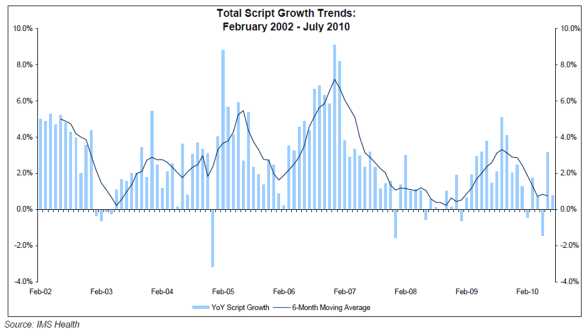
If you don’t visit, it’s worth going to the Kaiser Family Foundation Fast Facts section every once in a while. They take the research data and put it in slides that you can download. I did that and saved it up on Slideshare (see below)…
Predicting Non-Adherence
There is lots of buzz over yesterday’s article in the WSJ about Express Scripts being able to predict who will be adherent. Today’s blog post on the Corporate Research Blog added some details (or further confused me). It says that the model is 80% accurate in predicting the 10% of people who are least likely to be adherent.
Is that all it does? For sake of this post, let’s assume it does. That seems much less interesting and much easier to do. In talking with a leading researcher in this area that has looked at the correlation of 9,000 variables to adherence, he told me that nothing was highly correlated, but the most correlated metric was past behavior. Where they adherent in the past on other medications? Did they take preventative action (e.g., get flu shots, mammograms)?
Several people have been looking at how credit scores can be used to predict adherence. Given errors in credit scores, this may be deceptive even if it works.
But, back to the issue. If you know who’s least likely to be adherent, so what? Do you give up on these people? They aren’t likely to chance behavior. Do you try harder or have a different strategy with these people? If you succeed and move them to taking their medications 40% of the time (using a proxy like a 40% medication possession ratio), does it make a difference?
I would think it’s better to focus on the people who are likely to be adherent and how to enable them to move from 40-70% MPR to >80% MPR. We often work with clients to stratify their population and have different intervention strategies (channel, messaging, level of effort, etc.) across where they fit in the model (value, likelihood to engage, likelihood to change).
Stop By The Silverlink Booth At The Forum 2010 (DMAA)
Next week in DC is The Forum 2010 which is the annual event for The Care Continuum Alliance (formerly known as The Disease Management Association of America). If you’re there, you should stop by the Silverlink booth and attend the presentations that we’re giving with some of our clients and other industry leaders.
| Aligning Employee, Employer & Provider Research to Maximize Value-Based Benefits October 13, 1:00 – 2:00 p.m. Jan Berger, MD, MJ, Chief Medical Officer, Silverlink Communications Cheryl Larson, Vice President, Midwest Business Group on Health (MGBH) |
|
| Improving Statin Adherence through Interactive Voice Technology & Barrier-Breaking Communications October 13, 2:15 – 3:15 p.m. Ananda Nimalasuriya, MD, Chief of Endocrinology & Complete Care, Kaiser Riverside George Van Antwerp, MBA, General Manager, Pharmacy Solutions, Silverlink Communications |
|
| Addressing Colorectal Screening Disparities in Ethnic Populations October 14, 12:30 – 1:30 p.m. R. Reid Kiser, MS, National Director, Clinical Excellence Special Projects and Reporting, UnitedHealthcare Jack Newsom, MBA, MS, ScD, Vice President, Analytics, Silverlink Communications |
|
| Addressing an Epidemic – Improving Diabetes Care with Personalized Communications October 14, 3:00 – 4:00 p.m. Jan Berger, MD, MJ, Chief Medical Officer, Silverlink Communications William Shrank, MD, MSHS, Instructor, Harvard Medical School and Associate Physician, Division of Pharmacoepidemiology and Pharmacoeconomics, Brigham and Women’s Hospital |
Drinking, Breast Cancer, Heart Disease, and Donations
Another story I’m taking from USA Today. It was interesting. First, they talked in one article about a few alcohol companies that are promoting “pink drinks” as ways to support raising money for breast cancer. The companies didn’t appear to be linking sales to donations, but since drinking increases the risk of breast cancer, it raised an interesting question. Is that okay?
Would you buy chewing tobacco if they gave 10% of the purchase to fighting mouth cancer? Or would you buy more cigarettes from a company that had a lung cancer logo on the outside of the package and an advertising campaign around finding a cure for lung cancer? Maybe that’s not apples to apples. Would you buy more McDonalds (over Burger King) if they were more active in fighting childhood obesity?
Now, the breast cancer issue gets more interesting when they point out the health challenge of thinking about two sets of data…
- Drinking increases the risk of breast cancer
- Drinking reduces the risk of coronary heart disease
I think this is an interesting microcosm of what consumers face everyday. Confusing information from multiple sources leading them to not know what to do. Who do I trust? What action do I take? How do I weigh the tradeoffs? (Read the USA Today article for more or look at the blogger they feature at www.breastcancersisterhood.com.)
Americans Walk Less Than Others (Surprise!)
Really…this can’t be new news. BUT, it is relevant to our obesity epidemic. Here’s a chart based on a new study from the October issue of Medicine and Science in Sports and Exercise (also in today’s USA Today).
My takeaway…I need to use my pedometer and figure out how much I walk per day. It should be 10,000 or more steps a day to be considered “active”. [2,000 steps is a mile.]
I was surprised to see that women take more than 400 steps per day fewer than men in the US.
Aligning Images With Message
This new study says that just holding an alcoholic beverage makes you seems stupid. While I would agree that if your Facebook picture or blog picture was you with an alcholic beverage, I might think twice, but I’m not sure I would have the same impression of a person at a reception with a glass of wine.
But, it made me think about how important it is to think about images as aligning with messaging and branding. This is important in direct mail and e-mail and on the Internet. Being in the communication business, we often bring in mis-aligned marketing pieces to share with each other. (Maybe there needs to be a bad marketing blog like the bad pitch blog.) I remember one from a few months ago which was a happy birthday postcard to someone on turning 40 and encouraging them to take some action. The image on the postcard was of a 70+ year old woman. It really made the woman turning 40 feel like it was older than it is.
In another case, I think about when I was an architect. We were designing a boardroom for a big Fortune 100 company. When we were creating a rendering for presentation, I was told that the CEO didn’t like to see women in the pictures (probably wouldn’t happen these days) so we could only add images of men in business suits to the pictures.
White Coat Adherence
Do you brush your teeth more before you go to the dentist?
Are you more likely to take your medications the week before you go back for your physician visit?
YES!
But, do we make that clear to the physician? No. When the physician asks if you’re taking your medications, the answer is yes. That’s not a lie. What they need to know is how many pills are left since you last filled your medication? How many pills did you start with? How many did you lose?…
You get the picture. I like the term here that our Chief Medical Officer used – “white coat adherence”.
Now, let’s imagine that the physician orders a blood test for your cholesterol and your LDL hasn’t dropped, there are three scenarios:
1. They go back and really push you on your adherence (or diet and exercise);
2. They believe you but they assume the medication dose isn’t strong enough and increase your dose; or
3. They believe you but they assume the medication isn’t working and change your medication.
These are minimally issues for the healthcare system – wasted costs – but there is also the potential for giving you an unnecessarily high dose or changing you to a riskier medication since the default one didn’t work.
How do we address this? It’s not easy. This involves a few things:
1. Improving physician access to data (i.e., adherence data);
2. Improving physician – patient communications; and
3. Helping patients stay adherent and understand the impact of their medication (and lifestyle decisions) on their health.
I continue to see more and more data on the physician patient gap in communications. This is from a few years ago, but a study showed that 40 to 60% of patients could not correctly report medication expectations 10 to 80 minutes after physicians provided information, AND more than 60% of patients misunderstood prescription directions immediately after doctor visits. (source)
Pretty scary!
Auto-Renewal / Auto-Refill Article In Drug Benefit News
Per my prior two posts on this, Drug Benefit News (DBN) published an article today on this topic. Renee talked with me along with several other people to get a perspective on the topic.
Here are a few quotes from the article:
“Auto-refill for prescriptions is all the focus lately,” says George Van Antwerp, General Manager of Pharmacy at Silverlink Communications. “Everyone from the big PBMs to the local pharmacies are encouraging this.” This is because auto-refill programs address one of the common patient-reported issues with adherence — forgetfulness — allowing insurers to “minimize gaps in care.” Auto-renewals, on the other hand, are not considered common practice and many payers are hesitant to implement the service.
Express Scripts, Inc. is one of the few PBMs developing an auto-renewal program, which it will offer through home delivery. “Renewals are much more problematic than refills for patients when procrastination occurs,” Bob Nease, Ph.D., chief scientist at Express Scripts, tells DBN. “If you procrastinate on getting a renewal, it’s not just a matter of calling the pharmacy. You have to get a new prescription with a physician. And if you talk to physicians, they pull their hair out over this issue.”
Others contend that auto-refill and renewal programs may up plan costs by increasing medication waste. The concern is that auto-renewals may result in “provisions of medications that may not be a current active medication therapy or where the patient may have experienced an adverse effect and their drug therapy may have been modified by their physician,” contends Andy Szczotka, senior vice president of corporate clinical services at HealthTrans. “This may lead to potential medication waste and increased member and plan sponsor costs.”
“This is all done under the assumption that you’re improving adherence,” [Jerry] Shipkin [from SXC] says. “But I have not seen solid evidence that this improves adherence.”As an alternative, SXC sends its members auto-reminders with phone calls or e-mails to inform patients about their upcoming refill. “This is a more patient-friendly program,” Shipkin argues. “When you measure patient adherence on this program, it’s just not significantly lower than what you might get on an auto-refill program when you calculate the reversal.”
Van Antwerp contends that auto-reminders aren’t enough. “Everyone does auto-reminder programs,” he says. “In my mind, that’s the minimum that a pharmacy or PBM should do.”In addition, he argues, “anything can lead to accumulation if the patient is not using their medication and refilling their drug on a regular basis.” However, “how many patients do that?” he asks. “Drugs cost money.” While it could drive up more prescriptions, “no one’s going to pay for — and/or pick up — scripts they don’t need,” he maintains.
CVS Caremark Corp. claims its “Ready-Fill” program is “a convenience our members love,” according to Bari Harlam, the PBM’s senior vice president of marketing. The program includes auto-refills and auto-renewals. “There are a lot of people that have trouble being adherent, and this is a service that we offer to our consumers that helps do the work for them,” she tells DBN.
CVS Caremark members enrolled in the program receive notifications about their refill a few days before it’s shipped, and have the option of cancelling the refill. The PBM also calls its members’ physicians to request additional refills. “The physicians’ offices view this as part of the normal workflow, and retail and mail pharmacies are always reaching out to them for particular medications,” Harlam says.
JD Power Pharmacy Satisfaction Study
The study came out yesterday. I pulled the data from the executive summary into a powerpoint for all you visual people like me. Some interesting statistics on the value of pharmacy satisfaction and retention. Maybe this will create the business case for more tracking and focus on impacting satisfaction in pharmacy. I think we’ve seen that over the past few years for managed care with individual insurance.
Before you peek, who (pharmacy type) do you think gets the highest average ranking in satisfaction?
A Few Healthcare Factoids
I saw these in Money magazine (Oct 2010 pg 16) and thought they were worth sharing:
- Estimated increase in 2011 healthcare benefit costs = 8.9%
- Employee share of premium (for a family plan) in 2010 = $3,997
- Percentage of companies planning to increase cost sharing in the next 3-5 years = 43%
- Average family deductible = $1,518
- Employers rewarding workers who fill out health risk questionaires = 63%
- Percentage of employers penalizing employees for smoking and other health risks = 18% (29% plan to do it in the next 3-5 years)
- Percentage of companies that offer flexible spending accounts = 85%
- Percentage of workers that contribute to the FSAs = 22%
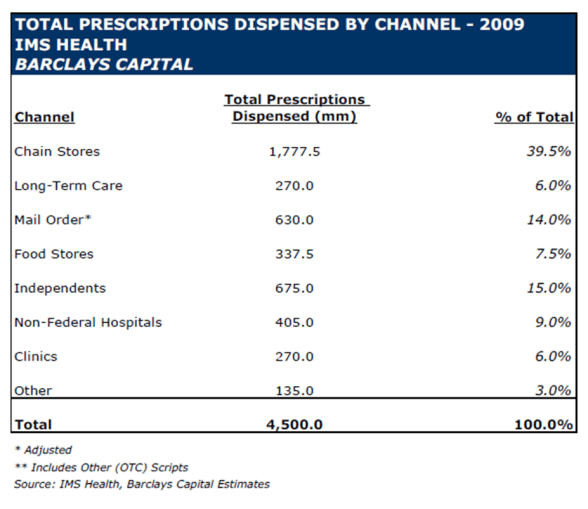
Total Prescriptions Filled In 2009 By Channel
Here is a chart from Barclays Capital based on their analysis and IMS Health data on prescriptions filled by channel last year.
Are Kid’s Backpacks Too Heavy?
I think the easy answer here is YES! You should go weigh your kid’s backpack. The experts say it shouldn’t weigh more than 10-15% of their weight. So, if my kid weighs 80 lbs, they can only carry 8-12 lbs of books. With the average textbook weighing 3-4 lbs, that’s not much.
Studies at the Mayo Clinic and at other hospitals around the United States calculate that overpacked or improperly packed school backpacks account for more than 7,000 emergency room visits annually. And according to the American Occupational Therapy Association, over 50 percent of all students between the ages of 9 and 20 suffer from chronic back pain related to the way they wear their packs. (source)
So, what do you do? I’d like to say that you don’t bring all you books back and forth and put everything online, but I don’t think that’s going to happen anytime soon. A logical answer is that you give the kids bags with wheels that they pull around. That seems easy enough.
A few other links on this topic which include other points:
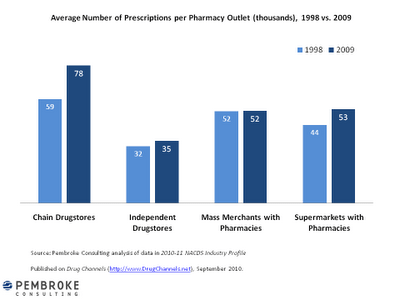
Pharmacy Productivity (Rxs / Yr / Location)
I found this on the DrugChannels.net blog. A good visual of the data showing how “productivity” has improved per location by different types of pharmacies.
What I think is interesting is that mass merchants have stayed flat. With Target’s original couponing strategy and Wal-Mart’s $4 generics, you would have assumed those had an impact that would show up here. I’m guessing the lift at independents could be explained away with increased utilization so the same number of patients go to the stores with just more scripts.
I’m not sure I have the time (or if the data is even available), but it would be interesting to look at patients per location and Rxs per pharmacist (and per pharmacy tech) by type of pharmacy.
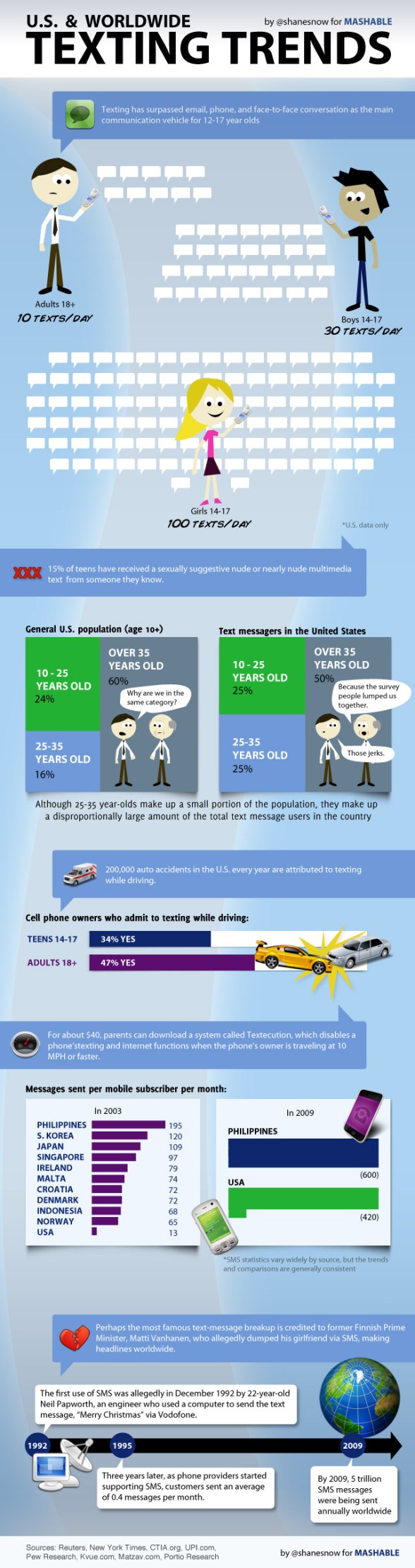
Texting Trends Infographic
I remember a few years ago when I got my first text. It was from the CTO at Accenture, and I had a phone that didn’t have SMS. I had to click thru a link to a website to see the text. I was totally flustered. How was I supposed to respond?
Well…I’m past that now. My brother and I send happy birthday via text. I find it easier to send a quick text when in a loud spot like the airport than to try and call. I’m sure my volume is still low. My friend said their kid did 15,000 in one month (which seems impossible). Another friend told me that their kids can text without looking. They sneak a quick peak and then respond without even pulling it out of their pocket (when their supposed to be off the phone).
We all know this is an emerging communication channel that will continue to evolve. And, smart phone use and adoption is expanding rapidly. So, here’s the infographic.
Mobile / Social Media Stats c/o HubSpot
I’ve never met the people over at HubSpot, but I like the information that they’re making available. (Thanks SF for the suggestion.)
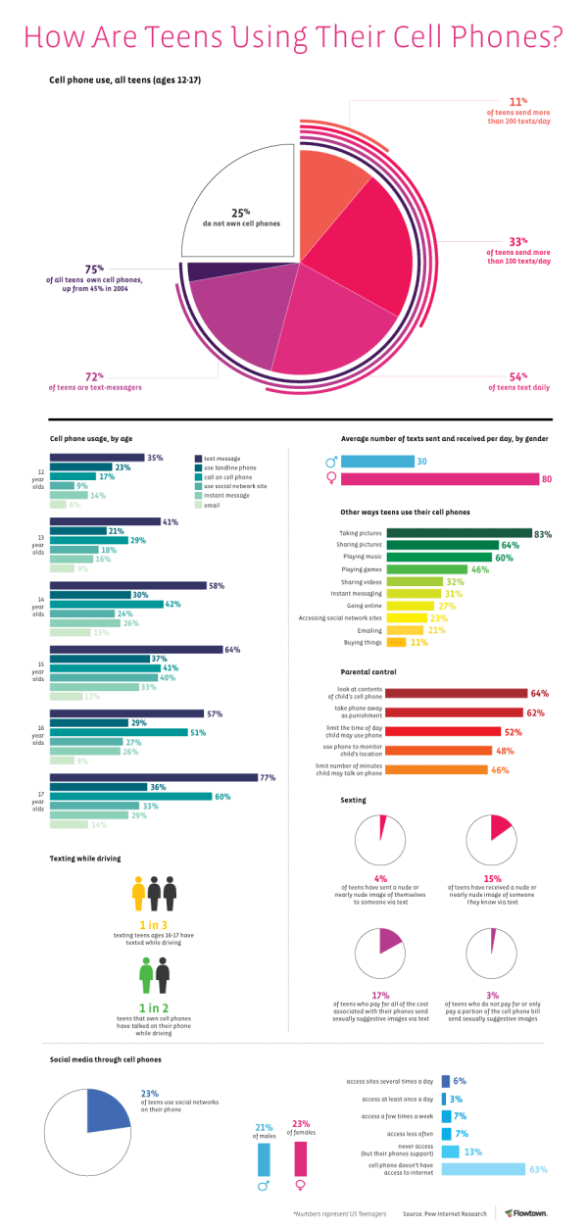
Here’s a few graphics from a recent post on their blog about mobile infographics. (BTW – I love infographics)
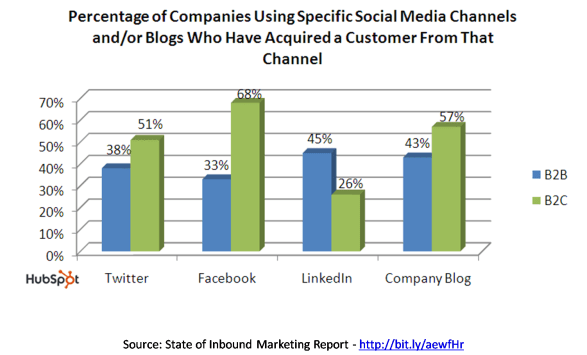
In another area of their site, they have some interesting data on how blogging and social media drives leads. Here are three of them that I found interesting.
Sleeping With Your Mobile Phone
There is lots of good data in the new Pew report on “Cell Phones And American Adults“. It shows that people who text a lot also talk on the phone a lot. It shows how adults use text messaging compared to teens. The one that stuck out at me was that 65% of people had slept with their phone.
Why do people do this? I do it if I’m using the phone as an alarm at a hotel, but otherwise, I don’t want the phone beeping at me at night with e-mails (legitimate or spam).
Does Playing An Instrument Increases Odds Of Being An MD?
I’m skeptical. My kid wants to be a physician so she was all upset yesterday when they played a video at school saying that 52% of kids that are in band in grade school go to medical school. There’s no time for her to play multiple sports, study, and be in the band so of course we said no.
I was in the band when I was a kid so it’s not an issue with the band. There are plenty of studies around music and academics. Not that I’m going to call the school out on the video, but I’d like to see the research. A quick Google search didn’t find anything on this correlation. I’d more importantly ask the question of what percentage of physicians played an instrument, at what age, and for how long. Did they play piano? Did they play the recorder? Did they play in marching band in college? Did they play in a heavy metal band? There is a difference.
I hate when groups “market” themselves hard to the kids. My son was all worked up a few weeks ago when the boy scouts talked about shooting guns and bows and arrows (neither of which I intend to let him touch for a while). He thought this was a way around me by joining boy scouts.
Anyways, if anyone knows about research on band (or other activities) and the correlation with being an MD (I prefer causality), please comment. Thanks.
Pharmacy Factoids From Old SWOT Analysis
I found this on the Internet while looking for something else. It’s a SWOT analysis (from about 2007) about Walgreens. You can tell it was written by someone who doesn’t understand all the industry dynamics. There’s no mention of mail order as a threat. There’s no discussion of PBMs. There’s no discussion of the value of specialty pharmacy. It’s pretty focused on the pure play retail strategy. Frankly, I’m pretty disappointed…BUT
What I did find interesting were some facts about the industry:
- Walgreens fills an average of 256 Rxs / day per store (in 2006) versus 100 Rxs / day per independent and 180 Rxs per day per chain.
- Walgreens (at the time) had drive-thru pharmacies at 80% of their stores and 30% of stores were open 24-hours per day.
- Free-standing stores generate 30% more in sales than pharmacies located in strip malls.
- 64% of Walgreen’s sales are generated by Rx (2005 analysis).
- A customer spends 10 minutes in the store if including an Rx purchase; 8 minutes if no Rx purchase.
- Only 30% of shoppers make impulse purchases.
- The average non-pharmacy store purchase in 2001 was $19.38.
- The average American visits a grocery store 2.2x per week but a drugstore once a month.
In case you don’t know what a SWOT analysis is…
How Seniors Use Social Media (Pew)
Not a big surprise…the Baby Boomers use technology. Many of us have had their parents, uncles, grandparents, etc., send them a “friend invite” or talk to them about technology. This will obviously continue as it’s more the norm and you have people that have been using technology for years age into retirement and look to connect with disparate friends and family.
Here are two charts from the recent report from Pew – Older Adults and Social Media. Very interesting to watch the trends.
NCPDP Nov 2010 Event: The New Economy And …
On November 2nd, NCPDP is hosting an educational event called “The New Economy and It’s Impact on Healthcare, Pharmacy, and the Patient.” Sounds pretty cool! It’s a topic we all talk about.
What does the new sense of frugality mean? What will new forms of insurance mean? How will pharmacy evolve? Will MTM work? Will MTM become a product for commercial? How is the consumer’s behavior changing relative to information and compliance?
The agenda includes yours truly along with people from:
* Kaiser
* Walgreens
* AARP
* Sanofi-Aventis
* North Carolina Association of Pharmacists
* Eaton Apothecary
* American Society of Consultant Pharmacists
* RegenceRx
Complexity of Decision Making
In today’s world, the amount of information is overwhelming. At the same time, we are constantly striving to practice DIY (do it yourself) medicine where we are reaching out to experts to help us sort thru information (especially when data is conflicting). But, a lot of that assumes we know what we need or we know when to ask for help.
A study published recently in the Annals of Family Medicine looked a small group of diabetics and how they received information about their condition.
They collected a nice long list of different sources used for information:
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
RESULTS Five themes emerged: (1) passive receipt of health information about diabetes is an important aspect of health information behavior; (2) patients weave their own information web depending on their disease trajectory; (3) patients’ personal relationships help them understand and use this information; (4) a relationship with a health care professional is needed to cope with complicated and sometimes conflicting information; and (5) health literacy makes a difference in patients’ ability to understand and use information.
CONCLUSIONS Patients make decisions about diabetes self-management depending on their current needs, seeking and incorporating diverse information sources not traditionally viewed as providing health information. Based on our findings, we have developed a new health information model that reflects both the nonlinear nature of health information-seeking behavior and the interplay of both active information seeking and passive receipt of information.
The Sandwich Generation
One of the things that I am surprised that we don’t hear more about is the sandwich generation. These are people who are caring both for children along with their older parents. According to Pew, 1 in every 8 people aged 40 to 60 fit into this category.
There are obvious implications in terms of managing health.
- Information challenges for these caregivers that have to manage information on their health, their kid’s health, and their parent’s health.
- Challenges in acting and coordinating this caregiver role while managing typical stresses of work, financial planning, and other things.
And, all of this puts a new requirement on health plans and health entities. How do you engage the caregiver? How do you track approval to send information to the caregiver instead of the patient?
What about when the caregiver is remote and there is a surrogate? How are decisions delegated? How do you create information and send it to multiple parties? Should the information be personalized to the individual knowing that perhaps my parents need certain information which I might need presented to me differently?
Other resources on this topic include:
Express Scripts Drug Trend Highest Among Trend Reports
I am sure there is a project at Express Scripts right now to figure out how to position this in the industry. I personally would go for claiming better adherence drives up drug trend (see prior post).
With five major drug trend reports out (Express Scripts, CVS Caremark, Medco, Walgreens, and Prime Therapeutics), there is only one more that I expect – SXC. I’m sure someone else could come into the market with a report, but it’s a lot of work.
The trend numbers so far are:
- 3.2% for Walgreens
- 3.4% for Prime Therapeutics and CVS Caremark
- 3.7% for Medco
- 6.4% for Express Scripts
Does anyone really care? Should they?
On the one hand, it’s a good marker, but the companies each have different mixes of clients (Medicare, Medicaid, Employer, Managed Care, Government). They also have different mixes of clients by geography. All of these things matter.
I would personally argue that we need a different key metric for the industry. The one challenge Express Scripts faces is that they really drove this metric for years and were able to set the standard. Now, they may be caught up in that legacy.
Some of the metrics that are used to compare PBMs:
- Generic fill rate – this is meaningful in that traditional PBMs make more money on generics but definitely subject to client mix
- Mail order penetration – this is meaningful in that it drives several other metrics and is where PBMs make money
- Drug trend – this is relevant in a traditional PBM sense that lower trend is better
- Cost share – this has held pretty flat for years while the absolute value has gone up
- Mail order satisfaction – this is generally a measure that everyone has as high and touts
- Client retention – it seems like everyone has high marks here while clients obviously move around
- Mail order fill accuracy – everyone’s at 99% plus so you get to differentiate at the six sigma versus two sigma level (which in scale matters)
I personally think average client cost per claim processed is a better measure. It takes into account drug mix (brand / generic). It takes into account rebates and rebates provided to clients. It takes into account retail mix (30 / 90 day) and mail order. It takes into account plan design.
I also think creating an average MPR (medication possession ratio) would be a relevant metric that more closely mapped to health outcomes and would still be within the PBMs sphere of influence. They can drive awareness and help with adherence programs thru the consumer, the pharmacy, and the prescriber.
I’m also a big fan of key metrics like:
- 1st call resolution
- Average inbound calls per claim processed (mail versus retail)
- Web utilization – # of registrants AND average visits per registered member per year
PBM Data – Apples and Oranges

When I first saw the data below from AIS’s quarterly pharmacy benefits survey (2Q 2010), I was excited. I hadn’t ever seen a breakdown of claims filled by tier across multiple PBMs. But, I was disappointed as I dug in.
| Percentage of Claims Processed per Tier, per PBM, as of 2nd Quarter 2010 | |||
|
% of Claims Processed |
|||
| Company |
1st Tier |
2nd Tier |
3rd Tier |
| 4D Pharmacy Management Systems |
78 |
16 |
7 |
| ACS, Inc. |
36 |
50 |
14 |
| Aetna Pharmacy Management |
64 |
20 |
16 |
| BioScrip |
50 |
39 |
11 |
| Burman’s Specialty Pharmacy |
90 |
8 |
2 |
| CIGNA Pharmacy Management |
67 |
26 |
7 |
| Envision Pharmaceutical Services, Inc. |
70 |
25 |
5 |
| Factor Support Network Pharmacy |
95 |
5 |
– |
| First Health Services Corporation |
48 |
37 |
15 |
| FutureScripts |
66 |
18 |
16 |
| HealthSmart RX |
48 |
41 |
11 |
| HealthTrans |
69 |
16 |
16 |
| Maxor National |
40 |
55 |
5 |
| National Pharmaceutical Services |
78 |
17 |
5 |
| Navitus Health Solutions |
68 |
28 |
2 |
| Northwest Pharmacy Services |
54 |
37 |
9 |
| OncoMed The Oncology Pharmacy |
90 |
10 |
– |
| Partners Rx Management |
72 |
19 |
9 |
| PBM Plus, Inc. |
60 |
35 |
5 |
| Prescription Solutions |
55 |
25 |
20 |
| Prime Therapeutics |
68 |
20 |
12 |
| RegenceRx |
73 |
15 |
12 |
| RESTAT |
71 |
17 |
12 |
| SXC Health Solutions/informedRx |
70 |
24 |
6 |
| United Drugs |
64 |
29 |
7 |
| Walgreens Health Services Division |
55 |
30 |
15 |
Where is the data from Express Scripts, Medco Health Solutions, and CVS Caremark? I’m sure someone chose not to participate, but I don’t think they would be hurt by these numbers.
Why are the numbers so different across companies?
- 1st tier ranges from 36% to 95%
- 2nd tier ranges from 5% to 55%
- 3rd tier ranges from 0% to 20%
What do I do with this? Do they all define tiers the traditional way (i.e., 1st tier = generics, 2nd tier = brand formulary, 3rd tier = non-formulary brands)?
Are they all even in the same business (i.e., a specialty only company might not have any generics)?
Do they serve similar populations (i.e., Medicaid is very different than commercial)?
Now, I could certainly drill in one by one. For example, if I pull out the companies that I believe have similar diversified clients, I get a few more focused questions:
|
1st Tier |
2nd Tier |
3rd Tier |
|
| Aetna Pharmacy Management |
64 |
20 |
16 |
| CIGNA Pharmacy Management |
67 |
26 |
7 |
| Envision Pharmaceutical Services, Inc. |
70 |
25 |
5 |
| FutureScripts |
66 |
18 |
16 |
| Navitus Health Solutions |
68 |
28 |
2 |
| Prime Therapeutics |
68 |
20 |
12 |
| RegenceRx |
73 |
15 |
12 |
| SXC Health Solutions/informedRx |
70 |
24 |
6 |
| Walgreens Health Services Division |
55 |
30 |
15 |
Now, I see some distinct clustering that maps closer to what I would expect. I would expect a PBM to have 65-70% generic (1st tier) utilization); 25-30% brand formulary (2nd tier) utilization; and 5-10% non-formulary brand (3rd tier) utilization.
The two things that jump out for me here are then:
- Why does Walgreens have such low 1st tier utilization? My general perception is that they do a good job at driving generic utilization and have incentives in place for their pharmacists to do that.
- Why does Navitus have only 2% third tier utilization? Do they have a closed formulary (i.e., no 3rd tier drugs are covered without some medical exception)?
In the same issue of Drug Benefit News (DBN 8/13/10) and the same survey, there were a few other data points:
-
The total number of claims processed by PBMs increased by 9.97% over the past year to 2.56B.
- Does that mean that the remaining ~600M claims are cash?
- Does that equate to a 9.97% increase in utilization or is that just more covered lives or more concentration of business among the PBMs that respond to the survey?
-
Average copays were:
- $9.98 for the 1st tier
- $23.69 for the 2nd tier
- $36.93 for the 3rd tier
IMHO (in my humble opinion), I think these copays show a problem…not with the data but with plan design. Generics should definitely be below $10 so we’re alright here although I would probably shoot for $8. A difference of $14 between tiers 1 and 2 is too low. $15 should be the minimum and $20 is probably better. The same goes for the $13 difference between tiers 2 and 3.
My ideal plan design would be $8, $25, and $45 (or the equivalent average using percentage copays).
The Power Of A Name
Believe it or not…Cows with names produce 68 more gallons of milk a year (according to Newcastle University in the UK).
So what does that mean for you? Imagine how important it is to treat your customers as people…or your employees. Think about that personal experience when you interact with a member. If you’re the consumer, think about how it makes you feel when you get a general message from your healthcare provider. Isn’t it better when it’s personalized to you?
Choices: Grande Skim Mocha With Whip @ 140 Degrees
Choices. We can all become overwhelmed with them. As several studies have shown, more choices are not better…they paralyze us and limit our ability to make a decision.
So what do we do with this. Choice is a double-edged sword. On the one hand, you want to offer choice to everyone. On the other hand, this can make implementation very difficult.
Like my Starbucks example. I can customize almost everything off a pretty basic menu…even the temperature. (BTW – they suggested using 140 degrees rather than saying kiddy temperature) But that makes it more difficult to standardize and should increase the risk of error. Imagine doing this efficiently and in scale.
Mass customization has been a challenge for years.
People can have the Model T in any color – as long as it’s black. (Henry Ford)
While technology allows this to a certain degree, it all has to be moderated. Let’s take communications. I could let every consumer tell me their preferences and other facts about them.
I want you to send me automated calls unless the information is clinical in which case I want a letter than I can share with my physician. I’d like the calls made to my home number between 5-7 pm or on Saturday’s between 10-4. I’d like you to leave a message and don’t call back unless I don’t act for seven days. If I interact with the call, please text me the URL or phone number for follow-up. I like to be addressed by my first name. I’m an INTJ so please use that as for framing the message.
You get the point. Where do you stop? And, do you really think that I know what’s best. I tell almost everyone to e-mail me, but depending on when it comes in, it could be days before I respond or even read the e-mail. That’s if it passes the spam filter.
I’m sure if I asked 10 people whether they wanted automated calls then 7 of them would say no, BUT you know what…good calls work (voice recorded, speech recognition, personalized). The vast majority of people interact with good, automated calls (some for 10+ minutes). Most people think about those annoying robocalls that use TTS (text to speech) we all get around the elections. But, good technology with a relevant message from a relevant party get people to care. It’s all about WIIFM (what’s in it for me). The other half of the equation is being able to coordinate the multiple modes. (e.g., I missed you so I’m sending you a letter. Let me text you the URL.)
So, should I let the consumer pick their preferences? Sure for certain things. But, what about a drug recall (for example)? Do I have to wait a week to get a letter? What can I personalize versus what should the company own. I pay for them to “manage” my health. Why don’t I let them?
There is no perfect system. You need a series of things to be successful.
- A database to track consumers – demographic data, claims data, preferences, interaction history, …
- A workflow engine with embedded business rules to manage communication programs with rules about what to do when certain situations arise
- Reporting to track basic metrics
- Analytics to understand and analyze programs
And, of course all this requires expertise to interpret and leverage the data for continuous improvement.
Are you doing all that? I doubt it…but you can be.
Creators, Critics, Collectors, Joiners, Spectators, and Inactives
Which of these are you? I’m clearly a creator and a joiner.
Forrester has created 6 overlapping groups of people from a social media perspective (paraphrased):
- Creators. These are people who publish on the web (blog, website, video, podcasts).
- Critics. These are people who post reviews online, comment on blogs, or contribute in other ways to existing content.
- Collectors. These are people who read lots of information and may vote or tag pages or photos.
- Joiners. These are people who have a profile on different social networking sites and visit them with some regularity.
- Spectators. These are people who read online information, list to podcasts, and watch videos but do not participate.
- Inactives. As suspected, these are the people who aren’t engaged in any of these social technologies.
The other thing that I think is interesting is their breakdown of these groups by percentage (Based on their North American Technographics Interactive Marketing Online Survey (Q2 2009)). As expected, in all these categories (except inactives), the younger age groups are more likely to represent these categories. For example, 46% of people 18-24 are creators while only 12% of people over 55 are creators.
- 24% of people are creators
- 37% are critics
- 21% are collectors
- 51% are joiners
- 73% are spectators
- 18% are inactives
A Collection Of Misc Articles
I’m in a clean-up mode in my e-mail and blog pile. For the first time in almost two years, I’m beginning to feel caught up. I have less than 250 e-mails (combined) in both my personal and work e-mail inboxes. This is a lot since once I open an e-mail I either (a) delete it; (b) respond immediately if possible; (c) file it in a folder on that topic; or (d) leave it in my inbox for future reading (i.e., it’s too much info to digest quickly) or for future response (i.e., it requires more time than I have).
It always begs the question of how late can you respond to something. Yesterday, I stumbled upon a e-mail from someone in Europe that wanted me to add their pharmaceutical site to my blogroll. I clicked on the link, reviewed the site, and added it. It took me less than 5 minutes, but the kicker was that he e-mailed me almost a year ago.
*****
- A study by Timothy Monk at the University of Pittsburgh concluded that keeping children on a stable schedule of activities can make them less anxious as they grow up.
- People with strong social connections are 50% more likely to live longer.
- People who regularly logged in to a weight-management website for 2 years lost 9-pounds (3x those that didn’t log in).
- Can a mouthguard make you a better athlete?
- A study in the July Health Affairs says that patients that use e-mail with their physicians have healthier outcomes. (Lots of challenges here, but this should be key in health reform.)
- Digital Darwinism…you have to develop relevance, interactivity, and accountability.
- MyPressurePoints.com – a survey and website focused on African-Americans with diabetes.
- Generic drug videos from Teva.
- 9 Leading Trends in Rx Plan Management by Medco.
- Two low-cost generics used by Kaiser to reduce heart attacks and strokes.
- Managing with the Brain in Mind – neuroscience.
- AMA and Medco study about physicians and pharmacogenomic testing
More to come…
Back To The Future: The Role Of The Pharmacist
Between the focus on differentiation and the focus on adherence, we have seen (and will continue to see) greater use of them as a strategic asset. CVS Caremark is leveraging them in their Pharmacy Advisor solution. Walgreens continues to leverage them at the POS. Medco is using them in their Therapeutic Resource Centers. And, the independent pharmacists have stressed this story for years.
In Medicare, the Medication Therapy Management (MTM) process begins to recognize the power of pharmacists and actually rewards them for their efforts. I was quoted in Drug Benefit News today about this topic. Here were a few quotes:
“The pharmacist is an under-utilized resource today,” George Van Antwerp, vice president of the Solutions Strategy Group at Silverlink Communications, tells DBN. “They go to school to work with patients and often end up simply filling bottles.”
While the benefits of pharmacist intervention are undeniable, Van Antwerp says, the challenge is finding the right balance of face-to-face interaction and automation. Issues also include getting a good return on investment for such services by condition and the fact that only an estimated 60% of the people picking up prescriptions are the patients themselves. In addition, “the staffing model right now would be stressed if pharmacists were spending significant time on cognitive services,” he maintains.

 October 12, 2010
October 12, 2010