant moms, help them understand that it’s important and why. For people who work, stress the importance of not missing work. For people with chronic conditions, focus on their additional risk. For the elderly, explain the risks to them.
A recent Walgreens study quantified some of the costs of the flu:
A new Walgreens survey examining the effects of influenza on people’s everyday lives and the economy, suggests that last flu season resulted in 100 million lost works days, along with nearly $7 billion in lost wages and 32 million missed school days, among many other findings released today. These findings, the first of a two-part Walgreens Flu Impact Report series, underscore the ramifications the flu and ill-timed illness can have beyond people’s health – from missed work and lost income to parenting challenges.
According to the Centers for Disease Control and Prevention (CDC), on average 13 percent of the U.S. population gets the flu every year, with active flu seasons seeing closer to 20 percent, or more than 62 million Americans.
New Walgreens Pharmacy Layout

I was in a Walgreens last week in Chicago. Maybe it’s just a newer store than my local store in St. Louis, but I thought the pharmacy looked very different. I captured a few shots with my camera phone. As you can see below:
1. There is an automated check-in option for refills. 
2. There is a pharmacist in front of the counter not just behind. (And people were actively coming in and talking with him.) The clinic also seemed to have a person on the floor roaving around interacting rather than sitting behind a podium. 
4. There was a sitting space with what appeared to be a meeting room.
5. Overall, there was a lot more signage and videos which made it a very lively and bright place to be. 
This seems like a different engagement strategy. I’m surprised no one is talking about it. The only thing I could find was a mention of a “training store” and 40 locations and the following mention in an article about Express Scripts and Walgreens:
As part of its plan to expand its healthcare offerings and reduce costs, Walgreen is working on pilot stores with new technology and a health guide on staff to help patrons more easily fill prescriptions, speak to pharmacists and see nurse practitioners at its in-store Take Care clinics. The first such store, in the village of Oak Park, Illinois, opened in November. Walgreen plans to have 20 stores in Chicago and other nearby towns by October. (source)
It sounds like there are just a few stores so I must have got lucky to stumble into this one. I had heard rumors of some re-design, but I hadn’t seen anything out there on the Internet. Interesting. I’d love to see a study to understand satisfaction, engagement rates, retention, etc. associated with this footprint versus the older store pharmacy layout.
Is Your Adherence Program Leveraging Segmentation?
I was just finalizing a new marketing piece with our marketing team on Silverlink’s adherence services. I love this picture because it drives home the point of understanding the consumer.
If you don’t understand the factors that drive behavior and leverage those attributes in segmentation and personalization of your adherence program, you may be leaving opportunities on the table.
Videos from Kim Feil, Walgreens CMO
I was looking for something else and stumbled upon a few videos in YouTube by Kim Feil who is the Chief Marketing Officer of Walgreens.
Primary Adherence – Technology, Kaiser Study, and EHRs
I think we all know that primary adherence is a real issue. Depending on what you read, you see that anywhere from 20-30% (or more) of patients don’t start therapy. They are prescribed a drug, but they never fill it. This is due to lots of reasons:
- They get a sample.
- The drug costs too much leading to abandonment.
- They don’t feel like they need the prescription.
- They feel better.
- The doctor tells them only to fill it if something else doesn’t work.
These issues vary based on whether it’s an acute drug or a maintenance drug. It also varys by drug class.
I’ve always been surprised that pharmaceutical manufacturers focus so much on ongoing refills leading to improved MPR rather than focusing on primary adherence which would grow their market significantly. One of the big reasons for this has been visibility. Without electronic prescriptions and mapping those to claims data, it was hard to identify who had a prescription and didn’t fill it. You could do something with data out of the PPMS (Physician Practice Management System) or through more complicated processes to get data out of their notes, but it wasn’t easy.
So, this new study by Kaiser caught my attention.
If you are a diabetic, have high cholesterol, or high blood pressure and you receive medical care at an integrated healthcare system that has electronic health records (EHRs) linked to its own pharmacy, then you are more likely to collect your new prescriptions than people who receive care in a non-integrated system, a Kaiser Permanente study shows.
That’s a strong sell for an integrated model, but perhaps more realistically for the use of EHRs. You can also see some of the data from Surescripts around this topic of electronic prescriptions and adherence.
This creates a great opportunity for pharmacies, PBMs, payers, and pharmaceutical manufacturers to leverage technology to improve primary adherence. By identifying people who don’t fill a prescription they receive, companies can help determine which of those are intentional and which of those should be addressed. This should help address the overall costs attributed to non-adherence and be a business driver for all these entities.
[Note: If you’re interested in working on primary adherence, let me know. We have several approaches for this at Silverlink.]
Walgreens and Express Scripts: The Plot Thickens ($ESRX, $WAG)
Remember when this “conflict” was first announced a few months ago. If you’re like me, you probably assumed this would be over in 30-days like the Walgreens – CVS Caremark dispute last year. What’s different? I’m not sure. It seems like both sides are well dug in. (From my poll a few days ago of 22 of the readers of this blog, 65% felt this would get resolved by 1/1 and 25% felt that it would never get resolved.)
Now, it seems like both sides are continuing to take significant steps towards no resolution.
Express Scripts has apparently launched a pilot program to move share from Walgreens stores now using coupons. I believe the pilot was with Lowes and is about to expand to the Department of Defense. Additionally, I’ve heard that Express Scripts has sent out letters to their clients preparing them for a limited network starting 1/1/12 without Walgreens.
On the flipside, I’ve heard that Walgreens has begun putting signage out encouraging consumers to talk to their plans about excluding them from the network and for Medicare members to chose plans that aren’t run by Express Scripts. Walgreens also put out a whitepaper about what happens when you remove them from the network. This has some really interesting data in it.
Key Statement: Excluding Walgreens from a pharmacy network will result in little to no savings for most sponsors and patients, and in some cases will raise costs, while causing significant patient disruption and risking gaps in care, and increasing administrative costs on plan sponsors.
- As part of this document, they are encouraging payers to consider directly contracting with them and/or creating a custom network (if their PBM contracts allow for that).
- They state that their costs are comparable to other retailers or within 2% of their costs.
- They show some data from another PBM (not named) that modeled out network savings for them based on a limited network taking into account their drug costs, generic fill rate, and 90-day rates. It shows a jump in costs versus savings.
- They share data that their Generic Fill Rate (GFR) is 1.4% higher than the rest of the Express Scripts retail network which the paper says translates to $2 per Rx in cost.
- They say that 90-day retail generates a 6-8% savings compared to 30-day retail based on the pricing that they offered to Express Scripts.
Ultimately, I still believe resolution will occur before the end of the year. While both parties are dug in, I believe it’s a lose-lose situation for this to stay unresolved. That being said, there are lots of things that could occur here:
- This creates a wave of direct contracting between payers and pharmacies.
- This validates the integrated model of CVS and Caremark.
- This creates a large number of limited networks.
- This creates greater use of the Walgreens discount card and/or cash business at Walgreens especially for lower cost generics.
- Alienating Walgreens creates a disruptive force in the FTC review of the proposed Medco acquisition.
- Another PBM jumps in to do a creative deal with Walgreens which limits their long-term ability to work with Express Scripts.
- Express Scripts ends up in a shotgun relationship with CVS.
- The terms of PBM contracts get changed going forward based on new terms regarding retailers.
- Walgreens becomes a much more vocal voice in the retail world through NCPA and other organizations.
Between this and the proposed Express Scripts acquisition of Medco, the landscape in the PBM market could be radically different by early 2012.
[Note: As the stock market has dropped, I have continued to buy stock in the PBM industry including several of the specific companies mentioned in this post – MHS, ESRX, WAG and CVS.]
$47 Per Rx Guarantee From Prime Therapeutics
I think this is a good, bold move. Prime Therapeutics has launched four new programs. The most aggressive is called Reliance and guarantees your net spend per Rx at $47. The easy way to do this would be to exclude specialty drugs and basically offer a generics-only formulary. My quick read from their drug trend report and press release is that it includes specialty drugs. It also includes a lot of utilization management programs, suggestions on plan design, encouragement for mail order, and other features. I’ll be interested to see the adoption of the program or whether it’s just a great program to encourage clients to consider new, more aggressive plan designs.
“Our Reliance plan keeps costs predictable for plan sponsors,” said Michael Showalter, Prime Chief Marketing Officer. “The goal is to make pharmacy benefits easy, understandable and affordable. Through Reliance, there will be no surprises, allowing organizations to better plan for and manage their pharmacy costs and reduce overall health care costs, while providing excellent benefits. We provide a single number demonstrating the true cost of care – $47. We are the only PBM to back that up with a price guarantee and complete price transparency.”
Infographic: Hazards of Hospitals
Scary infographic from http://www.MedicalBillingandcodingCertification.net.
Highlights From the Prime Therapeutics 2010 Drug Trend Report
I just finished reading the Prime Therapeutics Drug Trend Report. As I highlighted the other day, their overall drug trend was 2.9%. Like in the past few years, they have jumped up to offer a report comparable with the other big PBMs. And, as we saw with last year’s report, the new management team is aggressive in using this to highlight research, their competitive differentiation, and point out why they are a competitive force in the market.
More interesting that just their success in drug trend was their “adjusted drug trend” for the other PBMs. You don’t often see this in your face marketing in this space, but they clearly want to show not only that their trend was better but that their methodology is better. (I don’t have the time to compare methodologies at this point.)
Fortunately, they don’t stake the argument on trend since as I’ve pointed out before – trend can be misleading. Sometimes higher trend is good as when it indicates better Medication Possession Ratio or better success at reducing gaps-in-care. They focus on five things in the document:
- Savings
- Safety
- Guidance
- Satisfaction
- Partnership
Their Generic Fill Rate (GFR) for 2010 was 69.2% which was lower than the 71% reported by Medco and the 71.5% reported by CVS Caremark. (I couldn’t find the Express Scripts numbers for whatever reason.)
The report focuses on some of the differences in the Prime model (client ownership, not public) and how that plays out in transparency and alignment.
They are now at 12 Rxs PMPY which to me still seems a little low. (I’ve mentioned this is prior reviews, but I don’t understand why their population usage is different.) To validate my hypothesis, I looked at the PBMI report from last year which shows PMPM utilization ranges by respondents (not industry averages).
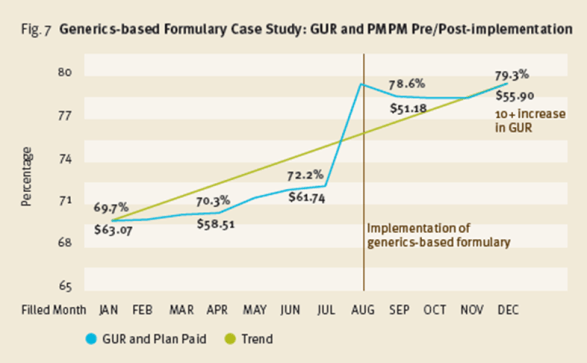
I do think their example around implementing a generics-formulary along with their new benefit plan guaranteeing cost at $47 per Rx are very interesting. They remind me of the GenericsWork product I launched at Express Scripts and should offer some clients a great way to save money. They key, as I learned, was really understanding how to manage member disruption and gain buy-in to the offering. [Amazingly, a quick Google search led me to a cached image of the PDF from my product from 2004.]
They give some good MTM numbers:
- $1.29 in return for every $1 spent
- $86 in savings to the payer over a 10 year period per MTM encounter
They also announce a new offering for 2012 which they call the GuidedHealth care engine. There’s a little information in the document, but it sounds intriguing.
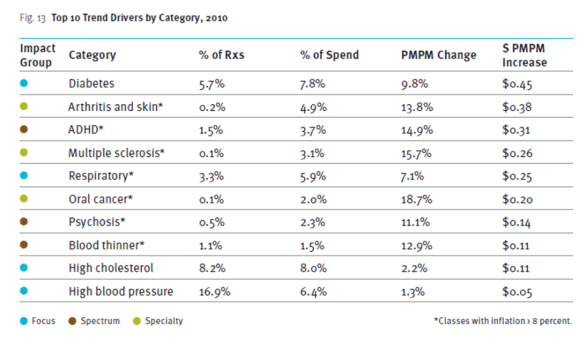
One of those typical charts that we all like to look at shows the drug classes that contributed most to driving trend.
I think their equation about overall cost…
Optimal cost = (medical cost + pharmacy cost) x health outcomes
One of my favorite charts is below which recognizes that there are two cost curves to focus on. The one for the relatively healthy which is often highly pharmacy focused cost versus the chronically ill that drive the majority of overall costs and is heavily medical and specialty medications.
Another study they share in here looks at the likelihood of hospitalization tied to adherence. Very interesting.
$7.60 PMPY savings for a limited network. Those are big numbers that they share from a case study around a client limiting their retail network by excluding one chain.
Their drug trend report looks at another hot topic – 90-day prescriptions. They share their results of a statin study looking at waste in 90-day retail and mail and 30-day retail and estimate the cost impact of the waste.
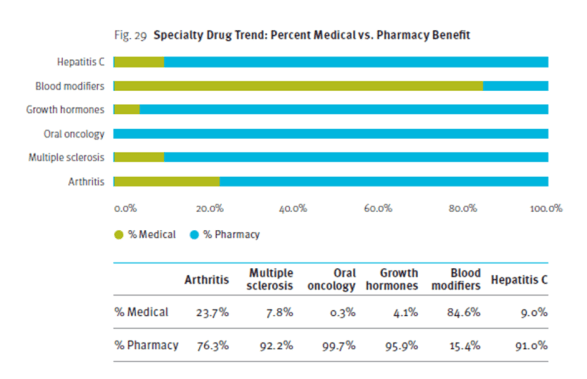
Another hot topic is the mix of specialty drug spend between medical and pharmacy. They share a chart looking at several of the large specialty drug classes.
At the end of the report, they give suggestions to clients on a spectrum of management (low to high). They also predict a few things in the next five years:
- A return to double digit trend increases after this generic wave;
- A generic fill rate in excess of 90%;
- Specialty drugs accounting for 40% of spend;
- Healthcare spending will increase 8-10% per year;
- The role of genetic testing will be validated; and
- Up to 25% of employers will drop benefit coverage.
Summary Of Drug Trends (Prime’s Report’s Out)
Prime Therapeutics published their Drug Trend Report yesterday. I haven’t had time to read it yet, but I pulled their total trend numbers and aggregated them into charts with the previously reported numbers from other PBMs. (As always, you can see detailed summary’s from Adam Fein and I on most of the reports.)
Additionally, here’s a summary from last year. AND, as always, don’t forget that these aren’t apples to apples.
(NOTE: Lower trend is better implying that the PBM is doing a better job at managing costs for their clients although as I’ve argued there may be some clinical reasons for trend going up that are good – e.g., improved adherence, identification of pre-diabetics, addressing primary adherence.)
Increasing Preferred Pharmacy Usage (3 of 3)
- Driving preferred pharmacy usage from the employer site
- Using social media
- Borrowing from other industries
The idea in all of these was to look at new ways that builds on the standard approach that we work with many clients on today. And, if you believe that the Express Scripts / Walgreens dispute won’t get resolved, we’re going to see a lot of people using limited or preferred networks very soon. This is also something that Adam Fein talked about in highlighting some of the progress Wal-Mart is making in this area.
So what are some examples of things we could borrow from other industries?
Referral Program: Why not offer incentives for people who refer their friends and family into the pharmacy? Wouldn’t this play into the social network or peer-to-peer trends out there?
Satisfaction Surveys: Why isn’t there more monitoring of the customer satisfaction to look for improvement opportunities? [Note: I know there is some, but I think it’s under-utilized as a tool.]
Tiered Service Levels: Frequent travelers get different levels of customer service. Why don’t high utilizers with lots of co-morbidities and Rxs get a better level of service?
Points: Why aren’t there more incentive systems and “points” that are used to reward consumers based on share-of-wallet or other metrics? [I think there may be some legal issues here.]
Online Order Tracking: Why can’t I watch my prescription being filled and track it around the system online?
Pharmacy Ratings: Why isn’t there a consumer and business system that ranks pharmacies based on wait time, friendliness of staff, error rates, generic fill rates, overall satisfaction, or other metrics that can then be pushed to the consumers?
Incentives / Coupons: Certainly these have been tried and there are limits here especially in government funded benefits, but it’s still few and far between.
MD Programs: Physicians can certainly influence this decision. Why isn’t there more effort to differentiate a pharmacy (mail, retail, specialty) by building relationships with high prescribers?
Check-in / Preferences: Why don’t the forms in the physician’s office (or applications) have you select a preferred pharmacy or have a pop-up with a preferred pharmacy in it to drive you there?
Credit: For some people, it’s an issue to front the money for the 90-day supply. Why haven’t the mail order pharmacies partnered with a credit card company to allow for installment payment?
If you’re going to “win” at this game, you have to think differently. You have to test and learn. You have to capture insights from your customers and translate them into product offerings. It’s not easy.
Infographic: MD-Pt Communication Link To Non-Adherence
Within the payer / pharmacy / PBM world, we tend to think of adherence as something that can be addressed by us. What if the problem is more systemic than that? I’m not talking about clinical issues like side effects or even cultural biases.
I’m talking about process related issues that stem from physician and patient interactions. If the patient doesn’t believe the drug will help them and doesn’t understand their condition and their medication, they’re set up to fail.
With that in mind, I appreciated the infographic that Stephen Wilkins (@HealthyMessaging) sent to me earlier today (see below):
Increasing Preferred Pharmacy Usage (1 of 3)
For my purposes, I’m going to define a preferred pharmacy as one of the following:
- Mail order pharmacy
- 90-day network (e.g., Maintenance Choice, Walgreens90)
- Limited or tiered retail network (e.g., Align, Walmart, Caterpillar, Humana/Walmart)
- Specialty pharmacy
- Specialty pharmacy with exclusive distribution of a drug
- Driving preferred pharmacy usage from the employer site
- Using social media
- Borrowing from other industries
- Plan design
- Incentives
- Interventions (letters, calls)
- Reminders on the intranet
- On-site collection boxes
- Kiosks
- On-site pharmacy
- Show them a message about considering mail order
- Trigger an SMS asking someone to call them
- Send an e-mail requesting a call back about the closest preferred pharmacy
- Send them a map of the closest in-network pharmacy
- Link them to a YouTube video on getting started with mail order
- Or, in the Worker’s Compensation area, it could create a virtual card for the network
25% of MDs Tell Un-vaccinated Kids To “Get Lost”
Unfortunately, the issue of kids not getting vaccinated is not going away. While only 1% of infants don’t get any vaccines, there are still 30% of kids who don’t get all the recommended vaccines.
So, what should a pediatrician do about families that don’t get their vaccines? Should they continue to treat them? The number that say it’s time to find a new provider has jumped to 25% in 2011 (compared to 18% in 2005) according to research reported in a Time Magazine article. I’d bet that number might jump further as physicians bear risk or have more money tied up in performance bonuses.
It begs the question of what adults do…For example, with flu shots, do adults get them? Based on a Consumer Reports study, it’s only about 50% of adults that do.
I have a few older posts on this general topic. It’s also a very interesting topic in the pharmacy world as retailers focus on vaccinations both as a revenue source and a value-added service.
- Penn and Teller on Vaccinations
- 50,000 Adults Die Each Year Of Vaccine Preventable Diseases
- Vaccines and Autism…The Long Path Back
- Increasing Flu Shots
I also found this infographic on the topic which I thought I would share.

Created by: Medical Coding Career Guide
Engaging The Un-Engaged
One of the hot topics in a lot of healthcare conversations these days is engagement. There’s the “easy” engagement for the e-patients that are actively involved in their healthcare. Then there’s the much harder engagement of those that aren’t engaged. And, finally, there’s the issue of chronic engagement. I can easily get someone to engage a few times with an incentive or some other “trick”, but how do I get them to stay engaged over time. It’s not easy.
This is one of the topics that will be discussed at the upcoming Forum 11 in San Francisco. If you’re coming, look me up. I’m presenting on Friday.
How To Use A Robot For Patient Support
While it’s unlikely that we’re going to get much empathy from robots in the near future, VGo Communications is definitely making the idea of tele-presence more believable. What intrigued me when I first saw this was the ability for remote caregivers to participate in events. For example, I could imagine my parents going to a physician’s visit in Detroit. If I was able to log-in and join them using a VGo robot, it would be great. It’s unlikely I would fly from St. Louis to Detroit to join them.
Now, cost would be an issue here, but I’m guessing someone can come up with a model that allows providers or hospitals to buy multiple robots and allow a remote, web-based log-in process. (After some training by the user on controlling the robot.)
If we look at studies like the one presented by Kaiser years ago (see below), we know that there’s a huge gap between what the physician says and should say. For example, this shows that only 34% of the time did the physician tell the patient the duration of therapy. This play into what I’ve talked about before which is the gap between what the physician says and the patient hears and the questions that come up after the fact versus what questions come to mind during the office encounter. Could a tele-presence by a third-party help that? It’s an interesting concept.
Great Video! Placebo Effect Summarized In Video
A great summary of lots of the placebo research. A must watch. (remember if you get this e-mailed to you that you might have to come to the website to see it.)
Diabetes Around The World (Infographic)
Here’s an infographic from ActosInjuryLawyers.
Penn And Teller On Vaccinations
This is a video that everyone should share. It’s a funny, short, and blunt video on why to get your kid vaccinated.
There was a recent article in USA Today about vaccines which said:
Vaccines are widely available across the country, doctors say, and poor children can get them for free. The biggest impediment to vaccinating kids today is not cost, but fear, says William Schaffner, a spokesman for the Infectious Disease Society of America and professor at Vanderbilt University School of Medicine in Nashville. Around the world, millions of parents began skipping or delaying vaccines because of an infamous (and since retracted) 1998 study in the British medical journal The Lancet. The study’s author theorized that a combined measles-mumps-rubella shot caused autism.
It became one of the greatest myths in modern medicine, says Offit, author of Deadly Choices: How the Anti-Vaccine Movement Threatens Us All. He points to nearly two dozen studies showing no link between vaccines and autism. Last year, The Lancet issued the retraction after learning that information had been falsified. British health officials also stripped the study’s author of his ability to practice medicine in England because of professional misconduct.
Press Hits, Presentations, Writing YTD
I wanted to put together a quick summary of brand awareness so far in 2011. It’s been a banner year already exceeding 2010 press hits (21).
- Drug Benefit News article in January around predictions for the industry
- Whitepaper on the future of the PBM/pharmacy industry
- Mention of my whitepaper in Adam Fein’s blog
- Barclays PBM Expert Call on 2/8/11
- Drug Benefit News article on Lipitor in February
- Managed Care Magazine on Lipitor
- Drug Benefit News article on coalition in February
- Drug Benefit News article on Walgreens PBM sale in March
- AIS Webinar on Copay Cards
- Drug Benefit News on Copay Cards
- Pharmacy Times on Mail Order
- Silverlink eBook we put out on healthcare communications
- AJPB July/August 2011 From the Editor
- Health Plan Weekly (8/1/11) on OptumRx moving away from Medco
- Pharmacy Technology Podcast in July
- Ten different appearances in the PCMA SmartBrief
- Five references on RxRoundtable.org
- A blog citation about extreme couponing
- Some discussion of my AIS webinar by David Williams
- A guest post on KevinMD about paying physicians for adherence
- Grand Rounds
- Drug Channels News Roundup
- A mention in DigiPharm
- HealthLeaders on Medco sale to Express Scripts
- HR Online about limited networks
- Drug Channels review of the Express Scripts Drug Trend Report
And, I have 5 things that I’ve actively provided comment and content to including my upcoming presentation at the Care Continuum Alliance on engaging the hard to engage with one of our clients – Aetna.
Yellow Dot and HIPAA
I’m confused. We spend so much time and money in this country worried about HIPAA and patient privacy and now people are putting all their healthcare data on a piece of paper in their glovebox and putting a sticker on their car letting people know that it’s there. The program is called Yellow Dot. (see USA Today article)
Don’t get me wrong…I think it’s a great, low-cost strategy to give data to rescue workers in an emergency. (Not that there shouldn’t be a much easier strategy using technology.) I’m just amazed that no one seems to worry about privacy here. Maybe, privacy is only an issue when data can be stolen in mass quantities and sold not when someone can break into your car at the grocery store and take all your information.
Am I alone on this or do others find these things difficult to reconcile?
Storytelling Is A Part of P2P Healthcare
P2P (or peer-to-peer) is a popular topic in healthcare today. It builds on both the social components of behavioral modification along with the social networking trends.
About one-third of Americans who go online to research their health currently use social networks to find fellow patients and discuss their conditions, and 36 percent of social network users evaluate and leverage other consumers’ knowledge before making health care decisions. Social networks hold considerable potential value for health care organizations because they can be used to reach stakeholders, aggregate information and leverage collaboration. (from Deloitte study)
One of the biggest researchers out there in this space is Susannah Fox from the Pew Research Center.
Peer-to-peer healthcare acknowledges that patients and caregivers know things — about themselves, about each other, about treatments — and they want to share what they know to help other people. Technology helps to surface and organize that knowledge to make it useful for as many people as possible. (from recent presentation from NIH – “Medicine: Mind the Gap”)
With that in mind, I found this study from a few months ago about storytelling very interesting. Imagine the power of capturing stories in some form – DVD, YouTube, written – and sharing them with newly diagnosed patients across an expanded social network. Imagine helping patients plug into a social network (ala – PatientsLikeMe).
Conclusion: The storytelling intervention produced substantial and significant improvements in blood pressure for patients with baseline uncontrolled hypertension.
What has really surprised me is that I haven’t seen the large institutional healthcare organizations promoting the use of the social networks. Maybe I’ve missed it, but I would think they would partner up with a few of these to encourage consumers to use them. I understand on the one hand that that is “handing off” a patient to a different company, but rather than trying to build their own social networking application, I think they’re better served to leverage what exists.
Newly Diagnosed Diabetics
I was giving a presentation today on diabetes and used this quote from the American Diabetes Association. I thought I would share it. To me, this is why it’s so important for pharmacies, PBMs, MDs, payers, employers, etc. to focus on the consumer experience and help address what consumers are feeling when they’re newly diagnosed with diabetes, cancer, or some other condition.
A New Life For Lipitor – OTC?
Are you surprised that Pfizer might have found a way to extend Lipitor? You shouldn’t be.
As I talked about before, Lipitor is scheduled to go generic later this year. Now, there are stories that Pfizer may try to take Lipitor over-the-counter (OTC). As Ed Silverman (Pharmalot) points out, this has been tried before with Mevacor. Has anything really changed since then? I don’t know much about any outcomes from the UK’s allowance of Mevacor to be sold BTC (behind-the-counter), but it would be a good point of information.
The prior questions about consumer behavior with an OTC statin all still apply:
- Will the right people use them?
- Will there be over-use?
- Will this create unnecessary risks?
- Will people monitor themselves appropriately?
Since statins certainly have side effects, this is a real question.
IMHO – I would think an OTC strategy is a low likelihood unless there is some new data.
On the other hand, with home monitoring of cholesterol tests, there have been some changes. This might be another source of data. Who’s using these? Have they impacted their use of medication?
Should You Be Fair Or Powerful In Your Communications
I’ve always found the discussion of why people with certain characteristics are more likely to get ahead very interesting. This recent article from Harvard Business Review talks about the fact that managers see respect and power as mutually exclusive. I think most of us would agree that this is unfortunate from a leadership perspective.
So the question I would ask is whether consumers think the same thing in terms of physicians, pharmacists, and their health plans. Are those that are respectful of the consumer seen as less powerful and therefore less likely to get their patients to be be compliant?
On the flipside, would consumers tolerate direct sometimes abrasive messaging that was clear with them about the risks?
May Video On PBM Selling Season (CVS, ESRX, MHS)
I just came across this video from May of Lisa Gill from JP Morgan talking about the 2011 PBM selling season. My couple of takeaways were pretty basic:
- Price is not the #1 decision factor in choosing a PBM. (I don’t believe that no matter how many surveys there are.)
- The model is creating differentiation. People like consumerology or the Medco clinical programs or the CVS Caremark 90-day program (Maintenance Choice).
I liked her quote from Florida relative to the CALPers issue at Medco that if they didn’t deal with people under investigation then there wouldn’t be anyone to do business with. (A little jaded perhaps!)
The key question here is the success that the smaller PBMs have been having especially SXC and Catalyst, but even more interesting would be her take on what will happen as Prime and OptumRx focus more outside of their traditional payer markets.
Everyone always talks about the 9x% of companies that don’t move PBMs, but the question really should be about lives that move. It only takes a few big clients – Walmart, GE, BCBS, … to make a difference in a selling season.
http://www.corporateresearchgroup.com/video-details.cfm?ID=263

 September 30, 2011
September 30, 2011