It’s an interesting question. If I pay you $30 to take your medications every month, will you be more likely to actually take them or will you be more likely to tell me that you took them? I was talking to someone about their program yesterday, and a lot of it comes down to measurement. If, for example, I get paid if I open the pill bottle every day and that data is stored somewhere, I’m surely going to open it regardless of whether I take the drug. (At least I think that’s what human nature would do.)
1, 2, 3 of picking benefits
In the November 2009 Time magazine, they suggest three things you should do when picking benefits:
- Don’t just default to your current plan. Spend the time to compare copays, premiums, deductibles, and estimate out-of-pocket costs. [too bad most plans don’t give us an easy to use model of what you would have spent last year under the different plan options] They also suggest opening a HSA (Health Savings Account) if you go with a high deductible plan.
- Fund your FSA (Flexible Spending Account). They estimate that you save $350 for every $1,000 you deposit (and use).
- Test your wellness. Many employers (and health plans) offer different forms or tools to test your wellness and health. You should know the results and you may even get paid to do it.
“Insights” Gone Wrong
There is a great “cartoon” at the end of the recent Fast Company magazine that gives an example of how using information can lead you to a wrong decision. It’s one of the reasons that I always point out the difference between someone who has provided services to an industry and someone who has worked in an industry. It’s not the same. Sometimes, you need to truly understand the nuances and how decisions are made.
It also made me think of a great Facebook example of how using social connections can lead to bad business decisions. Given all the talk about making peer-to-peer recommendations based on your social network, this is a slippery slope to watch. We are still new to this area and mistakes will happen. One of the bigger ones that I have heard occurred in Facebook where they allowed advertisers to use member’s pictures. Well, how do you think people felt when they saw the advertisements that say “Meet Singles In Your Neighborhood” with a picture of their spouse. It didn’t go over well.
Great idea. Interesting technology. Bad application.
This will happen in healthcare. The question is who will be first to stub their toe in the new world.
Mail Order Pharmacy – Good or Bad (Two Surveys)
I love when two parties (both with their own agenda) publish data that clearly shows that they are right. Now, in this case, one quotes a 3rd party so I do give them more credibility. And, the other (as I will show below) seems to not take the patient’s responsibility in mind.
First, PCMA (Pharmaceutical Care Management Association) publishes research from JD Power on pharmacy satisfaction. It shows that insured and non-insured patients are generally satisfied with their pharmacy experience. Mail order clearly came out on top of all types of pharmacies. (Given that only 12% of people know the name of their pharmacist, I would expect them to be more closely clustered together.)
The J.D. Power and Associates study measured customer satisfaction with the pharmacy experience across major national retail drug store chains, mass merchandisers and supermarket stores, and mail-order channels. The study examines seven factors that contribute to consumer satisfaction with brick-and-mortar pharmacies and five factors that determine satisfaction with mail-order pharmacies. The average overall satisfaction index for each of the pharmacy distribution channels were:
- Mail-order pharmacies: 834
- Supermarket pharmacies: 820
- Mass merchandiser pharmacies: 801
- Retail chain pharmacies: 798
Then (no big surprise here) NCPA (National Community Pharmacy Association) puts out a survey of 400 patients showing how dissatisfied they are with mail order.
- They are unhappy being forced to use a lower cost pharmacy. (GVA – get used to it as part of healthcare reform)
- They complain that their prescriptions don’t arrive on time (which could impact adherence). (GVA – did they call in time or wait for the last minute…were they adherent to begin with)
- They complain about their medications changing (i.e., titrating to a different strength). (GVA – they shouldn’t move to mail until they’ve stabilized and any mandatory plan I’ve ever seen required at least 2 months as the same strength before requiring movement to mail)
- They complain about getting different medications than what they ordered. (GVA – I bet most of that was people getting the chemically equivalent generic.)
This isn’t something that will easily get solved. The FUD (fear, uncertainty, and doubt) out there rules in many cases and statistical anomolies are what get discussed. I would love to compare complaint rates, error rates, and satisfaction for patients that use both channels (retail and mail).
Why Wellness Matters
I’ve had an intense month so I’m hoping to catch up on my big pile of blogging ideas this week. We’ll see.
Here’s one I pulled the other day. I liked this graphic from MVP Healthcare in their corporate profile.

It hammers home all the key points – regression to the mean, focus on the high cost individuals, and cost is avoidable if you focus on preventation and education and successfully engage the consumer.
Time To Kill The “Clean Plate Club”

I always thought this was something that only my parents talked about until recently when I heard a few friends use the same term – “clean plate club”. So, maybe more of you are familiar with these words:
“You have to finish what you were served. Don’t you want to be part of the clean plate club? People are starving around the world while you have all this food.”
I just assumed that my dad who was one of eleven kids who grew up in the Depression had this as a reality of limited food. It took me years to realize that this framework was a recipe for disaster in today’s age. When you go to restaurants that serve you huge plates of food and apply this mental framework, you are bound to over-eat site.
This is a great example of how something framed early in life can drive behavior. That’s one of the key concepts when planning healthcare communications is understanding the frameworks that consumers / members / patients have about their physician, their health insurer, their pharmacist, generic drugs, mail order, and a variety of other healthcare topics.
Nature’s Rules For Healthcare
I found this article – Nature’s 10 Simple Rules for Survival – on biomechanics and biomimicry interesting (Fast Company article). It looks at how nature has survived all these years and translates that to lessons for business. This is worth more pondering, but my Saturday morning thoughts on applying this to healthcare are in brackets.
- Diversify across generations. [We need different strategies for different segments. One size will not fit all.]
- Adapt to the changing environment — and specialize. [We need a US centric healthcare model not a model from Canada or the UK.]
- Celebrate transparency. Every species knows which species will eat it and which will not. [Be clear on incentives and roles. Set up a win-win not a win-lose. Don’t try to get government to run an efficient business which it never has.]
- Plan and execute systematically, not compartmentally. Every part of a plant contributes to its growth. [A technology infrastructure and shared decision making across a care continuum is important. The medical home concept has merit.]
- Form groups and protect the young. Most animals travel in flocks, gaggles, and prides. Packs offer strength and efficacy. [Social networking and leveraging peer-to-peer education and support will improve health outcomes.]
- Integrate metrics. Nature brings the right information to the right place at the right time. When a tree needs water, the leaves curl; when there is rain, the curled leaves move more water to the root system. [We need home monitoring and predictive metrics for preventative care. Using genomics and other measures should save lives by allowing us to act early.]
- Improve with each cycle. Evolution is a strategy for long-term survival. [Big bang improvement to the system won’t work. Pick one problem at a time – e.g., un-insured – and solve for it.]
- Right-size regularly, rather than downsize occasionally. If an organism grows too big to support itself, it collapses; if it withers, it is eaten. [Healthcare is inherently local.]
- Foster longevity, not immediate gratification. Nature does not buy on credit and uses resources only to the level that they can be renewed. [We need to address the issue of hyperbolic discounting. People want immediate value, but lots of healthcare improvements take time personally and systemically.]
- Waste nothing, recycle everything. Some of the greatest opportunities in the 21st century will be turning waste — including inefficiency and underutilization — into profit. [Don’t overcomplicate the solution. Sometimes the obvious can improve the difficult.]
The 5 Questions (Regence Group)
Regence Group recently put out an interesting website – www.whatstherealcost.org. It takes an unorthodox (for a health plan) approach to delivering several important points. It reminds me of what Wellpoint has done with Tonik or some of the things Humana is doing at HumanaGames.
One of the things I found interesting and very straightforward for patients to think about were their 5 questions:
- How much does that cost?
- Is that really necessary?
- Is there a cheaper option?
- Is there a generic for that?
- Has anyone out there had this before?
Imagine if every time we were asked to take a test or start a new therapy that we (patients) asked these five questions of our provider.
Deloitte 2009 Survey of Health Care Consumers
This is based on a Deloitte web-survey of 4,001 Americans in October 2008.
- 73% are confused about how the US healthcare system works
- Over 1/2 believe that 50% or more of healthcare dollars are wasted
- 7 of 8 Americans believe themselves to be in good health
- 1 in 3 are interested in working with a health “coach” to help them create and stick to a plan
- 68% are interested in home monitoring devices that would check their condition and send results to their MD
- 3 in 5 say financial penalties would improve their adherence
- Only 1 in 3 Rx users say they compared treatment options
- 22% say they looked or asked for information about a health insurance plan in the last 12 months
- 9% have a PHR
- Physicians who are more prescriptive (paternal) were preferred by a ratio of 2:1
- 8 in 10 say they would consider switching from a physician recommended Rx if a pharmacist (RPh) indicated a cheaper alternative was available
- Only 12% said they understood the term – biologics (should they?)
- 35% are willing to accept a smaller provider network for a reduced premium and lower copayments
- Only 25% favor increasing taxes to help cover the uninsured
Their major conclusions were:
- Health care is a consumer market
- The health care market is not homogeneous
- Cost concerns are changing behaviors
- Consumers want holistic care and resources to pursue wellness and healthy living
- Consumers embrace innovations that enhance self-care, convenience, personalization, and control of their personal health information
Could / Should Healthcare Follow The Car Dealer
Healthcare is one of the few industries where more supply equals more demand. (Maybe the only one.)
So, as we look at the healthcare shortage of PCPs, RN, and RPhs, should there be more discussion of closing locations? Should we pursue the tact of the car manufacturers in closing dealerships to have less locations? This would fly in the face of the MinuteClinic type of strategy.
Or, I guess the better question is whether there are certain points in the process where more access points are needed, but there are other points in the process where less access points are needed. For example, do we really need 6x,000 retail pharmacies in the US. Certainly, in some urban and suburban locations where the average person passes more than 3 pharmacies to get to the one they use, the answer is no. In some rural locations, there is no option other than the one pharmacy that is 20 miles away.
Would this change our behavior? I believe analysis would show that less testing facilities and more difficult access to certain tests would certainly change their use. Would this address the problem or simply create more services that were being done outside the system (i.e., cash businesses)?
I don’t know the answer, but I haven’t heard anyone talking about what seems like a logical discussion.
Finding A New Name
I have received notice that I can no longer use the “Patient Centric” term. Apparently, it’s a Trademarked name.
As I am looking at new names, I have come across a new series of blogs and sites.
1. I first looked at “The Engaged Consumer”
2. I looked at “Healthcare Communications”
- A new book and blog around this.
3. I looked at “Health Engagement”
4. I looked at “Member Engagement” which is open, but I’m not sure it’s the right terminology.
I welcome any thoughts. I am working on a few more right now.
New Clinical Webinars – HEDIS, Adherence, Engagement
In June, we are offering three complimentary webinars to our clients and prospects on key topics of discussion.
Increasing the Effectiveness of Population Health Program Engagement
June 16th | 1:00 PM ET
Getting consumers to take charge of their healthcare behaviors and choices is critical to controlling costs and improving outcomes. Successfully welcoming and engaging consumers in DM and health management programs can be the toughest road for health plans and population health organizations. Strategies that motivate participatory engagement are key – but it takes more than a friendly voice and the right script.
Join Silverlink for a complimentary webinar where we will discuss the challenges of moving health behaviors and effective strategies organizations can implement to get ahead of the behavior change curve.
In addition, learn how to:
- Leverage tailored messaging to drive high engagement rates
- Enable continued engagement over time
- Maximize buy-in and acceptance of health coaching
- Combine multichannel approaches to elicit engagement and re-engagement
- Optimize engagement campaigns through predictive analytics to drive results
Drive Positive Health Behaviors and Improve HEDIS Results
June 23rd | 1:00 PM ET
Whether your focus is on the HEDIS measures for women’s health, the diabetes metrics or a broad range of effectiveness of care measures, Silverlink can design communications strategies that increase your reach, motivate member action and improve HEDIS results.
With the backdrop of the economic slowdown, communicating with members about the importance of key preventive screenings is more critical than ever. Explore the many routes to break through health prevention challenges by tailoring communications interventions that work for your populations.
Join Silverlink for a complimentary webinar where we will present the results and lessons learned over several years in supporting HEDIS screenings including a recent campaign aimed at reducing health disparirities in African American and Hispanic populations related to colorectal cancer screenings.
In addition, learn how to:
- Use a flexible framework that supports national teams in delivering effective outreach in local markets
- Drive performance on high-profile HEDIS measures where plan performance has hit a plateau
- Segment your membership to deliver highly personal messages using multiple levers
- Design and target messages to help reduce health disparities
- Combine multiple messages to support members with more than one gap
- Leverage multichannel campaigns to maximize reach and action
Rethinking Medication Adherence
June 30th | 1:00 PM ET
More than 50% of consumers become nonadherent around their maintenance medications within the first 12 months of therapy. And, today’s economy is putting even more pressure on people to make economic tradeoffs that threaten their health. Several studies have shown that more people are skipping doses or not refilling medications. Non-adherence leads to $177B in direct and indirect costs to the healthcare system per year.
Silverlink provides a comprehensive suite of communications services to drive medication adherence from targeting and messaging to multi-channel campaign management and execution. Join Silverlink where we will discuss some of the common myths around and key strategies related to medication adherence.
In addition, you will learn about:
- Critical success factors in designing adherence solutions
- Important conditions to focus on for adherence
- Success metrics and key measurements
- Comprehensive solutions for all phases of the patient’s therapy from initiation through long term maintenance
Expanding the Role of the Clinic
I think the fact that Walgreen’s and CVS Caremark are expanding the role that the clinics can play in healthcare is a positive thing. There will be lots of debates about how much can be handled at the clinics versus the physician’s office, but I think the key point should be that today’s model doesn’t work. Chronic diseases are not managed. We provide sick care not well care.
Launched over the last four years to care for such simple ailments as ear and sinus infections, strep throat or pinkeye, retail clinic operators now are training nurses to do specialized injections for such chronic conditions as osteoporosis and asthma.
In addition, they are offering treatments for advanced skin conditions that include removal of warts and skin tags or closing minor wounds. Care for minor “sprains and strains” also is being offered at some retailers, and pilot projects are underway for breathing treatments and special infusions of drugs derived from biotechnology.
We need to figure out how to lower the costs, make the system more accessible, get patients engaged, and drive people to preventative care. I don’t know if the clinics can do this, but if they can, we should embrace them. I think both companies are very well positioned to drive change with their breadth of services. They touch the consumer on a regular basis and have the ability to use data, technology, and localized care to engage patients.
Medco 2009 Drug Trend Report
Here are my highlights from Medco Health’s 2009 Drug Trend Report:
- Overall trend was 3.3%. (1.3% excluding specialty drugs.)
- Specialty trend was 15.8%.
- Their generic fill rate was 64.1%.
- Interestingly, they broke out trend to show that clients with over 40% mail use had a trend of -0.7% while those with less than 40% had a trend of 5.8%.
- I do like the generic distribution chart below although it is for 2008 Q4 while their 64.1% number is for the average of 2008.

- They point out that utilization growth was negative 1.1% last year which was the first time in a decade. What I was surprised at is that they didn’t “blame” the economy for this. Most surveys I have seen say or imply that people are taking less medications because of the increasing cost burden while their overall wealth is decreasing.
- Medicare costs increased 6.8% for their PDP (prescription drug plans).

- I think it’s interesting in helping companies focus their management efforts when they project that “in the next 3 years more than 85% of drug trend will be driven by drugs in six categories: cardiovascular, endocrine/
diabetes, central nervous system, musculoskeletal/rheumatology, respiratory, and oncology”. - In a brief section about the unwired state of healthcare, they share some scary statistics:
- A review involving the medical records of 41 million Medicare patients identified $8.8 billion in error-associated costs and 238,837 preventable deaths. Moreover, a large subset of these errors are medication errors.
- An estimated 1.5 million preventable serious medication errors occur each year, with $217 billion (2006 dollars) in associated costs.
- Since people are always asking for quantifiable value around adherence, I liked the chart below which showed the survival rates over years based on adherence vs. non-adherence.

- They introduce a new metric – Generic Opportunity Score (GOS). It takes into account both chemical and therapeutic opportunities for generics to be used.
- They also provide some details on a brand-to-generic $0 copay waiver program which had a 14% success rate. That’s pretty good from what I have seen.
- Here is a breakout of the specialty pharmacy categories:

- Now, where they do credit the economy is with improving generic fill rate, mail order utilization, and client’s use of trend management programs.
- They show trend by age group with the lower age groups growing faster. They also showed a nice graph of utilization by state.

- Below is their chart on where trend growth in the future is projected to occur (which should tell you where to focus preventative action).

Do Consumers Understand Cost of Individual Insurance?
In a study done by Kelton Research on behalf of eHealthinsurance.com, I found a few interesting data points:
- 65% of people don’t think they could afford health insurance for more than 6 months if they lost their job. (Since most Americans live paycheck-to-paycheck, that shouldn’t be surprising.)
- Only 26% knew that individual health insurance is cheaper than COBRA although COBRA can be a lot less expensive with the Obama subsidiary.
- 31% think that they would be denied coverage by another plan versus the actual denial rate which is closer to 11%.
- To stay covered, only about 50% would be willing to spend less on cell phones or cable TV.
- Only 40% would be willing to pay more than $200/ month.
Why Does WSJ Villanize CVS Caremark?
I was so annoyed when I read the WSJ this morning about CVS Caremark charging more for members that go outside the CVS store or mail order. Come on guys. This is a basic tiered network design. It’s not unlike tiered formularies or preferred drug lists.
First, it’s a plan design that was created and offered to clients. Some clients choose it. That’s not CVS Caremark’s issue. Anyone could do this and offer it.
Second, what’s different between this an mandatory mail or retail buy-up. If you choose a higher cost location, you have to pay more. You’re getting the same drug at a higher cost facility.
What frustrates me the most here is that we will never reform healthcare and drive out costs if people want to have their cake and eat it too. You think you can have total flexibility and manage costs. We have to make some hard decisions and push people to drugs, locations, treatments, etc. that offer similar quality at a lower cost. That’s not going to be easy.

Express Scripts 2009 Drug Trend Report
I always enjoyed being part of the team that put the Drug Trend Report out when I was at Express Scripts from 2001-2006. With that in mind, I do await anxiously to see what new information they will share each year. I will say that the core fundamentals (as always) were very strong in the 2009 report, but I missed not having any client case studies in the document.
They reported drug trend of 1.5% (without specialty) and 3% with specialty.
Specialty drug trend was 15.4%.
Patients paid an average of $12.82 per Rx.
They say that more patients converted to Home Delivery (aka mail order). [I have to check this. My recollection is that mail volume was relatively flat and this would be hard to achieve unless they had more people filling less drugs on average at mail.]
They reported PMPY utilization of 14.32 Rxs.
Their members paid 29% of the generic drug costs; 19.6% of the brand costs; and 22.3% overall for traditional drugs. For specialty drugs, they paid 2.3% (or 20.2% for all drugs including specialty).
They have a section on compliance (which is rapidly becoming a key discussion point in the PBM world). I was a little surprised they didn’t call it adherence which is more common these days. But, they revealed some surprisingly high MPR (medication possession ratio) numbers for antidiabetics, antihypertensives, and lipid-lowering drugs. Considering adherence is where a member has an MPR of greater than 80%, they showed 77%, 83%, and 83% respectively. Since we know that 50% of people (on average) drop therapy within 12-months, this seems improbable on a book-of-business basis. (Maybe I’m just becoming a cynic in my old age.) The only reason I could find to explain this example was that this was not based on new starts (i.e., NRxs) unless they came in the first quarter. Therefore, there might be some selection bias in that they are taking MPR on people that started the year on the medication and may therefore have been people who were more likely to be adherent. I would rather see this done on a rolling 12-month basis.
As I often use, they define waste in the system and give you a potential GFR (generic fill rate) goal for the top therapy classes.
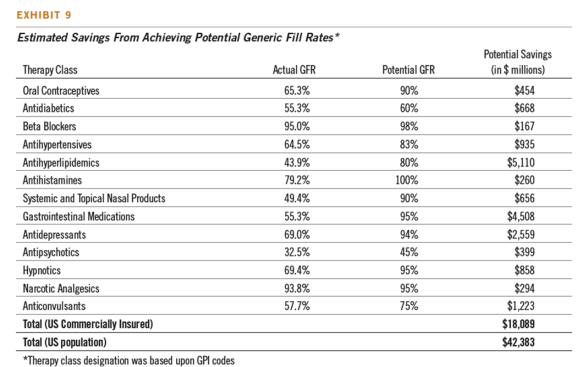
Their analysis shows that 55% of the costs for specialty drugs were billed through the medical benefit rather than the pharmacy benefit.
55% of their members are in plans with at least one step therapy module.
They talk about a few studies they have published showing that targeted and framed messages are more effective than general messages. And, that those messages are more effective with mail order users than people at retail.
Again, there might be some selection bias here as people at Home Delivery may simply be more active in managing their healthcare. The other question I have had for a few of my friends there has been whether we are comparing apples-to-apples. Since I ran a few of the programs before I left, I know we did a lot more interventions (web, inbound IVR, outbound calls, messaging on the invoice, letters, POS rejects) than we did for retail (letters and outbound IVR). If they’ve adjusted for that, than this is clear. If not, I would want to see that adjustment made.
As anyone who reads the blog knows, I am a big supporter of the theory behind their Consumerology story. I think Larry Zarin and Bob Nease have done a great job putting together their advisory board, creating case studies, and using behavioral economics. I always talk with our clients about these theories, and our analytics team is constantly helping clients define test plans that use these.
- Social comparison
- Hyperbolic discounting
- Loss aversion
In comparing adherence at retail and mail, one thing that came into my mind was whether a driver of better adherence was a longer time window to refill. Typically, you have a refill-too-soon (RTS) edit in place until 2/3rds of the medication has been used (based on days supply dispensed from dispense date). At retail, that means you have about 10 days. At mail, that means you have about 30 days (less the 7 days for shipping). Does that make a difference?
I was also surprised under the methodology section that they now include rebates in calculating costs. It’s a quick one-line comment but how did that effect trend or other metrics here…and if so, how significantly?
As always, I love the therapy class reviews in the back that give you great numbers like:
- Cost PMPY
- # Rxs PMPY
- Prevalence of Use
- Average Cost / Rx
- # Rxs / User / Year
The Personalization of Health Care
With genomics and other tools, it seems possible that we could one day see completely personalized health care. Of course, the immediate reaction will be won’t this mess up risk pools. [I am sure there is someone smarter than me that will figure out how to make that piece work.]
What I see is the following:
- Understanding personality types would allow patients to be matched to providers.
- Genetic testing would allow for better predictive models on what individuals with need in terms of coverage.
- Genetic testing will allow for the creation of personalized medicine.
- Better predictive models will allow for better care plans and preventative medicine.
- More transparency will allow people to make better decisions (e.g., calories displayed at restaurants).
- Ubiquitous technology will integrate health decision making into everyday processes and tools.
- Technology will allow companies to develop personalized, targeted communications that are based on patient preferences, historical responses, personality type, and experience to drive healthy behaviors.
Could we eventually get to the point where each of us had an adaptive plan that covered different things as we grew older and constantly optimized our care team or medical neighborhood based on our needs?
Of course, the risk comes when the models are wrong, but if you applied some of the chaos theory logic to a traditional modeling strategy and the current underwriting programs, who knows?
Not something for the next few years, but something I was noodling on the other day.
CVS Caremark TrendsRx Report 2009
This is one of my favorite times of year. After working on the Drug Trend Report at Express Scripts for several years, I love to get all the trend reports from the PBMs and read them. The first one that I have had a chance to review is the one from CVS Caremark. I found it an easy to read document with good case studies and a mix of strategy and tactics.
Here are some of my highlights and observations:
- 3 out of 4 clients cited “reducing health care costs” as their primary measure of PBM success…AND 2 out of 3 prioritized “plan participant behavior change” as the way to reach that goal. [Maybe the plan design bigot is finally dead.]
- With pharmacy spend approaching $1,000 PMPY, I found their chart on potential cost reduction a simple way of pointing people to things they should think about.

- A 10% improvement in diabetes adherence can save $2,000 in annual health care costs. [I assume this is based on improving MPR and would definitely like to learn more on how the health care costs are quantified.]
- They layout three objectives – improve use of lower cost drugs, improve adherence, and get people to take better care of their health. [Similar to the concept I laid out in my white paper of needing to be broader than just Rx benefit management.]
-
They talk about two of their solutions:
- Consumer Engagement Engine (CEE) which is very similar to what Silverlink does and provides business logic for targeting the right member at the right time with the right message.
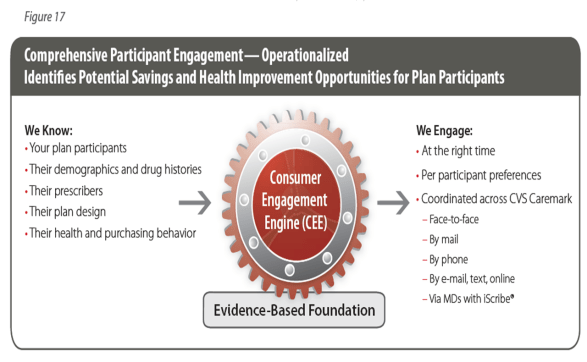
- Proactive Pharmacy Care is their “medical neighborhood” concept to stitch together their entities – Mail Order, CVS retail, Specialty, MinuteClinic, and their disease management company.
- Consumer Engagement Engine (CEE) which is very similar to what Silverlink does and provides business logic for targeting the right member at the right time with the right message.
- Their trend was 3.9% PMPM in 2008 (or 2.8% excluding specialty drugs).
- Medicare Part D utilization was up 4.1% compared to 0.8% for the rest of their BOB (book of business).
-
Their GDR (generic dispensing rate) averaged 65.1% for 2008 and was 66.3% in December 2008.
- Best in class employers = 68.2%
- Best in class health plans = 73.4%
-
As they remind you, a 1% increase in GDR is roughly equal to a 1% reduction in pharmacy spend.
- [What I would like to see is improvements in GDR from new drugs coming to market in 2008 versus improvements that came from clients implementing plan design.]
- They say [which I preach all the time} – “proactive consumer engagement improves results and lowers the risk of disruption. For best results, provide personalized actionable information at a range of touchpoints.”
-
I saw a few interesting things in one of the case studies they share about their “Generous Generics” program. [Does that name get used with consumers? What’s their reaction to it?]
- $0 generic copay at mail [that should drive volume]
- 10% coinsurance penalty for not shifting to mail after the second fill [similar in concept (I believe) to the Medco “retail buy-up” concept]
-
Top Ten Therapeutic categories (53% of spend):
- Antihyperlipidemics
- Ulcer drugs
- Antidiabetics
- Antidepressants
- Antiasthmatics
- Antihypertensives
- Analgesics, Anti-inflamatory
- Anticonvulsants
- Analgesics, Opioid
- Endocrine and Metabolic Agents
-
They state that the population of diagnosed diabetics is growing by roughly 1M a year.
- Executive Summary, Economic Costs of Diabetes in US in 2007, American Diabetes Association, March 2008
- Executive Summary, Economic Costs of Diabetes in US in 2007, American Diabetes Association, March 2008
- They state that a generic for Lipitor is now expected in Q4 2011 [which I think is about a year later than originally expected]
-
They show some data from their Maintenance Choice program which I think has a lot of opportunity.
- This is where you can get a 90-day Rx from either mail or a CVS store for the same copay. [The key here is for them to understand member profitability and for CVS Caremark to understand how to drive consumers to the preferred channel.]
- [I would really need to understand their profitability by channel because if I read the chart in here right, it would appear that given the choice 45% of those at mail would choose 90-day at retail…a scary concept for mail order pharmacy.]

- They give a case on Maintenance Choice which leaves me looking for a key fact. They state that a recent implementation has a goal of 70% of the client’s day’s supply will go through the preferred network (CVS) or mail and that 20% of it goes through mail today. [What percentage goes through CVS today? If it’s a client in Boston, that one scenario. If it’s a client in Chicago, that would be another feat.]
- Specialty pharmacy trend was 13.5%.
- They say that pharmacogenomic testing is being used more frequently for specialty drugs. [I would love to know more…how often? For what drugs? Has it improved outcomes? Are their clients covering it? How are they playing in this space?]
- They talk about adherence which continues to be one of the hottest areas in the Rx arena today. They give stats showing 15-48% improvement across different metrics and up to $142 in cost avoidance in one case. [Are these again control groups? What was the cost / benefit analysis or ROI? Is this improvement in average MPR (Medication Possession Ratio) or improvement in the % of people with an MPR of >80%?]
- They talk about 88% of heart failure patients maintaining optimal prescription adherence compared to a norm of less than 50%. [My questions here (which isn’t apparent) is whether this was an opt-in program so the 88% is for engaged and active participants or whether it was across all targeted members.]
-
They provide a quick list of factors that will impact drug trend:
-
Driving costs:
- Aging
- Obesity
- Diabetes
- Specialty pipeline
- More aggressive treatment guidelines and earlier diagnosis [which hopefully would lower total healthcare costs]
- DTC advertising
-
Reducing costs:
- Economy – reduced utilization and improved GDR
- Increased availability of generics
- FDA safety reform
- Lackluster non-specialty drug pipeline
- Utilization and formulary management
- Consumer price transparency
-
Communication Strategy Regarding H1N1 (Swine) Flu
“There is a lot of media, a lot of news, a lot of rumor – the sooner you can get correct and accurate information to consumers, the better – otherwise people will look to other sources that may not always be accurate.” (Jan Berger, President of Health Intelligence Partners on podcast)
We have been hearing a few things from our clients and have put some information up on the Silverlink website. Some of the comments have been:
- I have seen a spike in call center volume about this topic.
- Clients want to change plan design to make sure Relenza and Tamiflu are covered and don’t require a prior authorization or have a quantity level limit on them.
- We want to proactively reach out to at risk populations – children, seniors, or people with a compromised immune system.
- We want to be able to flexibly target certain geographies.
- We want to remind people not to panic, drive them to quality information sources, and make sure they know the basics – wash your hands.
At a minimum, everyone is adding information to their websites. Many consumers are Googling the topic or following updates from @CDCEmergency (on Twitter).
Healthplans, PBMs, and population health companies are at the heart of this. They need a coordinated strategy to inform people appropriately as this issue continues to be top of mind.
We recorded a podcast last night with the Medical Director from Healthwise and Jan Berger who is the former Chief Medical Officer from CVS Caremark and is now president of Health Intelligence Partners. In here, they answer some general questions about the situation and what companies should be doing to educate members.
The two standard solutions Silverlink is offering clients are:
- Offer an inbound FAQ (Frequently Asked Questions) line with CDC content and specifics about their plans. This can help with overflow from their call center and/or be used as a direct line from their website or outbound communications.
- Selectively target populations (age, zip code, disease state) with a brief message reminding them to wash their hands and telling them where to get qualified information.
As with all our communications offerings, these can be customized (messaging, channel, targeting, etc.) to meet client requirements. Additionally, since one of our technology advantages over others in the space is our flexibility, we can work with clients to keep these messages up-to-date as the situation changes and as new information has to be added.
Swine Flu (H1N1) Continues To Top News

(picture from http://www.myfox8.com/lifestyle/health/la-sciw-swine-masks28-2009apr28,0,4461177.story)
It’s amazing how this has dominated traditional media and blown away the online media.
- CDC on Twitter
- CDC website
- PandemicFlu.gov site
- Video of the CDC director
- Podcasts, videos, buttons, widgets, etc.
I few things that stick out for me:
-
The CDC’s policy on school closing would shut schools for 14-days when there is a confirmed case nearby. That would shut down work and be a huge strain on people if they didn’t get paid.
- I’m sure it’s the right thing to do to wait out the gestation period, but it would be a huge strain on the system.
- High school sports being cancelled in Texas.
- College graduation being held but no hand-shaking.
- People wearing masks which really don’t do anything.
- Biden telling his family not to travel.
- Companies not allowing workers that were recently in Mexico to come back to work.
- Pork futures are down.
- My church is no longer going to have communion wine where there could be shared germs.
- I have heard about huge spikes in prescribing of Relenza and Tamiflu and pharmacy shortages.
One of my favorite pictures that goes right to the health literacy issue is the following.
NOTE: This is not what H1N1 flu is about…hence the dropping of the “swine flu” term.

(picture from http://cuteoverload.com/)
Digital Consumer Presentation by John Sharp
Here is a good presentation by John Sharp of the eHealth blog:
Communication Evolution
I was thinking this morning about how communications evolve. Here are a few examples from the past few years:
1. Caller-ID replacing voicemail.
2. E-mails replacing memos (and getting much longer).
3. SMS and Twitter replacing e-mail.
4. Scanning replacing faxing.
5. Facebook replacing online photo albums.
6. Evite replacing invitations (with mixed success).
7. Twitter beginning to replace news clipping services.
8. Craigslist replacing newpaper listings.
9. Websites replacing brochures.
10. Virtual conferences eroding attendance at physical conferences.
7 Points in 7 Minutes
In looking at the Ix Therapy blog about the conference they just had with Health 2.0, I found this note which I found very interesting…
James Hereford made 7 fabulous points in 7 minutes about building Ix into the delivery system:
- You have to deliver what patients want (doesn’t matter how cool the technology is).
- It has to make sense for clinicians from a clinical perspective.
- It has to make sense for from a clinical workflow perspective.
- Focus processes on the value proposition for the patient (I may have mangled this one a bit).
- Information needs to be common, ubiquitous, and well-designed.
- Health care is all about trust; whatever we do needs to enhance trust in the patient-provider relationship.
- Incentives are critical.
Pharma Rx Costs Tied To Outcomes
Given our opinion that the PBM industry would be moving to more outcome based pricing, the articles today about Merck and Cigna‘s deal on pricing based on outcomes is very timely. I “tweeted” about it early in the AM, but I have got the article sent to me by a lot of people. So, here are a few of the things being said:
WSJ Blog –
Now Merck and Cigna have announced what they’re calling a “performance-based contract” for Merck’s diabetes drug Januvia. But the deal is actually the reverse the pay-for-performance ideal: Merck will get paid less per pill, not more, if the drug works well.
Under the deal, Cigna will get a discount on the drug if patients’ blood sugar falls. Cigna will get additional discounts if patients faithfully take the drug when they’re supposed to. (These two variables often go together — taking the drug faithfully helps keep blood sugar down.)
Cigna PR –
“Merck should be recognized as the first major pharmaceutical company to offer increased discounts on its oral anti-diabetic products, supporting CIGNA’s efforts to reduce A1C levels for individuals with diabetes, regardless of what medication they may be taking,” said Eric Elliott, president of CIGNA Pharmacy Management. “Improving people’s health comes first for both CIGNA and Merck. We hope this agreement will become a model in the industry.”
So…it seems like an aligned deal. Merck and Cigna want adherence. Employers want lower costs and better outcomes.
Consumers Don’t Care About Wellness
Here’s a good provacative quote from Forrester…are all the wellness efforts doomed or are incentives the minimum requirement to play?
“Health plans keep saying that they have to improve consumer engagement and that one of the best ways to do this is by engaging them in wellness initiatives. The data tell me that consumers don’t care about wellness. Employers do. But while most employees may hear the [wellness] message, they also ignore it….”
— Carl Doty, VP and research director at Forrester Research, told AIS’s INSIDE CONSUMER-DIRECTED CARE.
Whitepaper: The Future of the PBM (Pharmacy)
As we have been working with a lot of PBMs over the past year, the question has come up many times – “where do you see the industry going?” After bouncing some ideas off a few of you, we have pulled together a whitepaper with the Silverlink Communications perspective. Certainly, each area of the whitepaper could have been its own chapter, but rather than turn this into a thesis, we are publishing it.
As I have said in a few recent articles including the one in HCPro, I think the Express Scripts acquisition of NextRx will likely accelerate a few of our predictions here.
The executive summary of the whitepaper is below. The final whitepaper is available here.
I would welcome any comments you have…
Executive Summary
In the next several years, we believe that three changes will drive the pharmacy marketplace and ultimately change the business model for PBMs. These changes will be accelerated by the current financial crisis which may drive further consolidation in the short-term. Consolidation which we believe will accelerate the “race to the bottom” where the traditional model of scale has been maxed out with parity achieved among the large PBMs.
1. The need to better engage the consumer in understanding their benefits and ultimately responsibility for their care;
2. The effort to automate and integrate data across a fragmented system and across siloed organizations; and
3. The shift from trend management to being responsible for outcomes.
Consumer Engagement
The industry-wide movement to consumerism will continue to affect plan design, but it will also thrust PBMs and pharmacies into the critical path of member engagement. With pharmacy being the most used benefit as well as the volume and accessibility of retail pharmacies, they will play a critical role in driving adherence and helping consumers understand healthcare. This will renew the focus on cognitive skills, medication therapy management and ultimately drive the desire for a more traditional “corner store” approach that can be scaled using technology.
Combining this with the macro-economic forces that are driving ubiquity of technology through mobile media and the evolution of the Internet from a pull media to a push media will also challenge the PBMs and pharmacies to innovate. They will be required to look outside of healthcare models to identify the right communications to drive behavior. PBM’s and pharmacies will have to leverage behavioral economics and personalization technology to get the right message to the right consumer at the right time through the right medium.
Automation and Integration
The consumer engagement challenges will only exasperate some ongoing challenges within the PBM and pharmacy community. This will include the lack of staff to provide more cognitive services and the general fragmentation of data across organizations and functional silos. Figuring out an overall “single view of the patient” which shows all the touch points and offers a coordinated multi-channel strategy for inbound and outbound communications will become a major focus.
In addition, in order to make these solutions efficient, the development of predictive models, much like the clinical and underwriting solutions being used today, will become the norm across the industry. As these models are fine tuned and the promise of e-prescribing becomes more of a reality, the channel for engaging physicians in the member’s care will finally exist. PBMs and pharmacies will be able to use data to allow physicians to understand when patients aren’t being compliant and when there is an opportunity to drive change.
From Trend Management to Outcomes
The traditional business model for the PBMs has been based on large scale negotiations to drive rebates and efficiencies within mail service – cost to fill and acquisition costs. At the same time as those efficiencies reach a maximum discount, the traditional tools for managing trend will have run their course. Although plan design won’t “die”, comparative effectiveness may reduce (or eliminate) the need for formularies, and in general, the ability to shift cost to the consumer above the 25-30% level will be difficult.
Both of these challenges will push the PBMs and pharmacies into a role where they are focused on driving health outcomes and being part of the bigger solution across the industry. They have a strong footprint to drive this change and as theranostics (or personalized medicine) evolves there will be an opportunity to find cost effective solutions to change the prescription landscape.
Promotion vs. Nudging vs. Mandatory Mail
Although there is always a dialogue about the lifecycle of mail order, I think some of the work out of the Consumerology group at Express Scripts is interesting. The frameworks that they apply internally are very similar to the technology and approach that Silverlink uses with the rest of the market. [Kudos to Sean Donnelly and Bob Nease for their work on this new approach.]
The traditional ways of driving mail order have been:
- Over a copay incentive (and hope)
- Letter and calls encouraging member to convert
- Providing a call center to facilitate the conversion to mail (from an inbound call or from a transfer on an automated outbound call)
- Mandatory mail – requiring the member to use mail or pay the full cash price for the drug
- Retail buy-up – allowing the member to keep getting the maintenance drug at retail (after 2 fills typically) but requiring them to pay a penalty for choosing a higher cost channel
Now, “Select Home Delivery” uses the 401K approach of opt-out vs. opt-in to drive participation. As behavioral economics would suggest, inertia will carry the momentum and by getting the member signed up in mail and moving them to mail will drive success versus requiring them to take an action. The idea here is to “nudge” the member versus force them or leave it up to them to take action.
Select Home Delivery optimizes the use of cost-saving Home Delivery, requiring members to opt out of the program rather than the traditional approach of requiring members to opt in. The program is based on the psychological principle of hyperbolic discounting, which says immediate events (for example, the hassles of signing up for Home Delivery) loom large compared to downstream benefits (such as a lower overall copayment and receiving a 90-day supply). Dr. David Laibson, an economics professor at Harvard and member of the Center’s advisory board, conducted research showing that applying this principle to 401(k) programs dramatically improved participation rates.
“Opt-out and active decision programs for 401(k) enrollment dramatically improved low employee participation rates. We wanted to explore whether these tools could also solve healthcare challenges,” Laibson said. “This is one of the first marketplace adaptations that successfully applies behavioral economics to improve healthcare.” [quotes from Consumerology blog]
I think the new results from their blog (below) are impressive. [BTW – If you’re a member at Lowe’s or another client which has used this, I would love to hear your reactions.]

Express Scripts Outcomes Conference Begins
As with each annual Outcomes conference, Express Scripts (ESRX) has released their annual trend numbers. Here are a few of the highlights from the press release:
- Overall pharmacy trend = 3.0% (down from 5.5% in 2007)
- Estimate consumers and employers are paying $42B too much in 13 therapy classes by not optimizing generics.
- On average, a generic drug is over $90 cheaper than a brand name drug.
- Generic drug usage increased by 7.5 percent, while utilization of brand name medications decreased 11 percent.
- 67.3 percent of all prescriptions that Express Scripts filled were for generic drugs by the end of 2008. [I didn’t like the comparison which was an average across the 12 months ending in Sept 2008 from IMS of 63.7%…not apples to apples.]
- In 2009, at least 20 branded drugs are expected to become available generically.
- Over the next five years, more than $66 billion worth of branded drugs are expected to lose patent exclusivity.
“Using generic drugs that are safe and effective can help lower costs while still driving value for patients and employers,” said Steven Miller, MD, senior vice president and chief medical officer at Express Scripts. “Our results indicate that cost control is achievable through careful management of appropriate use of drugs and delivery channels, without shifting costs to consumers. Although the trend is the lowest it has been in over a decade, significant opportunity to lower spending still exists.”
“Finding ways to reduce spending without compromising health outcomes is the top priority for healthcare reform, as the Obama administration recognizes,” said Alan Garber, MD, PhD, Henry J. Kaiser Professor and director of the Center for Health Policy at Stanford University. “We have long used financial incentives to try to eliminate waste. Now we’re finding that tools that build upon the insights of behavioral economics and psychology can have powerful, positive effects.”
“In today’s economy, we are not only tracking wasteful spending across the country but developing strategies to reduce it,” said George Paz, chief executive officer at Express Scripts. “By applying the principles of behavioral economics we are helping consumers make better and more cost-effective healthcare decisions. We understand we cannot eliminate waste alone and we are committed to working alongside likeminded organizations, such as the Federal Coordinating Council for Comparative Effectiveness Research, to continue to identify strategies to improve our healthcare system.”
“Studies have repeatedly shown that people work much harder to avoid losses than to pursue gains,” said Bob Nease, PhD, the company’s chief scientist. “This suggests that a ‘stop wasting money’ message is more effective than a message focused on potential savings. In addition, by applying evidence-based segmentation, we have practical insight into which members are likely to be most sensitive to loss aversion. One size does not fit all.”
The $40B HealthCare Opportunity Around Retention
It’s obvious to anyone close to it, but harder to align the goals to take advantage of it. With people “aging-out” from group plans to Medicare and people leaving their employer coverage to go to the individual market, managed care has a huge opportunity to retain that business by providing them a transition path. According to McKinsey (and from what we see), that’s generally not happening.
A few facts from their report:
- 68 percent of all members aged 60 to 64 have never been approached by their current insurers to discuss retirement options.
- more than 80 percent of respondents aged 60 to 64 said they would consider purchasing an individual product from their current carrier if they left their jobs or retired.
- Only 33 percent of 60- to 64-year-olds thought that their insurers offered Medicare products, for example, when in fact almost all major carriers do.
It’s also a simple economic problem. They are less expensive to retain and convert while their a member than once they are on the open market. You may even save on broker fees. Developing a data driven approach to create timely and personalized communications along with a service to transition them should be a priority.


 October 20, 2009
October 20, 2009 

