I found this site listing some of the top diabetic bloggers and also found this infographic there.
Is War A Good Framework For Addressing Cancer?
A physician asked me this a few months ago, and I thought it was a great point. We were discussing the fact that there are often times when we (the medical institution) may try too hard to “cure cancer” (see some of the points in my post about palliative care). When it’s viewed as a war that has to be won, it may be that too much effort is spent to beat cancer into remission rather than thinking about the patient’s experience. (see cartoon from naturalnews.com below)
A friend game me this example…While his brother’s cancer was in remission, the toll of the chemo and the other treatments was so much that he was never able to work again. The patient would have preferred to be able to work a few more years and die of cancer, but that discussion never happened.
In general, I believe most physicians would consider this a failure. They’re taught to “beat” the disease not to back off and let the disease “win”. But, I often hear about the “war on cancer“.
Even after 40 years, we still have a large amount of annual deaths from cancer.
Infographic: Obesity
Unfortunately, I don’t think a lot of this will surprise many of you, but it’s scary to think about the impact of obesity across different industries. For some of them this is big business. And, while I don’t think employers have fully realized how to focus on this from a “wellness” or “disease management” perspective, I think that will change.
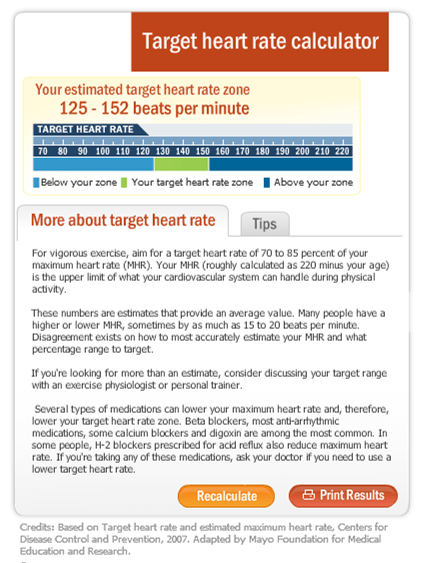
What Is My Maximum Heart Rate?
If you’re like me, you get on the treadmill or other exercise equipment at the gym and see it talk about exercising at X% of your maximum heart rate. Or, you get a heart rate reading on the device and wonder what it means.
It appears that the simple answer is to take 220 minus your age. For example, if you’re 30, then your maximum heart rate would be 90.
Now, when I plugged my age into a Mayo Clinic site, it shows me all the caveats about this answer.
Is Your Specialty Pharmacy A Dispenser, An Advocate, Or An Innovator?
Specialty drugs are expected to represent 40% of total Rx spend by 2020 so guess what…they’re the focus. Generic Rxs represent 80% of the oral drugs dispensed today and are low cost. PBMs, pharmacies, and payors are and should be focusing on specialty drugs.
Of course, this is driving a shift towards price compression and medical management types of functions like PA, UM, ST, case management, and even disease management.

So…what should your specialty pharmacy be focused on?
- Integrating medical and pharmacy benefits and data (a lot easier said than done as many have tried and failed).
- Using technology to engage physicians including social media, iPad apps, and EMRs.
- Providing a holistic solution that enables patients to self-manage, understand their disease, and improve their adherence to minimize waste and improve outcomes.
- Work with providers to be part of the broader care team and subsequently the shift to P4P (pay-for-performance) from FFS (fee for service).
I think this is going to require a tighter coupling of population health companies with specialty pharmacies and potentially better leveraging pharma manufacturers as partners versus suppliers.
This is not just a cost challenge…this is about outcomes. I usually think of it in terms of “The Triple Aim” which is about cost, quality, and experience.
If you look at your specialty pharmacy partner, I think you could put them in 3 buckets:
- Dispenser – Focused on operational metrics (TAT, ASA) and lowest cost dispensing.
- Advocate – Focused on “hub” type services that address basic patient needs (mostly patient out-of-pocket costs) and look at pharmacy focused case management.
- Innovator – Focused on using technology and data (medical, pharmacy, lab) to create differentiated outcomes through patient engagement, participating in the care team, and personalizing medicine.
9 Lessons From BlueZones
I got to see Dan Buettner, author of BlueZones, present a few times and love some of the insights from his research. The other day, there was a list of these nine lessons in USA Today:
- Move naturally
- Know your purpose
- Kick back
- Eat less
- Eat less meat
- Drink in moderation
- Have faith
- Power of love
- Stay social
It’s worth digging into his research if you’re looking at how to live longer.
Articles That Caught My Attention – mobile, mHealth, vaccines, gaming, social media
I’m getting a little backed up in terms of articles and ideas that caught my eye so I’m going to share a few of them here.
- Ubersense – looks like an interesting mobile app to help you with sports coaching.
- MakerBot – 3D printing for your home…how exciting!
- RedLaser – scan a bar code and find the lowest price…I have to try this.
- GenieMD – a simple interface for tracking your healthcare data in one free app
- ZocDoc – 1.8M MD appointments booked online using this app in August…seems to be getting some energy
- 19 states still allow paddling in schools (Time article – Spanking in the Schools) – seems pretty archaic to me
-
Top motivators for getting vaccines (Directions Research for Walgreens):
- 74% – pandemic / outbreak
- 67% – doctor recommendation
- 42% – CDC recommendation
- 27% – preventative health measure
- Evernote – smart notebook…may be something I actually buy!
- Specialty Pharmacies and URAC Accreditation
- Using video games in cancer therapy
- CDC social media kit
- Patient Engagement Is the Blockbuster Drug of the Century – Part II
- PWC research – Healthcare Unwired
- Targeting for care management
- Steve Jacobs website – http://unitedstatesofhealth.com/
- Doctors and social media
- When The Rx is an App
- Moving beyond legacy systems in healthcare
- Stamp size blood tests for liver damage
Using Gilligan To Drive Colonoscopies
While I do applaud the creative concept here, I wasn’t overly impressed with the creative itself. At the end of the day, the question for me is results. Did it pay for itself? Did it get more people to get colonoscopies (in the target audience) than otherwise would have? I’m unsure of that.
Here’s what I did find in a HealthLeaders article…At the end of the day, I’d want to compare that to a program we did at my last company for UHG in this area.
The campaign also netted 44 colonoscopy appointments. Of those 44 appointments, 13 were current Good Samaritan patients and 31 were new to the hospital. Forty-three of the 44 scheduled an appointment through the call center and one booked online. Of those who called, 27 cited the radio spot as how they found out about the service. More than half of the patients were in the target group of 50–59 year olds, with 24 female and 20 male.
Healthcare In 2020 – Best Book I’ve Read In A Long Time
Healthcare in 2020 by Steve Jacob is a great book. Lots of facts. Lots of relevant information. A quick read. Well referenced. If I could, I would send this to every client I’ve ever worked with to help them understand why changing healthcare is so important.
I’m going to share a handful of things from the book here. Even if I could provide you with a detailed summary, I wouldn’t. You need to read this book.
- Estimated MD shortage by 2020 is >90,000 and nurse shortage is 600,000-1M.
-
A great quote from two bioethicists (Daniel Callahan and Sherwin Nuland):
- The medical system’s “main achievements today consist of devising ways to marginally extend the lives of the very sick … for a relatively short period of time – at considerable expense and often causing serious suffering to (the patient)”.
- Of the 30-year increase in US average life expectancy in the last century, only 5 years can be credited to advances in medical care. The rest is from public health measures.
- The number of people 65+ will double to 1.3B globally by 2040 and the elderly will outnumber children <5 for the first time.
- The percentage of people who work out 12 times a month dropped from 53% in 1988 to 43% (in 2009).
- Doctors advise only about 1/3rd of their obese patients to lose weight.
- The most frequently reported “moderate activities” by US adults are food and drink preparation and lawn and garden care. [Not particularly high on the calorie burning schedule.]
- Nearly 3 out of 4 cancer deaths are attributable to smoking.
-
In a 2009 report, about 75% of adults 17-24 were ineligible for the military because they had:
- Failed to graduate high school
- Were physically unfit or
- Had a criminal record
-
1 of 3 homes in US metro areas have at least one problem that can harm health:
- Water leaks
- Peeling paint
- Rodent infestations
- Cancer screenings find lots of pseudo-disease – i.e., abnormalities that meet the criteria of being cancerous but will never grow to become harmful.
-
Surveys show a lack of participation in programs:
- ½ hadn’t been screened for colon cancer.
- Only 7% used nurse help lines
- <5% of people eligible used smoking cessation or weight management programs
- 3 of 4 people didn’t get a flu shot
- Use of decision aids has reduced rates of major elective surgery by ¼ without affecting patient outcomes or satisfaction.
- A physician would need to practice 18 hours a day to provide all the recommended preventative and chronic disease controls to their patients.
- A 2005 study found that nonclinical staff does the most effective job of managing patients with diabetes.
- Per the IOM 2005 report, 30-40% of healthcare spending represented “overuse, underuse, misuse, duplication, system failures, unnecessary repetition, poor communication, and inefficiency.”
- The FBI estimates that 3-10% of healthcare spending is lost to fraud.
- In a research study, parents with sick children saying they had Medicaid or CHIP coverage where turned down 2/3rds of times and had to wait 22 days longer for an appointment than those with private insurance.
- About 40 US surgeries a week are performed on the wrong person or wrong body part.
- 1/3rd of families lost most or all of their savings because of a terminal illness.
Some scary data points. This book was a great reinforcement of some of the projects I’ve been involved with trying to accomplish the Triple Aim – Quality, Cost, Experience.
10 Healthcare Trends To Monitor in 2013
I came across the chart below and thought I would post it with my perspective on trends for next year.
- “Accountable Care” in the form of CMS ACOs or Patient Centered Medical Homes will continue to expand. I predict some companies will begin to provide the infrastructure such that providers don’t have to come up with the $2-4M in capital needed.
- Integrated “Big Data” looking at pharmacy, medical, lab, AND patient reported data AND physician EMR data will be the rage to mine and use in predictive models.
- Consumer engagement around health will continue to be a huge focus.
- Obesity will continue to be an issue that people struggle with and employers begin to focus more actively on managing.
- mHealth in the form of mobile apps, connected devices, telemedicine, and remote monitoring will begin to move from the innovators to be a more standard component of the solutions with ROIs being more standard.
- The core components of health reform will remain (regardless of who wins) and the shift of people from underinsured and uninsured into the insured pool will finally be the tipping point for provider access and push growth in the clinics and telemedicine (video and phone) world.
- Transparency will become something that consultants begin to mandate and try to get into contracts around pricing, claims auditing, and other services across the entire healthcare spectrum.
- Hospitals will continue to buy physicians and look at how they can play a more dominant regional role especially outside of the urban areas.
- Consolidation will continue across all areas – providers, payers, pharmacy, pharma, technology.
- Investment in healthcare will continue to outpace other industries.
Should NY Hold The Marathon This Weekend? (SuperStorm Sandy)
 This seems like an interesting question, but one with perhaps a straightforward answer. With NY and NJ devastated by Superstorm Sandy and almost 4M still without power, should NY try to hold their marathon this weekend? Seems like a clear no to me.
This seems like an interesting question, but one with perhaps a straightforward answer. With NY and NJ devastated by Superstorm Sandy and almost 4M still without power, should NY try to hold their marathon this weekend? Seems like a clear no to me.
I do understand the fact that this is a big revenue event for the city. I do understand that you want to show your ability to recover from the storm. BUT, it takes resources – volunteers, police, hotels, food, and other efforts to pull this off. Wouldn’t those resources be better focused on the people that are still trying to dig out of their homes and get power?
Wired Health Survey
The same Wired article had some highlights from their Wired Health Survey. Here’s a few data points that caught my attention:
-
How many caffeinated drinks do you consume a day?
- 0 = 16%
- 1-2 = 56%
- 3-4 = 22%
- 5-6 = 4%
- 6+ = 2%
-
Most popular exercise types:
- Walking 62%
- Weight training 42%
- Running 37%
- Cycling 34%
- Yoga 21%
- Swimming 18%
- 73% of respondents take a supplement.
-
On average, how many hours of sleep do you get each night?
- 3-4 = 2%
- 5-6 = 39%
- 7-8 = 55%
- 9-10 = 4%
-
78% of respondents say that tracking their personal health metrics has helped them reach their goals. (Quantified Self) Here’s what they track:
- Height or weight = 64%
- Fitness or activity level = 46%
- Blood pressure = 39%
- Cholesterol = 33%
- Heart rate = 28%
- Vision or hearing = 26%
- Sleep habits = 26%
The Wired Guide To Health
I was reading Wired Magazine (Oct 2012) last night, and I came across this article “Living By Numbers: The Wired Guide To Health”. It gives “18 data-driven ways to be happier, healthier, and even a little smarter.” In my words, it’s a nice cheat sheet of some basic things we should all know (and many of which I’ve blogged about over the years).
- Conserve your willpower: it runs out.
- Shorten your workouts. (high intensity interval training)
- Make a sport-specific playlist. Music is the ultimate motivator. Choose your workout tunes carefully.
-
Learn to read a scientific report.
- Causation versus correlation
- True size of the effect
- Statistical power
- Conflicts of interest
- Don’t ignore data.
- Check your genome.
- Sleep or else.
- Know whether to caffeinate or nap.
- Be a discerning pill popper.
- Eat this meal. Load your plate for maximum nutrition not maximum taste. L
- Beware of food trends.
- Do the right things at the right time. (circadian rhythms affects sports)
- Heighten your senses with a call of duty. (gaming can make you quicker and more focused)
- Get to know your poop bugs.
- Dial in your happiness.
- Avoid unnecessary procedures.
- Get a standing desk.
- Learn to live longer. (Blue Zones)
Are You Part Of The Quantified Self “Movement”?
I’m not sure whether to call it a movement or a trend or some other term, but I think it’s very interesting. This idea of capturing and tracking data manually and through devices fits very well with the idea of “Know Your Numbers” in healthcare.
Here’s the descriptionof Quantified Self from Wikipedia:
The Quantified Self is a movement to incorporate technology into data acquisition on aspects of a person’s daily life in terms of inputs (e.g. food consumed, quality of surrounding air), states (e.g. mood, arousal, blood oxygen levels), and performance (mental and physical).
The movement was started by Wired Magazine editors Gary Wolf and Kevin Kelly in 2007as “a collaboration of users and tool makers who share[d] an interest in self knowledge through self-tracking”. In 2010, Wolf spoke about the movement at TED, and in May 2011 the first international conference was held in Mountain View, California.
Quantified Self is also known as self-tracking, body data and life-hacking. It is described in articles such as this one in the Economist and this in Forbes.
With an increasing amount of devices on the market that can be integrated (e.g, FitBit), we will see a huge rise in remote patient monitoring where the patient takes a greater role in this effort. Even know you are seeing more efforts to integrate devices into the “smart home” with a focus on older patients, but I think this smart home concept will continue to grow.
This Slideshare presentation is a nice summary…
Stand Up To Cancer At World Series

If you were like me, you were surprised and impressed to see all the Stand Up To Cancer signs at last night’s World Series game in San Francisco. It was impressive, but it made me wonder who this company was. Here’s some text from one of their press releases.
Stand Up To Cancer (SU2C) — a program of the Entertainment Industry Foundation (EIF), a 501(c)3 charitable organization — raises funds to hasten the pace of groundbreaking translational research that can get new therapies to patients quickly and save lives. In the fall of 2007, a group of women whose lives have all been affected by cancer in profound ways began working together to marshal the resources of the media and entertainment industries in the fight against this disease.
SU2C’s “Dream Team” approach to funding translational cancer research enables scientists from different disciplines at research centers across the country and internationally to collaborate on projects geared toward getting new, less toxic treatments to patients as quickly as possible. Monies also support innovative cancer research projects that are often deemed “too risky” by conventional funding sources. Sixty-five institutions are currently involved. As SU2C’s scientific collaborator, the American Association for Cancer Research, led by a prestigious SU2C Scientific Advisory Committee, provides scientific oversight, expert review of the research projects and grants administration.
I also grabbed a screenshot of some of the factoids from their website:

Less Than 20% Trust A Pharmacist To Help Them Make Healthcare Decisions – Surprising?
Whenever you go to the pharmacy, they always ask you if you have questions and make you sign off that you were offered counseling. It begs the question of whether anyone actually does. I just got this survey data e-mailed to me, and I wanted to share it since it was surprising to me and from RxAlly.
I also found it surprising that people don’t think their pharmacist can help them make healthcare decisions. This is certainly relevant in the Medicare world where AARP and others have partnered with pharmacists traditionally. Additionally, I think it limits some of the longer term opportunities for pharmacy, pharmacists, and PBMs. I’ve always thought that given their frequency of patient intervention that there would be lots of opportunities to leverage the pharmacist at the POS to close care gaps and be very engaged in the overall care and driving health outcomes.
Only 15 percent of U.S. adults have ever discussed a medication maintenance regimen with a pharmacist and only 49 percent have discussed any new medication with a pharmacist. Less than 20 percent (18%) of U.S. adults trust a pharmacist most to help guide and inform healthcare decisions for themselves and their families. A majority of people trust their doctor most (72%), followed by friends and family (36%), spouses or significant others (36%) and the internet (22%).
Source: RxAlly
http://rxally.com/rxally-news.html
Familiarity vs Importance Provider Gap Around Population Health Management
The ideas around Population Health are certainly critical both to us as a country to eliminate the waste in our healthcare system, but they are also foundational in a move from a fee-for-service (FFS) environment to an outcomes-based payment model. Interesting, if you look at a study that was just released, it continues to show a disconnect within the provider community. (Study is Population Health Management In Physician Practice: A Call To Action.)
I believe some of this stems from the costs associated with the build out, integration, and use of these technologies in today’s environment. But, I think some of this stems from a broken connection between national policy, localized implementation, and payer coordination around key healthcare issues such as obesity.
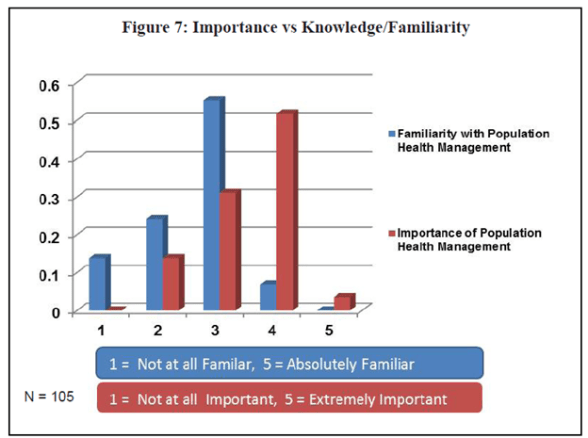
The following paragraph from the same document is also very telling.
“With 72% of respondents reporting that they had either already adopted or were in the process of adoption a patient-centered model of care, it was interesting that only 19% of practices self-reported as Patient-Centered Medical Home (PCMH) and only 10% as an Accountable Care Organization (ACO). Considering the critical role that population health management will play in both types of practice models, the data suggest that while they are undertaking population health management initiatives, many practices may not yet be at a level of transformation to warrant presenting as PCMH or ACO at this point in time. Also interesting is that of the 11 practices that did self-report as ACO, only 5 of the 11 also reported as PCMH – showing again perhaps another disconnect or struggle with implementation and understanding. PCMH, after all, has been described as “foundational” to Accountable Care Organizations.”
A lot of this change won’t be done by physicians, but it was promising to hear in the same report that:
- 96% of large provider practices employed Nurse Practitioners;
- 70% employed Physician Assistants; and
- 91% employed Care Coordinators.
So, how are those resources being used today? And, how do these resources get integrated into an overall care strategy for the patient? Are notes shared with external care managers? How do we find the right point person? How does an external payer team for MM coordinator with the local resources for something like discharge planning?
What Is Population Health Management? Or Medical Management? Or Disease Management?
This is one of those terms that is thrown around a lot just like Medical Management or Disease Management.
I thought it would be helpful to define the 3.
Population Health Management (PHM) is…
“Programs targeted to a defined population that use a variety of individual, organizational, and societal interventions to improve health outcomes” (Mathematica Policy Research Issue Brief, August 2011)
Medical Management (MM) is…
“The general term often applied to the practices of utilization management (UM), case management (CM), and disease management (DM), alone or in combination with each other.” (Trends and Practices in Medical Management: 2001 Industry Profile)
Disease Management (DM) is…
“An approach to healthcare that teaches patients how to manage a chronic disease.” (Disease Management on About.com)
Is that clear as mud?
In today’s world, everything is patient-centric so that doesn’t differ between the three. Obviously, DM is a part of MM, but I rarely hear people talk about MM as a part of PHM which it seems to be to me. But, I don’t think of most MM type programs taking on the macro level change that PHM implies to me. PHM implies things like public health or broad programs like BlueZones. It implies looking at things like plan design, incentives, social trends, workplace culture, and other aspects of change that are necessary to create change and sustain change.
Here’s the Care Continuum Alliance’s full description of PHM (or as they call it here – population health improvement):
Key components of the population health improvement model include:
- Population identification strategies and processes;
- Comprehensive needs assessments that assess physical, psychological, economic, and environmental needs;
- Proactive health promotion programs that increase awareness of the health risks associated with certain personal behaviors and lifestyles;
- Patient-centric health management goals and education which may include primary prevention, behavior modification programs, and support for concordance between the patient and the primary care provider;
- Self-management interventions aimed at influencing the targeted population to make behavioral changes;
- Routine reporting and feedback loops which may include communications with patient, physicians, health plan and ancillary providers;
- Evaluation of clinical, humanistic, and economic outcomes on an ongoing basis with the goal of improving overall population health.
The population health improvement model:
- Encourages patients to have a provider relationship where they receive ongoing primary care in addition to specialty care;
- Complements the physician/practitioner and patient relationship and plan of care across all stages, including wellness, prevention, chronic, acute and end-of-life care;
- Assists unpaid caregivers, such as family and friends, by providing relevant information and care coordination;
- Offers physicians additional resources to address gaps in patient health care literacy, knowledge of the health care system, and timeliness of treatment;
- Assists physicians in collecting, coordinating and analyzing patient specific information and data from multiple members of the health care team including the patients themselves;
- Assists physicians in analyzing data across entire patient populations;
- Addresses cultural sensitivities and preferences of individuals from disparate backgrounds;
- Promotes complementary care settings and techniques such as group visits, remote patient monitoring, telemedicine, telehealth, and behavior modification and motivation techniques for appropriate patient populations.
And, if you read articles about PHM, these macro issues don’t seem to be the focus. The focus seems to be mostly on the technology to accomplish PHM. There are obvious challenges and key success factors there. (Recent commentary on PHM.)
Only 66% Of Medicare Beneficiaries Used Their Free Preventative Care In 2011
Medicare offers people free preventative care which includes a variety of things:
- Abdominal aortic aneurysm screening
- Alcohol misuse screenings and counseling
- Bone mass measurements (bone density)
- Cardiovascular disease screenings
- Cardiovascular disease (behavioral therapy)
- Colorectal cancer screenings
- Depression screenings
- Diabetes screenings
- Diabetes self-management training
- Glaucoma tests
- HIV screenings
- Mammograms (screening)
- Nutrition therapy services
- Obesity screenings and counseling
- One-time “Welcome to Medicare” preventive visit
- Pap tests and pelvic exams (screening)
- Prostate cancer screenings
- Sexually transmitted infections screening and counseling
-
Shots:
- Tobacco use cessation counseling
- Yearly “Wellness” visit
(This list is from http://www.medicare.gov/coverage/preventive-and-screening-services.html.)
Now, while HHS says that over 32M people used these services in 2011, this is only 66% of Medicare beneficiaries. This varies by state with 48.1% of people in Wyoming taking advantage of this benefit while 71.1% of people in Delaware take advantage of the benefit.
I’m not sure of the root cause, but I suspect a lot of it has to do with education. Beneficiaries don’t understand what’s free. They don’t understand how to take advantage of the benefit, and physicians aren’t reinforcing this.
Different Ways To Represent The Same Data
I was just watching the Verizon advertisement where they show data in a few ways. While their charts are all basically the same, it made me think about different ways of representing the same data. We all know that this is an important thing as we evaluate the effectiveness of different programs.
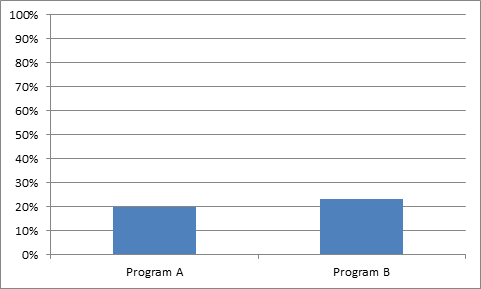
Let me highlight four different ways of representing two data elements. In this case, I’m comparing two programs. The first program (A) had a yield of 20% and the second program (B) had a yield of 23%.
- I could say that Program B was 3 percentage points better than Program A.
- I could say that Program B was 15% better than Program A.
I could show the data in two different charts where I simply change the y-axis.

The Real Bears YouTube Video – Creative Attack On The Soda Industry
This video is a little slower going than I had imagined, but it makes a series of tough points about the soda industry and its impact on our healthcare. See http://therealbears.org for more information.
What’s Possible With Healthcare Technology – Infographic and Health 2.0
I love where the future of healthcare technology is going. If you missed the Health 2.0 Conference this week, you can see a lot of the presentations now online for FREE! It’s very cool.
At the same time, I think this infographic from the Institute of Medicine reinforces some of the key points.
Keys To Long-Term Health – Stop Smoking, Eat Better, Exercise
We should all know this, but not many of us do it.
Infographic: Your Health In One Drop From WellnessRx
I saw a mention of WellnessRx from Health 2.0 and went to look at them. I found this infographic which I think is interesting and reinforcing of the value of biometrics in population health management.
Big Bird Comment From Romney Is Relevant To Healthcare

I keep seeing buzz about the Big Bird comment about PBS from the Presidential Debate from last week. As always, I interpret things differently. To me, this shows Romney’s willingness to make tough and perhaps unpopular decisions (like raising taxes for the Middle Class). At some point, these things may be critical.
Sure…the PBS budget may be small, but at some point, we as a country need to focus on how we cut costs to reduce our deficit. (See US debt clock.)

This reminds me a lot of the discussions we used to have to have as a PBM with employers or labor unions about their benefits. It goes back to the basic framework of “you can’t have your cake and eat it too”. Everyone wants to have a broad network of providers. Everyone wants to have an open formulary. Everyone wants to have the broadest benefits at the lowest cost without increasing their contribution every year.
Just by cutting a drug or a provider from your benefit may seem small, but the savings add up. (Like Big Bird or PBS.)
But, this is the problem we have in healthcare. How do we make enough small decisions to add up to real savings? How do we do this without upsetting everyone and impacting satisfaction (or is that simply life)?
The Future Of Population Health Is Mobile
The statistic that I like to point out is that more people have access to mobile devices than people who have access to toothbrushes. I know that sounds crazy to us Americans, but that’s apparently a global reality (in so much as statistics don’t lie). And, people seem lost without their smartphones so they have them within a few feet of them almost 24 hours a day.
Combine that with several trends, and you can begin to understand why Qualcomm Life predicts that by 2020 there will be 160 million Americans who will be monitored and treated for medical conditions remotely.
- There will be a shortage of doctors (at least in certain geographies).
- Technology continues to be more and more ubiquitous. (Just look at this amazing video)
- Telemedicine is becoming more normal.
- Big data continues to be a huge focus with lower data costs, greater integration, and ultimately more and more predictive models to interpret real-time data.
So, as I pointed out the other day about the value of the mobile data for a healthcare underwriter, that same data can be used to create a systemic intervention system for monitoring and intervening with consumers to drive behavior change. AND, since the data and delivery method is mobile, the interventions can be highly personalized based on when, how, what channel, etc. to improve engagement rates. I can even know who influences your behavior change and how to get them to encourage you to change behavior (peer pressure) or who you monitor and can influence you based on their recommendations.
I’m not sure I’m ready to go as far as Dr. Ron Loeppke from US Preventative Medicine who said
“These mobile apps that are emerging are going to be a predominant part of how health care is delivered going forward.” (Smartphones Take Wellness Engagement To New Levels by Elizabeth Galentine)
BUT, I do believe that over time that this will become the increasingly dominant channel for interventions and behavior change. Ultimately, your mobile phone number may be a more valued data point than your Social Security number.
New Drug Epidemic Causing 3x Deaths Of Cocaine Epidemic
There are so many attention grabbing ways of beginning this post…
- Millions of parents deal drugs to their kids
- 44% of teens have friends who abuse drugs
- An increase in free drugs
- Kids are stealing their parents drugs stashes
- 200M pounds of drugs left in the open for kids to find
- 10 deaths per 100,000 people from drugs
Would you have guessed that all of these are talking about prescription drugs?
The Medicine Abuse Project (at www.drugfree.org) is trying to get this word out and find a way to change this. The basic points of their messaging:
- Safeguard your medications…lock them up and throw extra ones away.
- Talk to your kids about drugs and the risk of abusing legal and illegal drugs.
Infographic: Laughter As Medicine (And Equals Working Out)
I think we’ve all heard this at some point or another although I was surprised by the comparisons to the health values of sleep and working out. I wonder how hard I have to laugh to accomplish that.
Go Patch Adams!

Will You Be Charged More For Not Participating In Wellness Programs?
Thus, the major factors that insurance companies traditionally use to charge higher premiums – such as health status, the use of health services, and gender – will no longer be allowed under the ACA. However, the ACA does permit employment-based health plans to charge employees up to 30 percent more on their premiums (and potentially up to 50 percent more) if they fail to participate in a wellness program or meet specified health goals. [From Kaiser document]
Traditionally, health plans and employers have rewarded consumers for taking some basic action (e.g., $100 for completing an HRA)…although some companies prefer penalties versus incentives.
At that same time, there is some evolution happening here with companies moving from simply paying for an action to requiring participation in a program (e.g., disease management). The next step that a few companies are engaging in is actually incenting or penalizing consumers based on health outcomes. This will certainly open some doors for legal challenges where people will argue that they are genetically pre-disposed to some factor that limits their ability to lose weight or lower their cholesterol or some other measure of health.
But, in one of the first legal challenges in FL, the court recently upheld the idea of rewarding (or penalizing) consumers based on taking a specific action (like completing a biometric screening). With that, I expect companies will be more empowered to take advantage of the fact that under health reform they can charge consumers up to 30% more for their healthcare for either not participating or not achieving a specific health outcome.
With an average monthly premium of $468 per month of single person coverage and consumers paying an average of 21% of their healthcare costs (or $97 per month), this means that a consumer could pay an additional $29 per month (or $349 per year). [If I interpret all of this correctly…if it’s 30% of the total health premium (not just the consumer’s share), then this jumps up dramatically.]
Not surprisingly, employees aren’t real excited about this. In a survey by the National Business Group on Health, 62% oppose charging employees more for health coverage if they do not participate in wellness programs. And, 68% oppose requiring employees to participate in a wellness program in order to qualify for health insurance.
And, according to the survey, the most effective cost control tactic was believed to be Consumer Driven Health Plans by 43% and wellness programs by 19% while 60% of employers plan to increase the premium paid by employees (i.e., cost shifting).
But, if companies throw out a life preserver (i.e., wellness program) to a drowing individual (i.e., unhealthy individual), why isn’t it a reasonable expectation that the individual has to grab it (i.e., participate in the program)?

 November 13, 2012
November 13, 2012 











